The White Ribbon Project Stories
Heidi Nafman-Onda:
Lung Cancer Patient Turned Community Builder
Story 1 of The White Ribbon Project Stories
“I was an only child and felt pretty lonely.”
Heidi Nafman-Onda always knew she didn’t want others to feel that loneliness. It was something she experienced young, and then especially again when she lost her parents.




“[They] died relatively early. My father died of a rare blood cancer at the age of 63, and my mother died of heart disease connected to type two diabetes at the age of 68,” Heidi explains. “Although they looked healthy, you know it wasn’t the best nutrition and no exercise. And the history on my mother’s side of the family was early heart disease. People were actually dying in their fifties. I just thought, I want to do better.”
So Heidi spent 15 years building her own community, performing work as a health enthusiast, educator, and trainer.
“There’s this kind of this nurturing, I guess, character that I have and I wanted to help people who were isolated. Help them not feel alone, and it’s just been ingrained in me since.

It’s just who I am
My way of trying to take care of people or give them the tools to take care of themselves. you know, hopefully i make a difference in their life.”
But at just 55 years old, while living a very active life, devoted to wellness and fitness, Heidi got the scare of her life. A scan for what turned out to be a benign ovarian cyst revealed something troublesome.
That’s when she got the call.
“I was told by a very somber voice on the phone that, ‘I’m really sorry to let you know that you have stage 3 adenocarcinoma of the lung, your prognosis is not good, and it would be a really good idea for you to get your affairs in order.'”

For this wife and mother, the news was as shocking as it was devastating.
“Looking at Pierre, who was with me, my husband, and holding my hands, he just started to cry. And I knew that I was in trouble,” Heidi recalls.
“I didn’t want him to be alone.. I wanted him to find happiness again. So it was a hard day.”
It was hard to break the news to her family, and even harder to tell everyone else. She describes the feeling of defensiveness that arose when she had to share her lung cancer diagnosis.
“I felt like, why do I have to explain this? I mean, any other cancer people have empathy and compassion for you and say things like, ‘Oh my gosh, I’m so sorry,’ and, ‘How can I help?’ Versus, ‘Well, I didn’t know that you had a smoking history.'”
Heidi had never smoked, but still questioned why she felt these feelings of shame. She realized she didn’t see many others talking about their own lung cancer diagnoses.
“And as time went by, the more I learned about lung cancer and the increasing rates, specifically in people without smoking histories or people who had smoking histories but quit many, many years ago. They were getting lung cancer. And then [I] learned that it was the number one cancer killer, you know, more than, you know, prostate, breast and colon combined.”
So on August 1, 2019, Heidi decided to finally share her lung cancer diagnosis, starting with a post on Facebook.
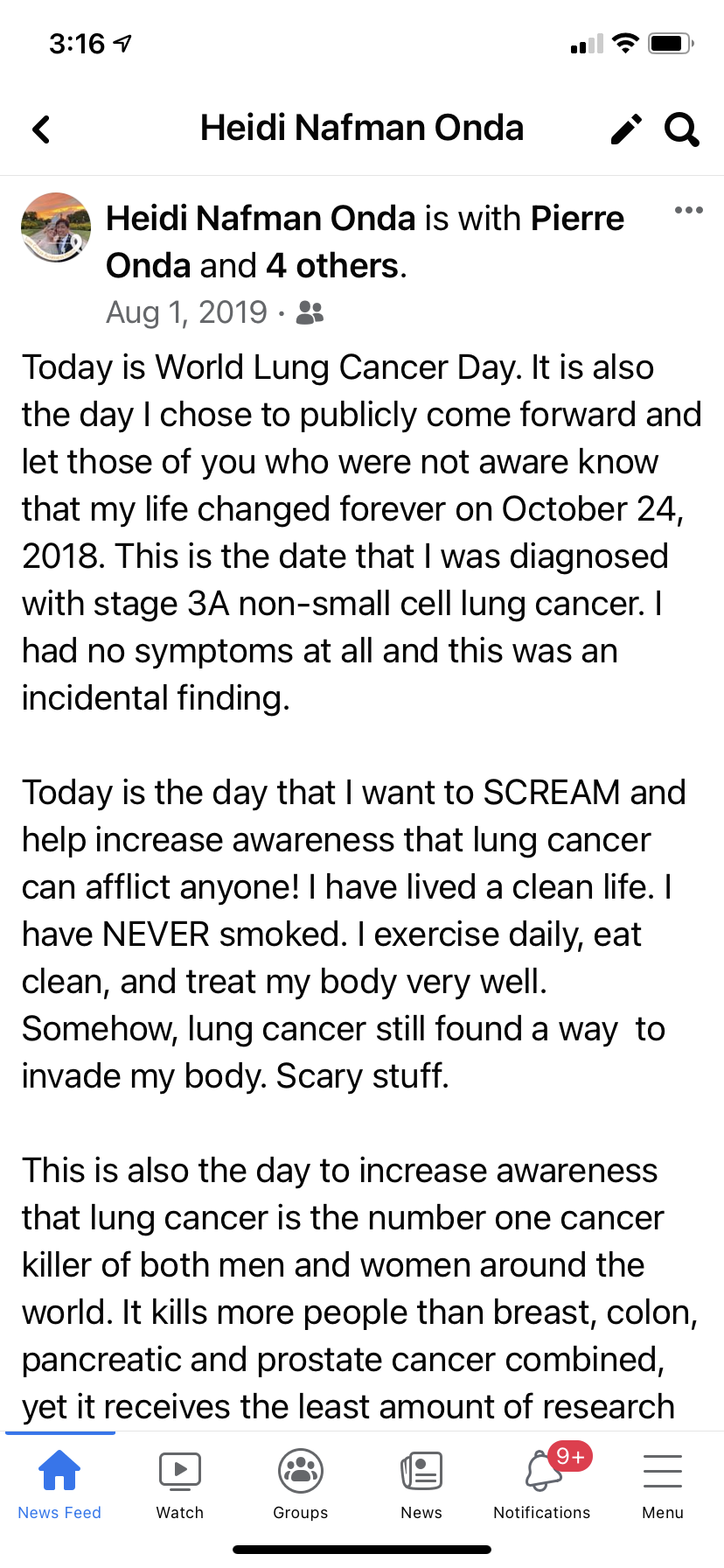

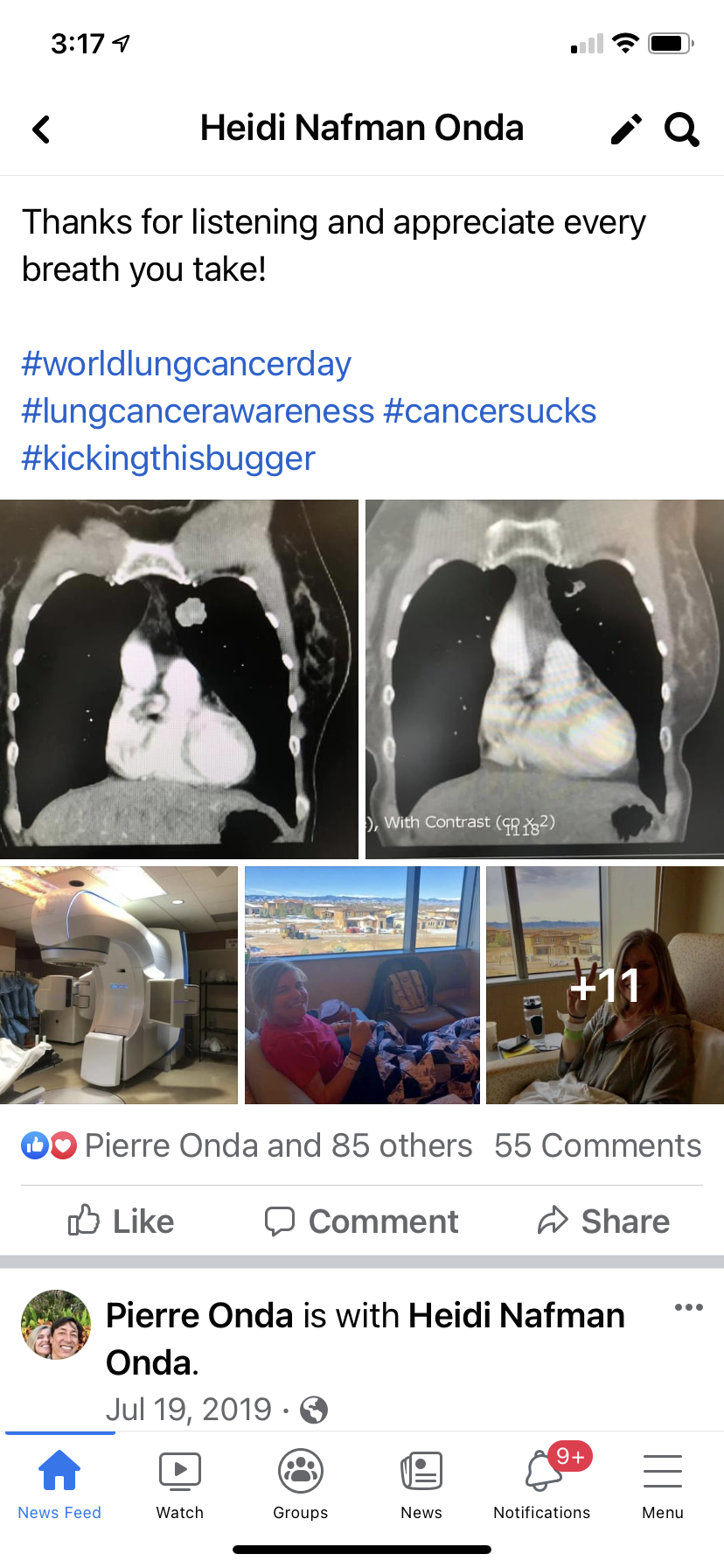
“To say that I had lung cancer and look at me, I’m training for a a big bike race or a fundraising bike race, not to beat anybody, but just to raise funds for cancer research in general. I don’t look like I have lung cancer. I don’t feel like I have lung cancer, but I do.”
And if it could happen to me, it could happen to you.
Anyone with lungs can get lung cancer. And no one deserves it.
It’s a message Heidi wanted to share with the world, but she says she unexpectedly came up against a wall, experiencing a hard time finding support for spreading awareness in lung cancer.
“I kept thinking to myself, so why are cancer centers across the country not talking about this with the growing numbers, you know you really had to dig to find this information?” Heidi says. “I was just basically told, ‘We just don’t do anything,’ and references to doctors wearing white coats and white lights in the parking lot. I just felt so humiliated and disrespected. I just had a meltdown.”
So once again, Heidi decided to create her own community. She started with an iconic symbol that would signal to everyone touched by lung cancer:
You are not alone.
Regardless of smoking history, lung cancer stage, age – everyone is in it together.

“To find out you have a terminal cancer diagnosis or any disease that’s terminal, it’s overwhelming. My head was spinning. It was surreal. It was, how could this be happening?” Heidi recalls. “And then simultaneously to be put to shame. Why is that okay to do to somebody? To make people feel like they somehow made this happen to themselves? There’s no empathy for you. I thought, how cruel and awful… I care about them, whether they lived a life of healthy habits or if they didn’t, they’re humans. We all matter.”
That’s how The White Ribbon Project was born. Heidi’s husband Pierre created the very first ribbon made out of wood. It went straight onto their front door.
“I wanted it big, so I could literally scream from my front door that I had lung cancer. I wasn’t ashamed of it.”
One year later, The White Ribbon Project has created and delivered more than 3,000 white ribbons and counting. They’re in almost every state and even around the world, in:
- Canada
- Philippines
- Ireland
- The Netherlands
The White Ribbon Project movement includes anybody: any subtype, stage, age, patients, survivors, caregivers, medical center physician and staff, researchers, and so much more. But that medical industry support has been a critical piece, with the group now in more than 70 cancer centers, including 33 that are NCI-designated comprehensive cancer centers.








“With about 235,000 people diagnosed in the United States every year and about 130,000 of them not making it for a year. This has been a silent epidemic, a hidden epidemic.
“This ribbon is somehow giving people the confidence to stand up and tell their stories. It’s making them vocal and visible. That’s what we had in the breast cancer movements in the early days and the same thing with HIV AIDS, it’s the same recipe.
“We need people to stand up, tell their stories, humanize this which they are doing, and the medical community to stand with us and validate the fact that anyone with lungs can get lung cancer and they are doing it.”








Part of the shifting narrative also sheds light and hope on lung cancer diagnoses, even advanced cases.
“Three years out, and I’m living a very high quality life… so there is hope that it is worth getting screened and it doesn’t to be a death sentence.”
Heidi looks forward to continuing to grow The White Ribbon Project, along with Pierre, who has tools in hand.
Her objective remains the same as the one she sought in childhood: helping to build a community for all, so not one person feels alone and left behind.









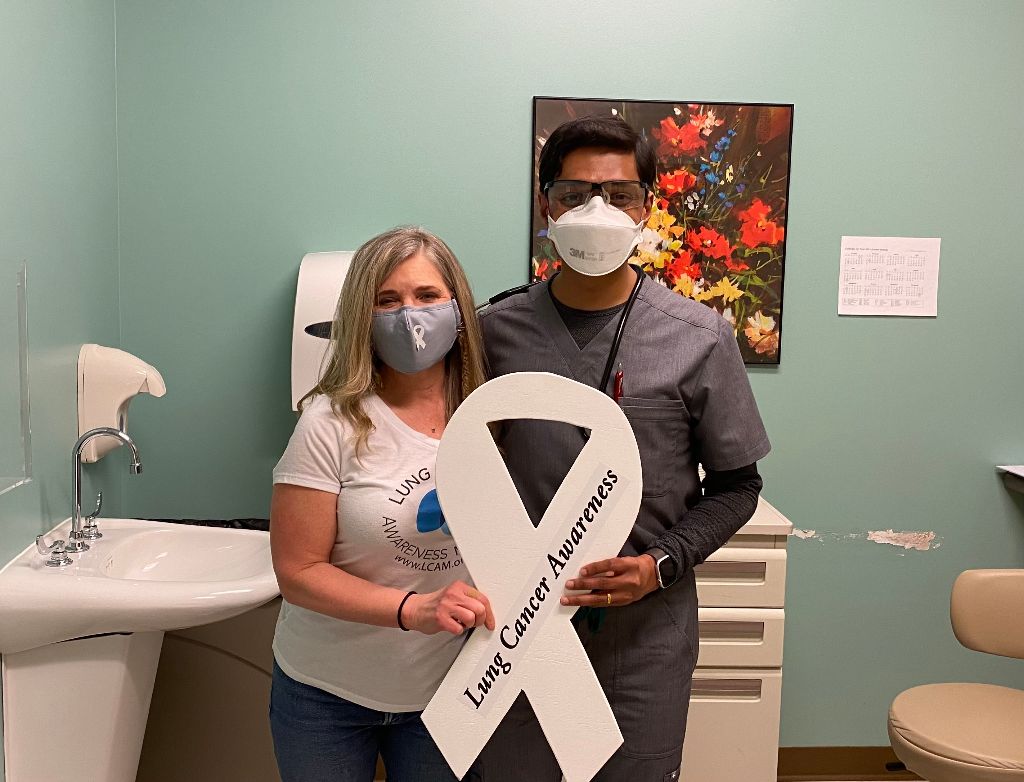
“As long as people want these ribbons, we will make them and we will figure out the rest. We will figure out how we can sustain this and get people to learn how to make them.
And now we have a movement.
Heidi Nafman-Onda
→Back to The White Ribbon Project Stories

Inspired by Heidi's story?
Share your story, too!
More non-small cell lung cancer (NSCLC) stories
Michelle W., Non-Small Cell Lung Cancer, EGFR+, Stage 2B
Symptoms: None; discovered by chance during a check-up for persistent head and neck pain
Treatments: Surgery (lung resection), chemotherapy (upcoming), targeted therapy (upcoming)
Kelsey D., Non-Small Cell Lung Cancer, EGFR+, ALK+, Stage 4 (Metastatic)
Symptoms: Severe back pain, falling due to collapsed spinal vertebrae
Treatments: Radiation therapy, targeted therapy (tyrosine kinase inhibitor, osimertinib), surgery (spinal fusion surgery), chemotherapy (through a clinical trial)
Megan F., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Chest pain, anxiety, shortness of breath, arm pain and swelling, back pain
Treatment: Targeted therapy (lorlatinib)
Roxanne C., Non-Small Cell Lung Cancer (NSCLC), Stage 3
Symptoms: None; incidental finding
Treatments: Surgery (lobectomy), chemotherapy (cisplatin), radiation therapy, targeted therapy (tyrosine kinase inhibitor/TKI)
Natalie B., Non-Small Cell Lung Cancer, Stage 4 (Metastatic)
Symptoms: Extreme fatigue, severe cough
Treatments: Chemotherapy, immunotherapy, clinical trials, radiation therapy, surgery (double lung transplant)





One reply on “The White Ribbon Project Stories | Heidi Nafman-Onda”
My 64 yo husband, just diagnosed with inoperable Stage IV adenocarcinoma of Lung upper left lobe 8-10 cm with difuse Mets to peritineum and omentum. Awaiting visit with Oncologist. Any suggestions?