Go With The Good | Cancer Friends
Featuring Katie and Pete Mang

“Cancer Friends,” hosted by Andrew and Esther Schorr, highlights stories and lessons from cancer survivors and their support system. For more “Cancer Friends” episodes, watch on our video channel here!
This segment focuses on Pete and Katie Mang, a young couple whose lives turned upside down after Pete was diagnosed with glioblastoma, a rare brain tumor. Faced with the burden of uncertainty for their family, they decided to always focus on the good.
Navigating financial toxicity and treatments was difficult, so they created Go With The Good to help other families find resources and support after a cancer diagnosis. Pete and Katie share the lessons they’ve learned along the way, including how they approach parenting with an uncertain cancer diagnosis, living with gratitude and finding support for the caregiver.
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
A bit of the blessing of the uncertainty is it has had us focus on what’s really important.
Katie Mang

Every single time that we do something as a family with the kids, it’s special no matter what we do.
Pete Mang
Introduction to Katie and Pete Mang
Andrew Schorr, The Patient Story: Hello and welcome to The Patient Story and Cancer Friends. I’m Andrew Schorr, with my dear wife and partner, Esther Schorr.
As a couple, we’d like to introduce you to another couple in Hudson, Ohio, and that is Pete and Katie Mang. First of all, thank you for joining us.
Katie: Thank you for having us.
Andrew, TPS: They have quite a story. For a number of years now, Pete’s been dealing with one of the most serious cancers, glioblastoma, also known as GBM. It’s usually older people [in their] 60s [or] 70s who have it. Pete, you were diagnosed at what age?
Pete: I would have been 34.
Andrew, TPS: Wow. So very young. We’re going to tell you the story of them, how it happened, being a young couple with 2 little boys, and eventually deciding, based on what they learned, to start a foundation to give back to people who are affected by a brain tumor.
Pete’s cancer diagnosis
Esther Schorr, The Patient Story: Katie, can you talk a little bit about how Pete was diagnosed?
Katie: In summer of 2018, it was a normal workday. I was driving home, and I got a phone call from Pete’s architecture firm, where he worked, that he had a seizure and was not communicating properly.
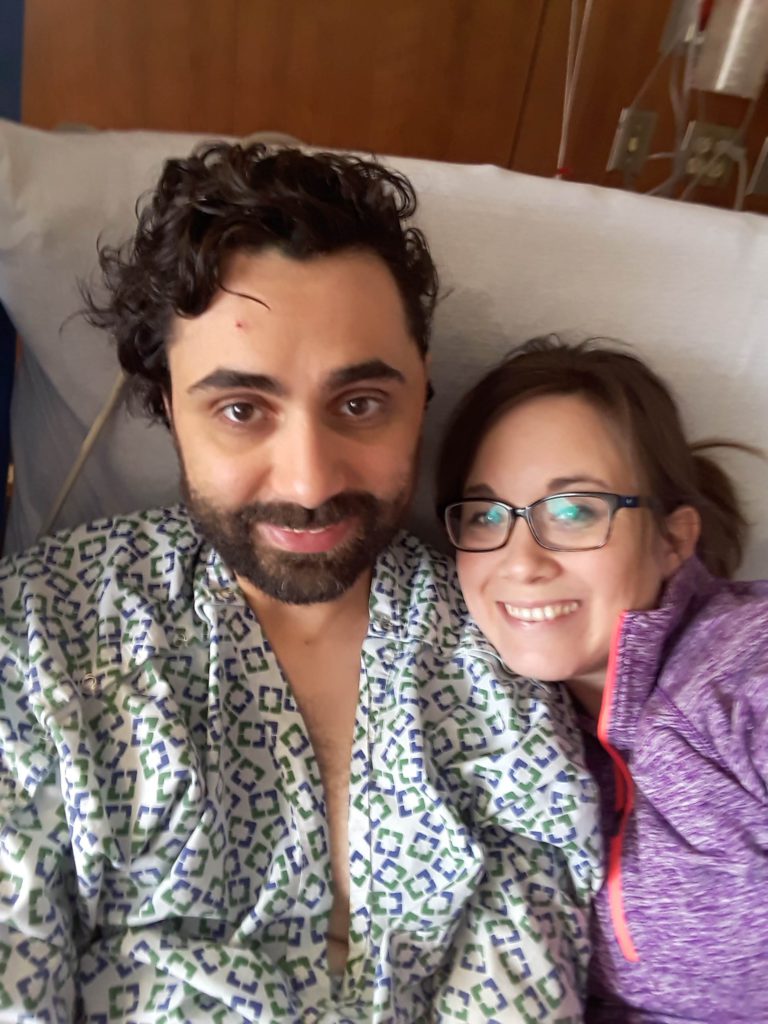
They had called an ambulance to take him to the county hospital, where I met him. [I] found out that on the commute there he had two grand mal seizures in the commute to the hospital. After several tests — and we weren’t quite able to get the seizures completely under control — they determined it was a brain tumor.
[It was] something that was a complete surprise to us with no family history and [with] Pete [having an] excellent health background. We consulted with a family friend who happens to be a physician, and he suggested we transfer to another hospital that had a cancer and brain tumor center.
That took a little bit of a fight with the hospital system, but we got it done. He then ended up at the Cleveland Clinic, and he was in the ICU for a brief period of time, trying to get the seizures under control.
»MORE: Patients share how they processed a cancer diagnosis
Awake craniotomy
Katie: Then for nearly 2 weeks, he stayed there until he had an awake craniotomy.
Andrew, TPS: What is that?

Pete: That was having surgery in your brain while being awake. They ask you questions, you have to answer those questions, and they figure out where they need to do the surgery at.
Andrew, TPS: What’d they ask you?
Pete: I remember [them] asking about the alphabet [and] some other questions that normally you would know. They figure out how far they need to go with the surgery as they’re talking to you.
Andrew, TPS: The goal is to cut out, for you, a golf ball-sized tumor, but not healthy tissue [so that you can] perform as much function as possible, right?
Pete: Correct. They want to get out as much as they can.
Katie: Based on where the tumor was located, speech was the primary concern, both in receptive and expressive speech, being able to retain the information and express it. Luckily, they were able to because of the craniotomy.
Andrew, TPS: Pete, you’ve told me sometimes you have to search for words or how to get the words out.
Pete: Right.
Treatment and symptoms
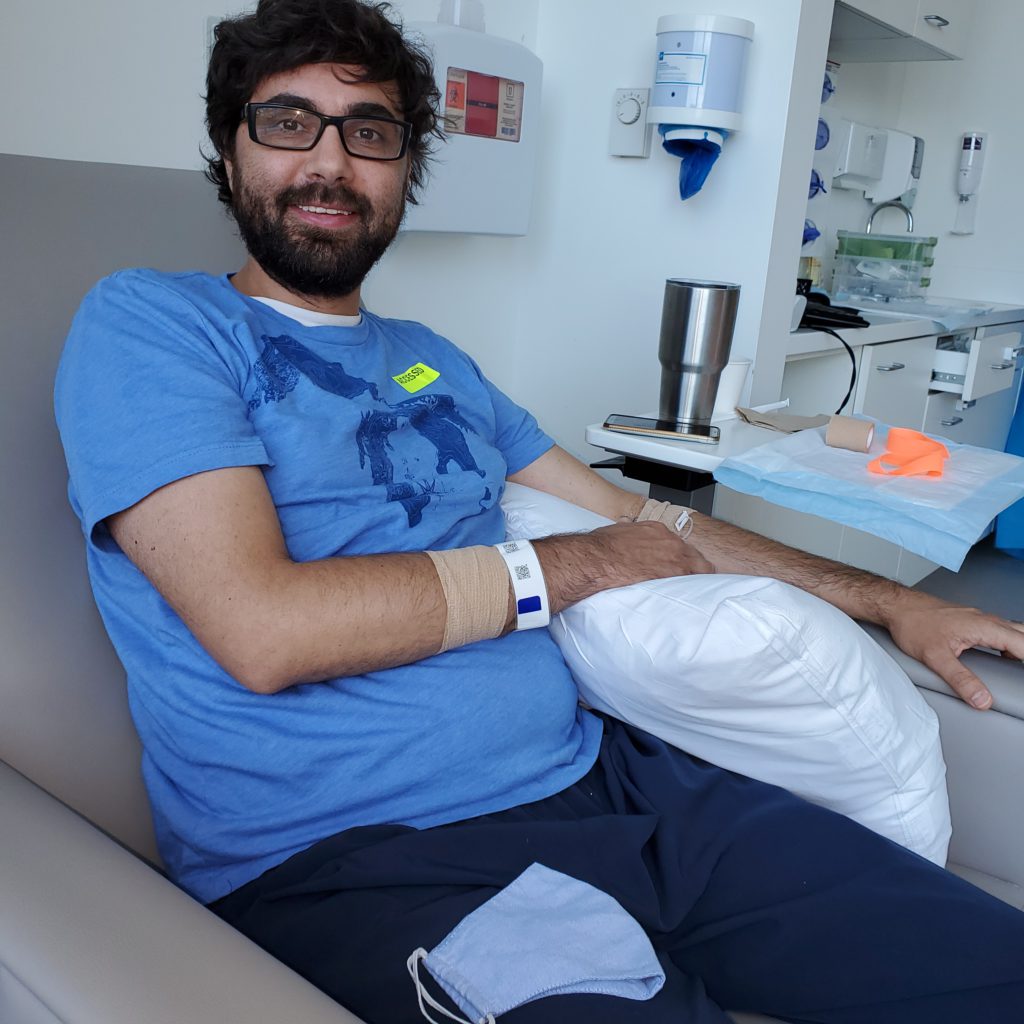
Andrew, TPS: You did have various therapy, but you got blasted, Pete, with first surgery, a lot of radiation, Gamma Knife, [which is] targeted radiation, [and] chemo. We’re talking about over 4 years. That must have been quite an ordeal.
Pete: There was always something we were doing at the clinic. There was always something.
Katie: Then the symptom management, too, that goes with that. It’s not just you go to the clinic, and it’s done. It’s taking care of the fatigue, nausea, and comfort care at home with it as well.
Esther, TPS: Now, Pete, what’s happening at the moment as far as your health?
Andrew, TPS: There’s a clinical trial. Tell us about all that.
Pete: Correct. I’m on a first phase trial, and I’ve actually been on that trial for over 2 years now. It’s an immunotherapy. I’m up doing this treatment twice a week. Usually, that day, I’m tired once I get home, so it gets hard sometimes.
Andrew, TPS: It’s remarkable, but we should mention you were telling us that you were on the treadmill jogging just a few minutes ago.
Pete: Right, absolutely.
Parenting with a cancer diagnosis
Andrew, TPS: Katie, this is a family event with younger people.
Esther: And younger children.
Andrew, TPS: And young children. Talk about that a little bit [and] how you cope. This [was] a major shocker that day you rushed to the emergency room. Your husband was having surgery. Explaining whatever you did to the children, the family, and coping yourself, and then doing that over several years now.



Katie: When this all happened, our kids were 2 and 5. [It was the] summer before our oldest started kindergarten. We had just moved into a new home about 6 months before that, and we were dependent on dual income [and] coparenting. We were both busy professionals.
Everything kind of got flipped upside down in one day. I took some time off of work. With the kids being so young at the time of diagnosis, we kept things very age appropriate. “Dad’s in the hospital. Dad’s not going to be home for a little bit. When he does get home, here’s the things. His hair might be gone. He might be tired.”
Our 5-year-old caught on to a lot more of it, where our 2-year-old doesn’t really know anything different. He’s now turning 7 next month, and then [the older one will be] a 10-year-old. They kind of have grown up, and we’ve reeducated and provided different levels of age-appropriate communication, also tailored to their personalities.
To have 2 kids in the same family be so different requires a little bit of different levels and types of communication with them, too. Being that they’re still young, they don’t know the full story. What we have learned is this disease is incredibly unpredictable.
To be on a clinical trial for 2 years, having treatment 2 years before that, [so] 4 years total. We couldn’t have guessed any of that. The burden of that uncertainty is a little too much to put on the kids.
They have what we would consider an age-appropriate understanding of the differences in our life since then, like how we handle things as a family differently. We consulted with our pediatrician on how to talk and handle with this, especially right after it happened. The pandemic happened in the midst of all this, too.
Pete: Then I started the trial.

Katie: With young kids being at home and being exposed to a lot of this, while going through this as well. We’ve consulted with the pediatrician. We’ve consulted with a child life counselor. Every year, I let the teachers know this is our family situation. We have excellent guidance counselors in our school, and they’re always aware of our situation.
It’s a little awkward, but every year at the beginning of the school year, I send an email to the principal. They know me by now, but I explain what’s going on here, too.
We’re lucky that we have navigated who needs to know in our children’s lives to provide the circle of support that’s age appropriate [and] that’s flexible. We have a plan in place if something bad were to happen. We just have to push the button, and everybody knows how to respond appropriately.
»MORE: Parents describe how they handled cancer with their kids

Support for the caregiver
Esther, TPS: Katie, obviously, this is a huge project for anybody. A family journey. You’re the key care partner here. How have you been able to cope with all this? What’s been the support that you get? You just described all this great support that you rallied for Pete [and] for your kids. How about you? What are you doing for yourself?
Katie: Over the last 4 years, I have built my personal support toolbox, but it’s taken a lot of trial and error to get to that point. I am very lucky to have a great network of family support in this area. I rely heavily on my close circle of confidants: my mom, my sister, a couple of close friends.
I also know if I need to talk to my doctor or therapist. I’m not shy about it. I think one of the things that’s helped both of us is we are both really realistic about what’s happening. We talk about that, and we’re very open.
I can come to Pete and say, “I’m having a bad day, and it’s because an MRI is coming up,” or, “I’m having a bad day because I’m stressed.” There’s no guilt in that, [which] maybe I felt early on. Pete’s super supportive.
Pete: We’re doing this together. The diagnosis is me, but it’s the whole family. We do this together.
Go With The Good Foundation
Esther, TPS: You’ve done something else together that you discussed. You mentioned to us that you started a foundation.
Katie: The day we got Pete’s diagnosis — because you don’t know right away. We have a brain tumor. Then there’s going to be surgery. Then they’re going to have a biopsy, and then 3 weeks later, you’re going to come back for a diagnosis and a plan.
At that point, we learned that this is glioblastoma. That’s a shock. Doesn’t matter that we’ve just been through all of this, and now the diagnosis is the shock. One of the things that really came out — I don’t know if it was that night or the next day, but we kind of talked about how we’re going to handle this from a mindset standpoint.
Pete said, “We’re going to go with the good.” Out of every situation, we’re going to find a couple of the key pieces of good, whether that’s having grace in the situation, getting a piece of good news or a good MRI, or just we had some chocolate and wine, and that was good.
Pete: Exactly. There’s always something good to look at. Like you said, we went to the restaurant and got a good dinner or something. Those little things add up, and so that’s where Go With The Good became [something].
Esther, TPS: Please explain what it’s for. What does the foundation do?
Pete: The base of the foundation is the focus is on young adults, families potentially, who have a brain tumor diagnosis. From a financial standpoint, it becomes difficult from that diagnosis.

There’s a lot of information that we’ve learned throughout this 4 years and through research and everything. There was a lot that we’ve learned that some of these other families may not have learned. The goal was to pass this information to them and financially help them from that diagnosis.
Andrew, TPS: What a beautiful thing.
What key lessons have you learned?
Andrew, TPS: Katie, what are some of the key lessons learned?
Katie: That it would have been good to know going into this that brain cancer is, depending on different reports, the most or second-most expensive cancer to treat. Not only because of the extensive and expensive treatment, but all the treatments that go around it, like speech therapy, occupational therapy, seizure medications, [and] all those things.
It would have been good to know what we were getting into. We want to pass that on not as something to scare you, but knowledge is power. You need to know where you stand in this, how and when to navigate, and where to find support for insurance disputes.



All of the therapies I just described, there’s a line item in insurance for every single one of them. Learning the insurance system and also knowing when to pull in help has been valuable, both in peace of mind, but also our wallets.
Also, knowing who to go to for the various types of support. If you didn’t know some of these resources could be found for free or inexpensive, you would pay a lot of money for help in a lot of these things, whether it is a legal dispute, care, or services.
For one example, we were able through family reach to get free financial consultation. I was considering paying for that, and then we were able to get this at no cost, pro bono. [We also got] someone who understood our situation as a young couple trying to navigate the financial ups and downs with an uncertain diagnosis.

Then we didn’t know that we could get brain-tumor-specific support through the network and clinical trial navigation services support with Medicare and Social Security.
Pete: Like you said, the seizure medication is very expensive, and we were able to find these groups that were able to really help financially on the costs of these medications.
Katie: We’re talking thousands of dollars a month.
Andrew, TPS: I can’t even imagine. What is the website address, Katie?
Katie: It’s GoWithTheGood.org. We just launched this year, so keep checking back as things keep getting updated.
Esther, TPS: The other big resource you mentioned was the Family Reach Foundation.
Andrew, TPS: Family Reach Foundation helped you, and they’re a great organization.
The burden of uncertainty
Andrew, TPS: You used a phrase earlier, Katie, and I wanted to ask both of you how you deal with it. You said, “The burden of uncertainty.”
First, Pete, how do you deal with the burden of uncertainty? Katie touched on how [glioblastoma is] so unpredictable, [as well as] what course it’s going to take and when. How do you deal with that?
Pete: To be honest, I’m not quite sure. The words aren’t coming to me right now as part of the aphasia. Finding some of these words are hard right now, to be honest.
Katie: I think the thing that you and I have both talked about [regarding] the uncertainty is making the most in the moment.
Pete: Right.
Katie: Being very mindful and present in the moment, as well as prioritizing what’s important to us in the moment. We have made major changes to our life in terms of how we spend our time, how we do our careers, how we spend time with our kids, [and] how we make family decisions. Not just because of the uncertainty, but a bit of the blessing of the uncertainty is it has had us focus on what’s really important.
Pete: With the uncertainty, for me, having 2 young kids, I enjoy that time. I think that’s where I come from. Every single time that we do something as a family with the kids, it’s special no matter what we do.

Andrew, TPS: You mentioned you’re in a clinical trial with an immunotherapy. In a number of cancers, immunotherapy has been rewriting the history [and] the journey of people with what otherwise would have been cancers that would shorten somebody’s life dramatically.
It sounds like in the moment, you’re giving back a lot, and you’re treasuring the time you have together. That’s a beautiful thing, too.

Living with gratitude
Esther, TPS: You talked about gratitude, and I think at the root of what you’re talking about is gratitude for the time you have together with your children. [I think you’re] spreading that essence of the way people should live their life, no matter what their situation is.
In some ways, maybe that is the little tiny silver lining in people touched with cancer. It does give you pause to be grateful for the time that you have together. You sometimes don’t appreciate that.
Pete: Right.
Andrew, TPS: Not going to run for the bus or the train. You’re going to live in the moment.
Katie: What do we say? You’ve said this so many times. You’re like, “We don’t need to sweat the small stuff.” We let a lot just roll off it.
Pete: I go slow. Go slow with it. Why rush through things, you know?
Andrew, TPS: That’s the point. Slow down the cancer journey. You want to be cured. We all want to be cured. I’m a 2-time cancer survivor. We want to be cured, but short of that, while we’re undergoing treatment, enjoy what we can.
Esther, TPS: The things other than treatment.
Pete: Exactly.
Conclusion
Andrew, TPS: I’m sure they know your name well at the Cleveland Clinic.
Pete: Oh, yeah.
Katie: Frequent flyer. They were sending around a retirement card.
Pete: The guy was leaving, one of the nurses, and all the nurses signed it. They came and were like, “Hey, Pete, can you sign the card for us, too?” Because I’ve gotten to personally know some of these nurses. I know their kids, and I know what sports they’re doing.
Andrew, TPS: We wish you all the best. Thank you for sharing time with us. Good luck with the foundation and how you’re giving back. Certainly with your treatment, Pete, we wish you all the best. Katie and Pete Mang in Hudson, Ohio. Thanks for being with us.

Inspired by Katie and Pete's story?
Share your story, too!