Jade’s Stage 2X Classical Hodgkin’s Lymphoma Story
Jade was diagnosed with stage 2X Hodgkin’s lymphoma when she was 21. She went into remission after going through ABVD chemo, then the same regimen without bleomycin (AVD).
Jade also highlights how she got through losing hair after chemo, self-advocacy and survivorship.

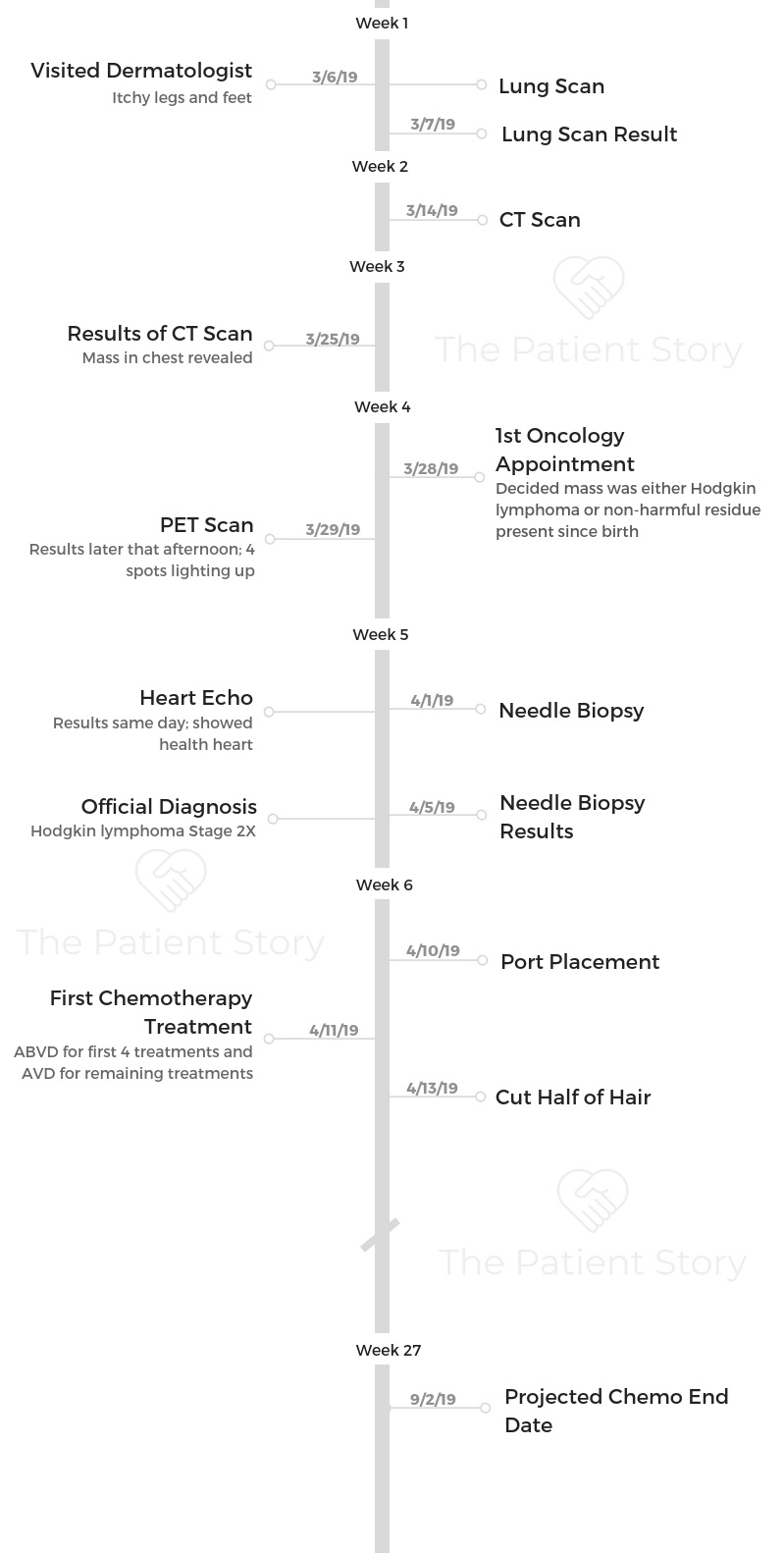
- Diagnosis
- Treatment Decisions
- Chemotherapy
- Quality of Life
- Did you experience hair loss?
- Were you surprised when you lost hair?
- Do you have wigs?
- What has been the worst part of your treatment?
- What has helped you deal with this kind of stress?
- Were there times when you had to advocate for yourself?
- How important is it to have caregivers?
- Relationship with caregivers
- Financial toxicity: paying for cancer treatment
- What kind of help have you had preparing for issues outside of treatment?
- The new normal following cancer
- Message to newly diagnosed patients
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.

My advice would be take everything a day at a time.
When I was first diagnosed, I would always think about what was coming for the next week and the week after that. I would get so stressed over that, and my mind would kind of go crazy thinking about all the appointments.
But once you start thinking about what’s going to happen today, it helps you feel less stressed about everything that’s about to happen.
Jade B.
Diagnosis
What were your 1st symptoms?
I only had one: itching on my legs and feet.
Describe the first visit to the doctor
The first time I saw the doctor was a year ago, and it was for the itching. I was only showing him my legs to see what was wrong.
I was prescribed creams to try out, but they didn’t work out. I saw the doctor a second time, and we tried other creams. They didn’t work.
In March of this year, I saw a dermatologist. She ended up referring me to an oncologist when I got some scans back, because there was something showing up.
What tests and scans did you go through?
I had one CT scan, one PET scan before I started chemo, and one PET scan halfway through chemo.
How long did it take to get those results back?
I got them the same day.
How did you learn the diagnosis?
My doctor called me the day that I had my PET scan. She said there are 4 places that are lighting up.
That’s how I learned about my diagnosis.
I had to go in the next week on Monday to do all the testing. At the end of the week, I was diagnosed with Hodgkin lymphoma.
Processing news of the diagnosis
I was shocked. At first I was really scared. I remembered I cried a lot, but I was more in denial.
For a few days, I didn’t believe it, and it wasn’t until I started chemo that I really realized what was happening. Now I’m fine with it.
»MORE: Processing a cancer diagnosis
How did you break the news to your loved ones?
When I got the call, I was with my mom, so she knew when I was talking with the doctor on the phone. I waited until my dad came back from work to tell him, and I just said, “It’s Hodgkin lymphoma.”
I texted my friends and asked them if I could meet them very soon. I saw most of them the same day or during the weekend, and I told them what was happening. That’s how I told everyone who I’m close to.
»MORE: Breaking the news of a diagnosis to loved ones
Treatment Decisions
How did you decide where to get treatment?
I didn’t. When I was referred to the oncologist, I just went to that hospital. I just stayed there because I liked the hospital.
I could’ve been transferred to my city, but the transfer of the documents and all takes a bit of time. They preferred having me with them, so I stayed there.

Is your hospital a large medical center or a small hospital?
It’s a large hospital.
What are some pros/cons of being in a large hospital?
I like it. Compared to the one in my city, it’s a small one. I’ve been there a few times. But the one I’m going to for chemo, it’s nice because you get a lot of staff, especially in oncology. There are tons of nurses, and it’s really fast.
I feel like even though it’s a big hospital, everyone knows you, and I really like that.
How was your medical team?
They’re so sweet. I really like them. I have 2 oncologists, and they’re kind of young, so it’s really fun.
I see my nurses all the time, and they’re always talking to me because I’m the youngest one there.
I feel like because I’m the youngest, they’re always remembering me and asking me how my treatment is going and if it’s working. They’re really always there for me.
Whose decision was it to do chemotherapy?
That’s what the oncologists said. It wasn’t my decision.
Chemotherapy
Describe your chemo regimen
I did 6 cycles of ABVD chemo.
What is each week like?
I get my chemo every 2 weeks on Thursday. The day that I have chemo, it’s just a regular day.
The week after, I have my side effects, but they’re not that bad. My week off, I just go on with my life, and I hang out with my friends.
ABVD chemo side effects
I’ve had mouth sores, bone pain, sore throat and numbness in my fingers once.
The few days after chemo, my taste buds are kind of weird — everything tastes sour.
How do you deal with these side effects?
My first 2 treatments, I had mouth sores, and I didn’t really know how to deal with them. I talked to my doctor, and he prescribed me a mouthwash that really helped.
I also looked online, and a lot of people said that they would eat ice during chemo and that would help.
Ever since, I’ve been doing that, and it’s really helped. I don’t really have mouth sores anymore. For bone pain, I don’t really have a way of dealing with them. I just take Tylenol, and they go away after a few days.
»MORE: Cancer patients share their treatment side effects
Quality of Life
Did you experience hair loss?
Yes, I am going through that right now. I have been losing hair for a few weeks, but it’s not that bad. I’m probably going to shave it soon because it’s really annoying.
Were you surprised when you lost hair?
I was expecting it, but yeah, I was surprised. I remember I was showering one morning, and I was washing my hair. A few hairs came out. I’m not the type of person to lose hair, so I was really shocked when it happened.
The few weeks after that, I would lose hair all the time. To this day, I’m losing hair all the time. At first I was shocked, but now I want to get rid of it.
»MORE: Dealing with hair loss during cancer treatment
Do you have wigs?
I have 2 wigs and scarves.
What has been the worst part of your treatment?
The worst part, I would say, would be kind of having to pause your life for 6 months.
Especially because I am 21, and I’m studying in school. When I was diagnosed, I was doing an internship, and I had to stop.
I also had to stop work. Pausing your life for 6 months really is not fun.

At first I was doing things, and now I’m getting really bored. I can’t really go out much. I think that’s the part that sucks the most for me, just not doing anything.
What has helped you deal with this kind of stress?
My friends and family really helped me. A lot of my friends are reaching out every day to see if I can hang out with them. Just go out to walk.
I have my “me time,” watching Netflix and reading. That helps, too.
Were there times when you had to advocate for yourself?
Not yet, no.
How important is it to have caregivers?
Really important. I really couldn’t make it if it wasn’t for them. They’re always there for me, and if I ever need to talk, I have them.
They’re always there with me at chemo, and that really helps because chemo is long. Having someone with you is honestly, for me, a necessity, to have someone just to talk with and spend time with.
It really helps take your mind off what’s happening and the treatments and cancer and all of that.
Relationship with caregivers
At first it was hard for my parents, but they wouldn’t really talk about it with me. They would mostly talk about it between them. I think it’s hard for them to really see you go through that. They really want to try their best, and they always, always check up on you.
Reassure your parents that everything is going to be fine. I think that’s what they’re mostly scared of, that something is going to happen.
Just make sure that they’re feeling positive about this and try to be happy when you’re around them. Of course, you can be sad around them, but not all the time because I feel like that makes it worse for them.
Financial toxicity: paying for cancer treatment
I have money saved up and live with my parents, so I don’t have a lot of things to spend money on. At first I was fine to stop work because I don’t work a lot of hours a week anyway.
I went to the government in Canada and asked for the medical leave money. You get paid every 2 weeks for 15 weeks, so that helps.
I’m finishing up in July, and after that I don’t get any money. I think I’ll be fine.
What kind of help have you had preparing for issues outside of treatment?
Every time I have chemo, my dad doesn’t work so he can come with me all the time. For my appointments, my mom works during the morning, so she can always come to my appointments.
We asked for my appointment to be in the afternoon so my mom could come with me. They’re always there for that so they can drive, because it’s not in my city. It’s an hour away.
My parents are always the ones driving because after chemo, you’re not feeling like driving, and they’ve been really helpful for that.
The new normal following cancer
At first it was different because that’s all that’s on your mind.
You’re always thinking about it, and there’s not a day where you don’t think about your cancer. At some point, I got kind of used to it, and I tried to get on with my life as much as I could.
Right now, I’m in remission. Ever since I’ve heard that news, I just don’t think that much about cancer anymore. Of course, I still have my moments where I think about it, and I get sad. I remember I’m in remission. That’s kind of the new normal.
Message to newly diagnosed patients
My advice would be kind of take everything a day at a time.
For me, personally, when I was first diagnosed, I would always think about what was coming for the next week and the week after that.
I would get so stressed over that, and my mind would kind of go crazy thinking about all the appointments and all of that. But once you start thinking about what’s going to happen today, it helps you feel less stressed about everything that’s about to happen.
Don’t hesitate to ask for anything from your friends and loved ones.
They want to help as much as they can, and you don’t need to be shy to ask for anything.

Inspired by Jade's story?
Share your story, too!
Hodgkin’s Lymphoma Stories
Madi J., Hodgkin's, Stage 1B
Cancer details: Most common and most treatable form of Hodgkin lymphoma
1st Symptoms: Shortness of breath
Treatment: 3 rounds (6 infusions) of ABVD chemo
Danielle D., Hodgkin's, Stage 2
Cancer details: Diagnosed at age 25
1st Symptoms: Swollen lump on right side of neck/chest area, continued to grow
Treatment: ABVD chemotherapy (3 cycles = 6 infusions)
Lani S., Hodgkin's, Stage 2
Cancer details: Tumor pressing on heart
1st Symptoms: Appendicitis led to CT scan that found tumor
Treatment: ABVD chemotherapy, 7 cycles
Jason F., Hodgkin's, Stage 2A
Cancer details: Diagnosed at 39
1st Symptoms: Itchy legs, bloated face and “upper trunk,” slow-healing wounds, asthma worsened
Treatment: 6 cycles (12 infusion) ABVD chemo, 18 radiation therapy sessions
Logan A., Hodgkin's, Stage 2A
Cancer details: Diagnosed at age 15
1st Symptoms: Lump in neck & fatigue
Treatment: 4 cycles of ABVE-PC chemo
Helicon K., Hodgkin's, Stage 2A
Cancer details: Found lymphoma cells in adenoid tissue
1st Symptoms: Difficulty breathing with blockage in nose, surgery to remove tissue resulted in discovery of Hodgkin lymphoma cells
Treatment: ABVD chemotherapy (4 cycles), radiation (20 sessions)
Lauren C., Hodgkin's, Stage 2A
Cancer details: Diagnosed at 23 years old with nodular sclerosis, relapsed after 6 months of 1st-line treatment
1st Symptoms: Itchy body, enlarged lymph node over collar bone
Treatment: ABVD chemotherapy and ICE, radiation, and stem cell transplant for relapse
Wade W., Hodgkin's, Stage 2A
Cancer details: Diagnosed at 18 years old
1st Symptoms: Enlarged lymph nodes (around neck), diagnosed at 18 years old
Treatment: ABVD chemotherapy (2 cycles), AVD chemotherapy (4 cycles)
Moe C., Hodgkin's, 2B, Relapse
Cancer details: Diagnosed at 19, relapsed before remission
1st Symptoms: Fatigue, weight loss, night sweats
Treatment: ABVD chemo, DHAP chemo, MINE-R chemo, splenectomy, autologous bone marrow transplant
Fabiola L., Hodgkin's, Stage 2BX
Cancer details: Stage 2 with bulky disease, relapsed after 1st chemo. Remission after 2nd chemo & bone marrow transplant
1st Symptoms: Shortness of breath, dry cough, fatigue
Treatment: ABVD chemo (6 cycles), IGEV chemo, bone marrow transplant, BEAM chemo, brentuximab
Stephanie O., Hodgkin's, Stage 2B
Cancer details: Stage 2 with bulky disease
1st Symptoms: Shortness of breath, dry cough
Treatment: Stanford V chemotherapy (12 weeks, 1 infusion each week), radiation (20 days)
Chelsea B., Hodgkin's, Stage 2B
Cancer details: Diagnosed at 32
1st Symptoms: Lump in neck
Treatment: ABVD chemotherapy
Katee P., Hodgkin, Stage 2B
Cancer details: Accidentally found in x-ray after months of symptoms
1st Symptoms: Night sweats, fatigue, extreme itchiness, persistent cough
Treatment: AAVD chemo, clinical trial w/brentuximab (Adcetris) + nivolumab (Opdivo) immunotherapy
Mara T., Stage 2BX (Bulky)
1st Symptoms: Shortness of breath, back pains, daily migraines
Treatment: 3 rounds of ABVD, 3 rounds AVD, Radiation
Topics: Self-advocacy, mental health
Jade B., Hodgkin, Stage 2X
Cancer details: Diagnosed at 21 years old
1st Symptoms: Itchy legs and feet
Treatment: ABVD chemotherapy (4 treatments), AVD (remaining treatments)
Tylere P., Hodgkin, Stage 3
Cancer details: Mother is a nurse practitioner; suspected cancer
1st Symptoms: Swollen lymph nodes in neck
Treatment: Clinical trial; Chemotherapy, BMT
Kayla T., Hodgkin's, Stage 3A
Cancer details: Possibly misdiagnosed the first time; later diagnosed as grey zone lymphoma
1st Symptoms: Pulled muscle in chest
Treatment: ABVD chemo, radiation, high-dose chemo, stem cell transplant
Erica H., Hodgkin's, Stage 3B
Cancer details: Staged at 3B
1st Symptoms: Intense itchiness, fatigue, night sweats, weight loss
Treatment:ABVD chemotherapy, 6 cycles (12 infusions)
Nicole M., Hodgkin's, Stage 4
Cancer details: Staged 2 then 4 after second opinion
1st Symptoms: Extreme fatigue, persistent itching on lower half of legs
Treatment: 6 cycles (12 infusions) chemo, ABVD then AVD (dropped bleomycin)
CC W., Hodgkin's, Stage 4
Cancer details: Diagnosed at 29, misdiagnosed as mono
1st Symptoms: Achiness, extreme fatigue, reactive rash on chest and neck. Later: chills, night sweats
Treatment: ABVD chemotherapy (6 cycles)
Lia S., Nodular Sclerosis, Stage 4A
Cancer details: Most common and most treatable form of Hodgkin's lymphoma
1st Symptoms: Extreme lower back pain
Treatment: ABVD chemotherapy
Ava O., Stage 4B
1st Symptoms: Trouble digesting, weak immune system, raised glands, night sweats, chest pain, extreme fatigue
Treatment: 6 cycles of ABVD chemotherapy
Topics: Emotional grieving, mental health, letting go
Delishea A., Hodgkin's, Stage 4B
1st Symptoms: Extreme itchiness and dry cough
Treatment: 6 cycles of chemo, radiation, immunotherapy (Adcetris)
Topics: Finding community & support, self-advocacy
Emmanuel S., Relapsed Hodgkin’s
Symptoms: Enlarged lymph nodes
Treatments: Chemotherapy: ABVD, ICE; autologous stem cell transplant; Targeted therapy: Brentuximab
Kelsey R., Hodgkin’s, Stage 2A
Symptoms: Bad leg itching with no rash, enlarged lymph nodes
Treatment: ABVD chemotherapy, radiation
Manda M., Relapsed Hodgkin’s, Stage 2B
Symptoms: Loss of menstrual cycles, iron deficiency, itching, night sweats, tiredness, night terrors, trouble breathing, difficulty concentrating, enlarged lymph nodes
Treatment: ABVD chemotherapy, radiation, ICE chemotherapy, bone marrow transplant
Samantha S., Relapsed Hodgkin’s
Symptoms: Fatigue, cough, enlarged lymph node
Treatment: ABVD chemotherapy (later changed to AVD), Brentuximab, Cyclophosphamide, BEAM chemotherapy, autologous bone marrow transplant
Patrick C., Hodgkin’s Lymphoma, Stage 2B
Initial Symptom: Dry cough, difficulty breathing
Treatment: Chemotherapy (ABVD)




























