Scott’s Stage 3 Refractory Multiple Myeloma Story
Scott shares his story of stage 3 multiple myeloma, IgG lambda. He details undergoing extensive treatment, including a kyphoplasty, clinical trial regimen with targeted therapy and immunotherapy, a stem cell transplant, and consolidated chemo.
In his in-depth story, Scott also highlights dealing with a refractory cancer, the importance and impact on his marriage, and how he managed parenting with a cancer diagnosis.

- Name: Scott C.
- Diagnosis:
- Multiple myeloma
- IgG lambda
- Most common type of heavy chain produced in myeloma is IgG
- Staging:
- 3
- 1st Symptoms:
- Pain in hips and ribs
- Night sweats
- Weight loss
- Nausea
- Treatments:
- Surgery
- Kyphoplasty
- Clinical trial: KRd
- Targeted therapy: Carfilzomib (Kyprolis)
- Immunotherapy: lenalidomide (Revlimid)
- Steroid: Dexamethasone
- Stem cell transplant
- Consolidation chemo
- Darzalex (daratumumab), Pomalyst, & Dexamethasone
- Surgery
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Diagnosis
What were your first symptoms?
Summary: Pain (hips, ribs), night sweats, weight loss, nausea
Prior to diagnosis, I had symptoms. It’s interesting because I had several. I just didn’t connect them.
The main thing was pain. I first noticed some pain in my hips over the summer. I had always had body aches because I was a carpenter.
Then in December, we just didn’t put it off anymore because it was in my ribs by then. The pain radiated up the side and in the front, and come to find out, it was a broken rib and a tumor.
I also had night sweats. I didn’t connect that to anything. I ignored those. I was losing weight. My weight has fluctuated all my life, so I didn’t think much of that either. What did worry me was the nausea.
I had constant, pervasive nausea. I wasn’t vomiting, but I always felt sick to my stomach. I didn’t eat much. The pain was the worst, though.
I went to see an orthopedist. He called me and said, ‘We didn’t find much, but we did find a broken rib.’
I said, ‘What?’ I had just had pneumonia and sepsis, and I had just seen films of my ribs two month prior. There were no broken ribs before.
How did your doctor break the news to you?
I went down there to see the X-ray at the orthopedist in person, and I took a picture of the scans. I went to my primary right after. He said he thought this was different than the pneumonia.
He didn’t like what he was seeing. I said, “I see a mass,” and he said, “I do, too.”

First scan
He went into his office and set up an appointment for a CT scan of my spine the next day. About 45 minutes after I got home, he called me. I was infested.
He told me it was really bad. He walked through everything and told me where the mets (metastasis) and tumors they could see were and where they had spread.
There was no mention of a primary, and when you get a diagnosis with multiple mets and no primary, your brain races. I felt so bad. I felt physically horrible. After learning that, I felt like I had to get ready. It looked like I was going to be dead in a month. I was getting worse by the day.
My doctor canceled his Christmas travel plans, and he stayed in town to figure out what it wasn’t. At a time when everyone else was on vacation, he managed to rule out raging lung cancer. He knew it wasn’t in my brain, and he knew I didn’t have prostate cancer or liver cancer. He was ordering all kinds of tests, running them and reading them.
A couple of days later, he called me and said, ‘I know exactly what you have. You have multiple myeloma.’
Describe the bone marrow biopsy
It’s not that invasive overall. It’s not like you’re sliced open or anything, but a needle is inserted into your pelvis. While they do a good job of numbing you and all that, it’s a horrific procedure. There’s no way to sugarcoat it.
I can’t have them done unless I’m anesthetized now. The first and only time they did it while I was awake, they gave me all the pain medicine they possibly could, and it was still really painful for me.
I don’t want to scare anyone because a lot of people tolerate it really well, and it’s just pressure for them.
I just had so much going on that it was really painful because, as we know now, the pelvis is the epicenter of my disease. They were poking the lion, so to speak.
I clenched my teeth so hard during the biopsy that I chipped a tooth. We were all freaked out. Now, no one asks, and I just get put under.
It’s a fairly simple procedure technically, but it’s intense in ways that I don’t think gets enough attention, because for medical professionals, it’s routine.
Be prepared, but know that it doesn’t last long. With prep and everything, it’s only about 45 minutes long.
Processing the multiple myeloma diagnosis
It was a relief because up to that point, I thought that I had something that was moving faster than the myeloma was moving. I had conversations with my kids.
My wife and I talked about it a little bit, but we just know things at this point. We’ve been together 30 years. We were set no matter what. She was on board for whatever.
When I first found out, my first instinct was to call my wife. She was out Christmas shopping, and she loves doing that, so I thought, ‘I’m gonna let her shop. This is the last time she can ever Christmas shop without knowing this.’
When she came home, she instantly knew something was wrong. I asked her to sit down on the couch. I told her everything. I collapsed. I told her I was sorry.
She shushed me and took my face in her hands. She said, “I’m all in. Whatever this takes. You have two jobs: fight as hard as you can and stay alive.”
I don’t make many promises to her. I’m a high-percentage guy. But I promised her that I would do that.
I was relieved because I had been researching myeloma already anyway. I suspected that it might be myeloma.
My defense mechanism is to learn as much as I can about my disease, so that’s what I did. I knew we had a direction and a referral to a specialist, so that was amazing.

Targeted Therapy & Chemotherapy
Meeting a myeloma specialist
I met Dr. Perkins, the myeloma specialist. From the very first appointment, I felt comfortable with him. He’s a fantastic physician. He now runs the show.
I love my primary, Dr. Turner. He’s been my doctor for 15 years. He said he’d loved to treat me, but he didn’t know how.
He still watches over everything, though. He gets every piece of paper that’s generated for me. I see him once a month still because he manages my pain.
The plan going forward after diagnosis came from Dr. Perkins. He explained all my levels, the plan and all the options.
My levels were pretty high. I don’t think I had 6 months left because of the way it was progressing.
Dr. Perkins suggested what was the gold standard of care at that point, and that was a triple therapy followed by an autologous stem cell transplant. He also alerted me to an opportunity for a clinical study. I elected to pursue that because my interests coincided with the greater good.
Describe the targeted therapy clinical trial
I started my targeted therapy clinical trial first. Everybody calls it chemo because it’s easier, but it was immunotherapy. I didn’t have my port in yet because everything was moving too fast, but we went ahead and started that. Then I had the port in on Valentine’s Day, and I’ve had it in ever since.
I got the golden ticket with this trial. I had 6 infusions in 3 weeks of carfilzomib (Kyprolis), and I went from knocking on death’s door to almost stable.
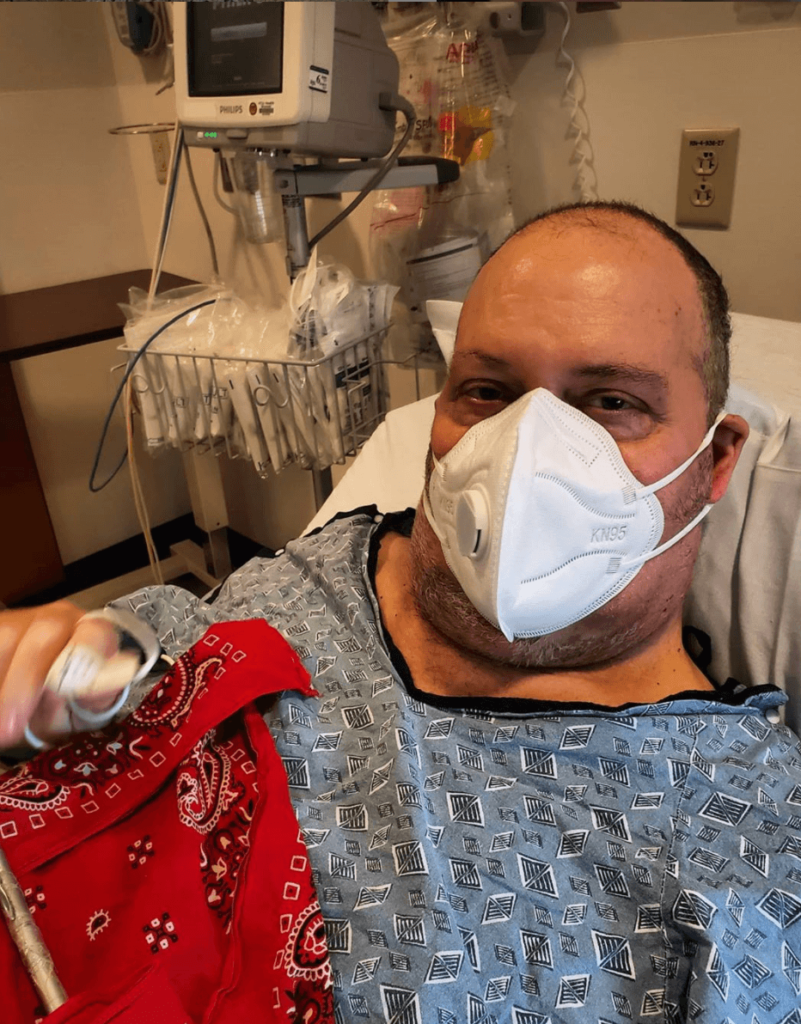
It was 50 mg twice a week. They took about half an hour or so. I also got pre- and post-medications, as well as fluids, so that added time. It always ended up about 3 or 4 hours in total for infusions.
I was taking 25 mg orally of Revlimid (chemo) every day, and I was getting 40 mg of dexamethasone (steroid) on the first day and 4 mg the second day. I did all that from February to June. I stopped when they were happy with the way the numbers were moving to have a kyphoplasty. We squeezed that in and moved right into the stem cell transplant in July.
»MORE: Learn more about immunotherapies
What side effects did you experience?
The drug carfilzomib, which I’m on again now, is cardiotoxic. The toxicities are cumulative based on exposure, so there’s that. It took a long time for that to manifest, but it’s happening now. I didn’t see any of that initially.
I had a lot of hypotension, which was the opposite of what we thought was going to happen. I had some minor diarrhea.
I think the myeloma causes all my nausea. I had nausea, but I don’t think it was the drugs.
Dexamethasone is a steroid, and I was on such a high dose. That caused my heart to race. We’ve modified my dosage a bit now that I’m on it again. I get hiccups. I retain fluids. It interferes with sleep a lot, especially at the high doses, but it’s more manageable now.
»MORE: Cancer patients share their treatment side effects
Surgery & Recovery
Describe the kyphoplasty
Really, there wasn’t any prep for me to do. The only thing was the regular NPO (nothing through the mouth) after midnight, so I couldn’t eat anything beforehand. It’s a very simple procedure.
They made what they call a snakebite incision in your spine. I was on the table for 15 minutes for the kyphoplasty.
Then, in the same surgery, he went in on a different level and worked on a lesion that was right up on the spinal cord. He burned it using radio waves.
It’s sci-fi stuff. It’s so neat. He couldn’t get my margins, but he took a lot of it. He got as close as he could.
I’ve never been worried about surgeries. I wasn’t nervous at all. I knew what was going to happen already. I was actually excited.
Surgery meant I was doing something. Surgery was a counterpunch to the myeloma, so I was ready for it. Plus, it was taking care of a lot of my pain, so it was a win all the way around.
»MORE: Read more patient experiences with surgery
Recovering after the kyphoplasty
Recovery wasn’t bad. I was a little sore for a few days, but I was up and moving instantly. Within 30 days, I didn’t even know I had the surgery. I just knew that I felt good. After surgery, I started prepping for the transplant.
Stem Cell Transplant (SCT)
What was the preparation for the transplant like?
Days and days of testing. They test everything. It’s a very intense procedure, and if you don’t meet certain levels, it’ll kill you. They give you a lethal dose of chemotherapy, and if you’re not strong enough, you won’t make it.
It wipes out every bit of your bone marrow in your whole body. It’s very strange to volunteer to put that in my body. I made all the requirements on my test results, though.
I was high risk on the cardio and pulmonary side of things, so they had to just watch me and treat me a certain way for potential side effects. That prep work took about a week.
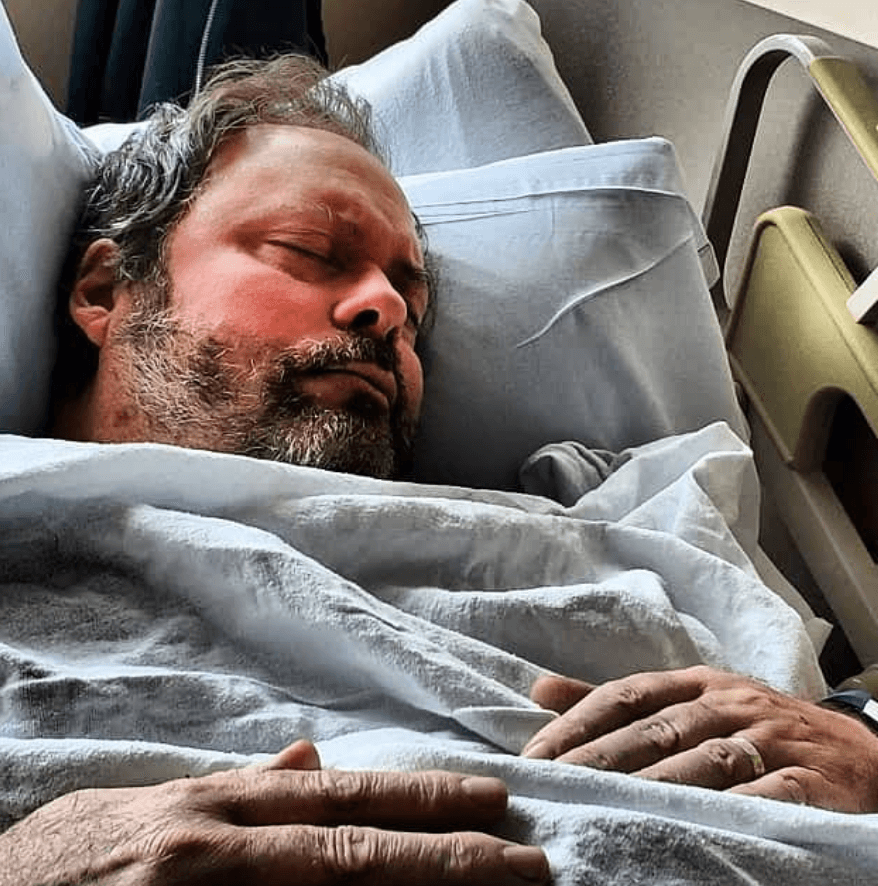
Then they took my stem cells. I had to have a PICC line in for that. It was like a garden hose. They removed all my blood over the course of the process several times, and the machine spins out your stem cells. It’s a 2-day process usually.
I had Neupogen before that. It stimulates your bone marrow to make lots and lots of stem cells. That’s extraordinarily painful. I felt my skeleton in 3D. I could feel it all. That’s the worst pain of the whole thing.
The second day, I felt better. Heating pads helped. I made enough cells for two treatments. I had one to use and one to keep for emergencies. It’s still there in case I need it. I don’t know how much it’ll help me if things go south, but at least it’s something.
Stem cell transplant and recovery
I was admitted on the 16th of July. That day, they hit me with chemo. That was unpleasant. I developed angina within a couple of hours. They had to monitor me and check my levels frequently.
I was getting hot flashes, and every day I felt a little bit worse. I was in the hospital for 15 days. I never needed a transfusion of cells. My platelets dropped pretty dangerously low. My eyes and my gums started to bleed. My entire mucus membrane slid off. I couldn’t eat anything really, but you have to eat what you can.
I had nausea, but it was manageable. I had 3 different nausea medications running 24/7. That was a suggestion from some other people, and it helped so much. I want to be that for others. That’s why I want to be open about my experience.
About halfway through my hospital visit, that’s when my platelets bottomed out. I got preserved platelets and found out I was very allergic to the preservative. I looked like a red cheetah and then turned into the Thing. It didn’t hurt or itch, but it was crazy. It itched later when it healed.
I was so weak. I would lie there and think about getting up and just continue to lie there. They only thing that gets you into gear is you have to go sit on the toilet. That would get me moving because I was going to crap myself if I didn’t. The diarrhea was unreal.
I couldn’t take the shame. The nurses kept saying, ‘We love poop! Don’t worry about it.’ I just couldn’t help it. I was so freaked out.
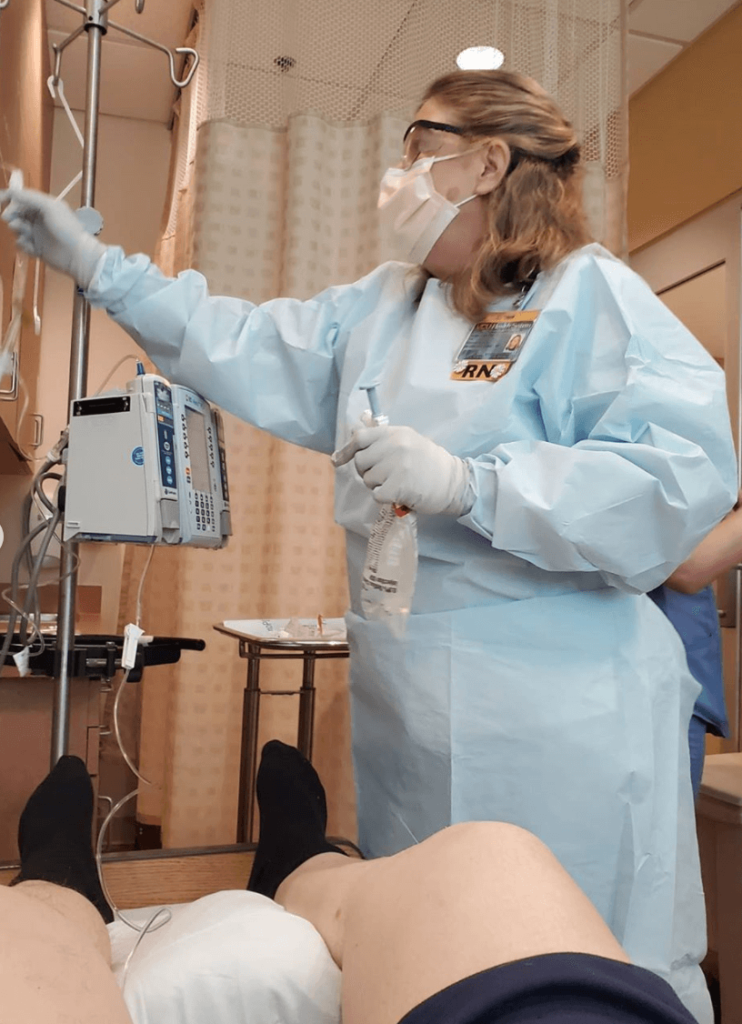
The need for a caregiver
My wife would come after work and stay with me. She would help me shower while the nurses changed my bed. All I could do was stand there, and my wife had to shower me.
I’ve never been that weak before. It was hard to do anything. It was hard to breathe. I just had to keep going.
I walked because that’s what they told me to do. Every myeloma patient I talked to told me to listen to my nurses and walk.
I progressed well enough that I was allowed to leave early. Like I said, I was there for 15 days.
I was on 100 days of seclusion because you can’t be exposed to fungus or mold or anything.
I went to the clinic every day because you’re struggling to get nutrients. I needed magnesium a lot.
After 32 days, they said, “You don’t need to come back every day.” I was allowed to come back for 3 days a week instead of 7. We did that one week, and then they said I could just come twice a week. I did that for 30 days. At 67 days, I hit my deadline and was released from the program.
I felt so good. I had forgotten what it felt like to feel good. I thought the transplant was the best thing that ever happened. Even though it didn’t pan out the way I hoped, I still feel that way.
»More: Read stories from cancer caregivers
Refractory cancer
For a little while, I felt great. I just stuck with the protocol. I couldn’t do certain things still, but I got along fine.
100 days after the transplant, they did another biopsy. We learned that my numbers hadn’t moved despite the chemotherapy.
I was out-of-the-bag refractory at that point, and my doctor suspected it was to all types of chemo. We haven’t tested it, but he’s reasonably sure.
I have a particularly adaptive myeloma. While I was on carfilzomib, it was figuring out how to survive. I went on a consolidation treatment, which was a disappointment. He put me on Darzalex, Pomalyst and dex.
The Pomalyst jacked my neuropathy sky high. I was willing to deal with that if it was going to save my life.
Anything that doesn’t put me in the ICU and gives me more time with my wife, I’m gonna do it. It wasn’t working, but we didn’t really give it a chance, so I went back on Revlimid.
I couldn’t hardly take the Darzalex. I got just about everything you could get from it. It took me 13.5 hours.
They had to pump me with so many drugs just to get me to sort of tolerate the Darzalex. Darzalex didn’t do anything for me.
We weren’t able to slow the progression of the disease with the transplant or consolidation chemo. My lesions and mets were progressing. I was officially high risk.
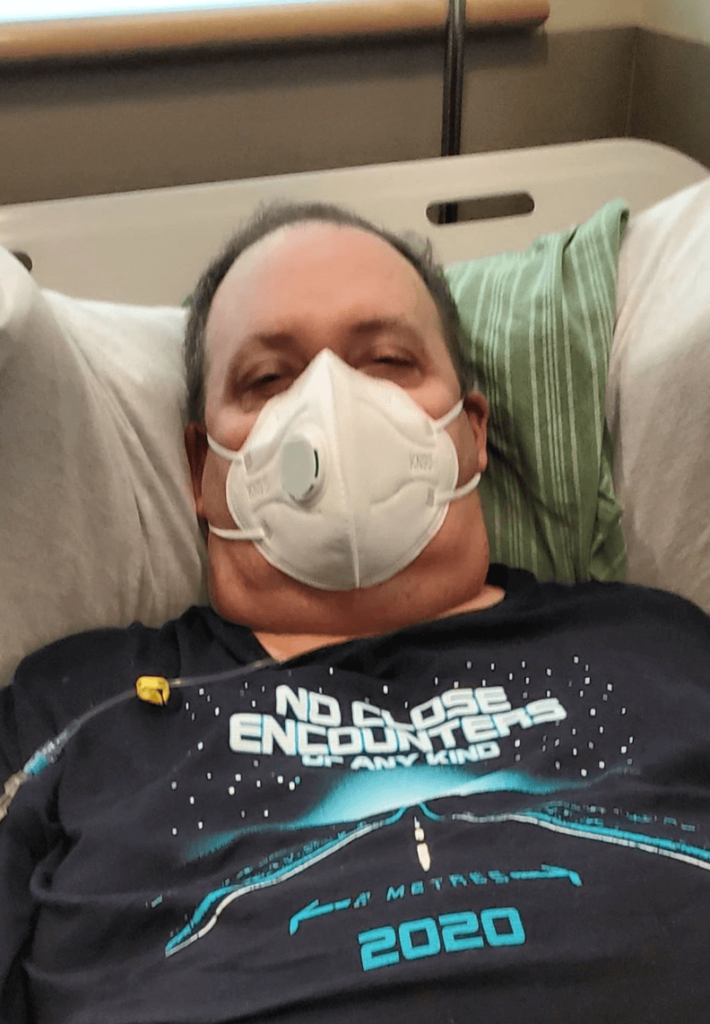
Reflections
What helps you move forward?
No one gives it to me. It’s who I am. I have always believed that I could impact my reality. I never could be someone to throw my hands up. I’ve had a lot of adversity in my life, so I’ve been preparing for this. I was well suited for cancer to come at this phase of my life.
In many ways, cancer has been a blessing to me. I know people go berserk when they hear that, but it’s true. I’m not saying there’s not a whole lot that’s bad, but when you put it on the scales, is what you got worth what you paid?
For me, the answer is yes.
Positivity is my magnetic north. It’s not a simplistic approach. It’s a very nuanced response. There are people I call the “Positivity Taliban.” They want to tell you that you can never feel anything negative and have to squash reality. That’s not true.
You need to feel what you need to feel. You need to process your feelings because that ability makes you stronger. You won’t get anywhere by suppressing them. You should feel sad. You shake hands with sad. You give it a cup of tea and sit down with it, but you just don’t let it move in with you.
Feel it, and when you have the cathartic moment of watching the sun come up the next day, that’s your cue. You have to get up and get going because you have things to do.

My support system keeps me going. My wife. My wife is 90% of why I’m alive. I have my wife, my daughter and my son. At first, everybody wants to help you. Eventually, they drift off in good and bad ways. You can’t get mad about that. It just happens.
When people say, “F you, cancer,” it doesn’t resonate with me. I don’t think anger is a good emotion. I think it’s toxic. I love my cancer away. I love myself, and it’s part of me. I don’t hate it. I could do without it, but I don’t hate it.
Light and darkness can’t exist in the same space. So, when you fill yourself with light, you’re driving the darkness out.
Positivity is a self-perpetuating thing, too. There is always an aspect that isn’t as bad as the rest. If you focus on that, you’re making it easy on yourself.
I get a lot of people telling me in very specific detail how my story has helped them. I love that because it means that something great is coming out of this.
»MORE: What kind of support cancer patients say helped the most
How has your wife handled the tough moments?
She is everything to me. She always has been. Everything that’s good, decent and kind in my life is from her.
My life is divided into the period before her and the one with her. I knew that I would marry once, and she’s it. She’s a person I trust with everything.
We have 30 years under our belt. I said I was well suited for this, but she was, too. We’ve had a lot of time together.
She’s an inordinately strong person, but she’s stoic. She’s never going to complain, but I know her well enough to know when she’s hurting.
We just don’t dwell on things. She’s never read any of my IG posts because she says, “I lived it. Why would I want to read it?” She’s very powerful. She recharges with me.
We have a cabin we inherited from her dad. It’s pretty incredible. We go there when we need to get away. We have a landline, but there’s no cell phones, no internet, no neighbors within visible distance. It’s amazing.
We do things that are important to us. She and I steal moments together all the time. We’ve always loved driving around at night. We’ll drive up to the pharmacy to go pick up my meds and turn on some jazz. We get 20 minutes sitting in the car holding hands. We’re best friends. She comes home and tells me about her day, and I listen. She values that.
I know how to help her unwind. Being able to come home and not have to cook is helpful for her. It’s a team effort really.
We work so well together. We’d overcome so many things. We just put it in the same box with everything else we’ve overcome.
We don’t talk a lot about what’s going to happen, but we did have to settle a few things. I told her, “We don’t have to talk about this much, but these are the things that are important to me.”
I told her what I wanted done with my body. I want my ashes to be extremely close to hers. We did that for her parents, and I told her that’s what I wanted.
I made sure she knew I wasn’t avoiding the topic or ignoring it, but it was more that we just didn’t need to talk about it, and she agreed. We’re more focused on me living and doing things that we can still do now.
She knows I don’t want to be in pain. That’s always been my deepest, darkest fear. I don’t want to die like an animal. I want it to be a happy thing. I want to be surrounded by my family. I want people to be joking. If I have breath, I’m going to be cracking up because that’s me.

Advice for other couples going through cancer
Trust each other. Give your partner the ability to live up to what you think they can do for you. Trust them to do the right thing. Give them credit, but be prepared to help them understand you.
Yes, they’re your partner, but they’re still an individual. Don’t hold back with your honesty, because how can you expect someone to react to you appropriately if they don’t have the full story?
Trust them enough to lay everything out on the table. Don’t be afraid to lean on each other. Be open. My wife recognizes when I’m focusing or dwelling on hurtful or negative things. She never invalidates me, but she gently reminds me. She asks if I want to be doing and thinking the way I am.
A lot of communication depends on the way you frame things. You don’t want to be judgmental. Be careful with your language. Tell them you love them every day.
»More: Marriage and cancer

How has myeloma affected you as a parent?
I’m trying to teach my kids that death can be a beautiful thing and something that we can control.
I want them to admire me. I want them to be proud of me and how I handled this.
I want them to know that I never let it beat me or change me. I want them to see that I haven’t changed myself in the face of something catastrophic. I think I’ve accomplished those things so far.
My daughter is very strong. I’ve had conversations with my kids about how they’re going to need to step up and take care of their mom when I pass because she’s not going to be okay for a while.
My daughter is strong like me. She’s going to have to step up for her brother and mom.
Everything has reversed. She is now my parent.
I laugh about it and say she’s my mommy. I’m on her phone plan. She got me a new cell phone. She told me, “Dad, don’t poke your eye out with that thing!”
I think she likes to be present. It helps her not to worry. Especially in the beginning when I was really sick, she was there for everything. It would’ve been harder had she not been there.
»MORE: Parents describe how they handled cancer with their kids

What is your advice for someone who has just been diagnosed?
The number one thing I want to say is it will get better. You will have no reason to believe it, and you may not understand it, but I promise you it will.
I’ve been in that spot. I know. I have your disease. I’m your tribe. This is our flavor, and we share it. I’m over here now. How you get here is going to be different than the next person, but there is a way for you.

The second thing is just to worry about today. Tomorrow will take care of itself. At most, worry about today and tomorrow. The rest will take care of itself. You have to live life in smaller bites, because it’s too much.
Learn everything you can about your disease. Don’t be afraid of it. You get power in knowledge. How can you make decisions — and you’re going to be asked to make many — if you don’t have all the information?
For your research, stay away from Facebook. Facebook is a great thing for certain things and for many things, but it is mostly a cesspool of misinformation, and so are random Google searches. Don’t be afraid of going to the actual source. Go to the actual articles. Talk to actual patients.
Believe in yourself. Be kind to yourself. You are stronger than you know. Forgive yourself for how you feel. Accept it all. Eat well. The rest will fall into place.

Inspired by Scott's story?
Share your story, too!
Multiple Myeloma Stories
Clay D., Relapsed/Refractory Multiple Myeloma
Symptoms: Persistent kidney issues, nausea
Treatments: Chemotherapy (CyBorD, KRd, VDPace), radiation, stem cell transplant (autologous & allogeneic), targeted therapy (daratumumab), immunotherapy (elotuzumab)
...
Melissa V., Multiple Myeloma, Stage 3
Symptom: Frequent infections
Treatments: IVF treatment & chemotherapy (RVD) for 7 rounds
...
Elise D., Refractory Multiple Myeloma
Symptoms: Lower back pain, fractured sacrum
Treatments: CyBorD, Clinical trial of Xpovio (selinexor)+ Kyprolis (carfilzomib) + dexamethasone
...
Marti P., Multiple Myeloma, Stage 3
Symptoms: Dizziness, confusion, fatigue, vomiting, hives
Treatments: Chemotherapy (bortezomib & velcade), daratumumab/Darzalex, lenalidomide, revlimid, & stem cell transplant
...
Ray H., Multiple Myeloma, Stage 3
Symptoms: Hemorrhoids, low red blood cell count
Treatments: Immunotherapy, chemotherapy, stem cell transplant
...




