Harjeet’s Stage 4 Subcutaneous Panniculitis-like T-cell Lymphoma (SPTCL) Story
Harjeet shares her stage 4 non-Hodgkin’s lymphoma story, dealing with a rare cancer diagnosis of subcutaneous panniculitis-like T-cell lymphoma. She describes her treatment, including multiple chemotherapy regimens and an allogeneic stem cell transplant.
In her story, Harjeet also highlights how she thought of fertility preservation, the support that helped her the most, and how she’s transitioned to survivorship.
- Name: Harjeet K.
- Diagnosis (DX)
- Subcutaneous Panniculitis-like T-cell Lymphoma (SPTCL)
- Rare subtype of non-Hodgkin’s lymphoma
- With hemophagocytic lymphohistiocytosis (HLH), an autoimmune disease
- Subcutaneous Panniculitis-like T-cell Lymphoma (SPTCL)
- Stage: 4
- 1st Symptoms
- Persistent high fevers
- Red and tender lumps or rashes formed on legs below the knees
- Fatigue
- Night sweats
- Weight loss
- Chills
- Treatment
- CHOEP chemotherapy
- 6 cycles
- GemSi chemotherapy
- Salvage chemotherapy
- 6 cycles
- Allogeneic stem cell transplant (SCT) or bone marrow transplant (BMT)
- Brother was a 100% donor match
- CHOEP chemotherapy

- Getting Diagnosed
- What were your 1st symptoms?
- When did you go to the doctor?
- Describe the ER visit
- When did the symptoms worsen?
- Describe the biopsies you underwent
- What led to the diagnosis?
- How did you process the cancer diagnosis?
- Deciding where to get medical treatment
- What was the full non-Hodgkin’s lymphoma diagnosis?
- How did you break the news to loved ones?
- Treatment & Side Effects
- Did you get a port or PICC line?
- Describe your chemotherapy regimen
- How were your chemo infusions?
- Describe the chemo side effects
- Describe the hair loss
- Mentally processing the identity changes
- How effective was the CHOEP chemotherapy?
- Treatment plan addition: stem cell transplant
- What was the discussion about fertility preservation?
- More side effects hit later
- How did doctors try to get rid of the CMV eye infection?
- What was the second chemotherapy regimen?
- Overall treatment recap
- Stem Cell Transplant (Allogeneic)
- Describe the transition between chemotherapy and stem cell transplant
- For your allogeneic stem cell transplant, your brother was your donor
- What was the preparation ahead of the stem cell transplant?
- Describe the day of your stem cell transplantation
- How was the recovery following the transplant?
- Describe the recovery at home
- Your low blood counts persisted
- What has the follow-up been?
- Reflections
- What was the hardest to go through?
- Dealing with so many treatment questions
- The power of positive thinking
- How important was it to have support?
- Were you able to work through treatment?
- How has survivorship been?
- How do you cope with the ongoing follow-ups and maintenance?
- Any last message to other patients?
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
I am a survivor and a warrior, and I have learnt that the human spirit is stronger than any adversity. No matter what your battle is, just keep going and keep fighting.
Focus on being well and focus on being healthy. It took all the strength and motivation to survive this, and I felt it down to every fiber of my being. I am acutely aware of how lucky I am to be given a second chance to live.
Harjeet K.
Getting Diagnosed
What were your 1st symptoms?
I immigrated to Canada in May 2018 to settle down. My life was going in the exact direction I had dreamt of up until this moment — to travel the world, have kids and build my future in this beautiful country.
It all started from the end of May 2019. I started having some fevers. It continued for 3 to 4 days. Two weeks passed, but my fevers did not.
Overall, first symptoms:
- Persistent, high fevers
- Red and tender lumps or rashes formed on legs below the knees
- Fatigue
- Night sweats
- Weight loss
- Chills
When did you go to the doctor?
We went to see our family doctor, and she advised some blood work and X-rays. After going through my blood tests and X-rays, she couldn’t find anything and said it might be a viral fever. All the tests that were done on me so far were negative.
Describe the ER visit
I went to the emergency room as the fever was persisting in the range of 38.5°C to 39.5°C (101.3 to 103 F). This was the first time I felt nervous, worried that something was really wrong with me.
After getting all the blood tests and X-rays done all over again, the doctor at emergency referred me to an internal medicine specialist.
Two days later, I got a call from an internal medicine specialist for my appointment and physical checkup. I was admitted to the hospital by June 2019 midweek for further checkups and scans.
I took 1,000 mg of Tylenol every day, as advised. I had a fever every single day for about 2 months.
When did the symptoms worsen?
In August 2019, new symptoms developed in my body. Red and tender lumps formed in my legs below the knees.
The team of doctors at the hospital had a look, and different opinions were made out of it. They concluded that it could be a case of erythema nodosum.
I had no idea what they were talking about!
I had countless blood tests, scans, X-rays and surgeries (laparoscopy and colonoscopy) after my CT scan showed some abnormalities. I was scared as hell as I still had no answers. It had been almost 3 months, and my fevers were not going away.
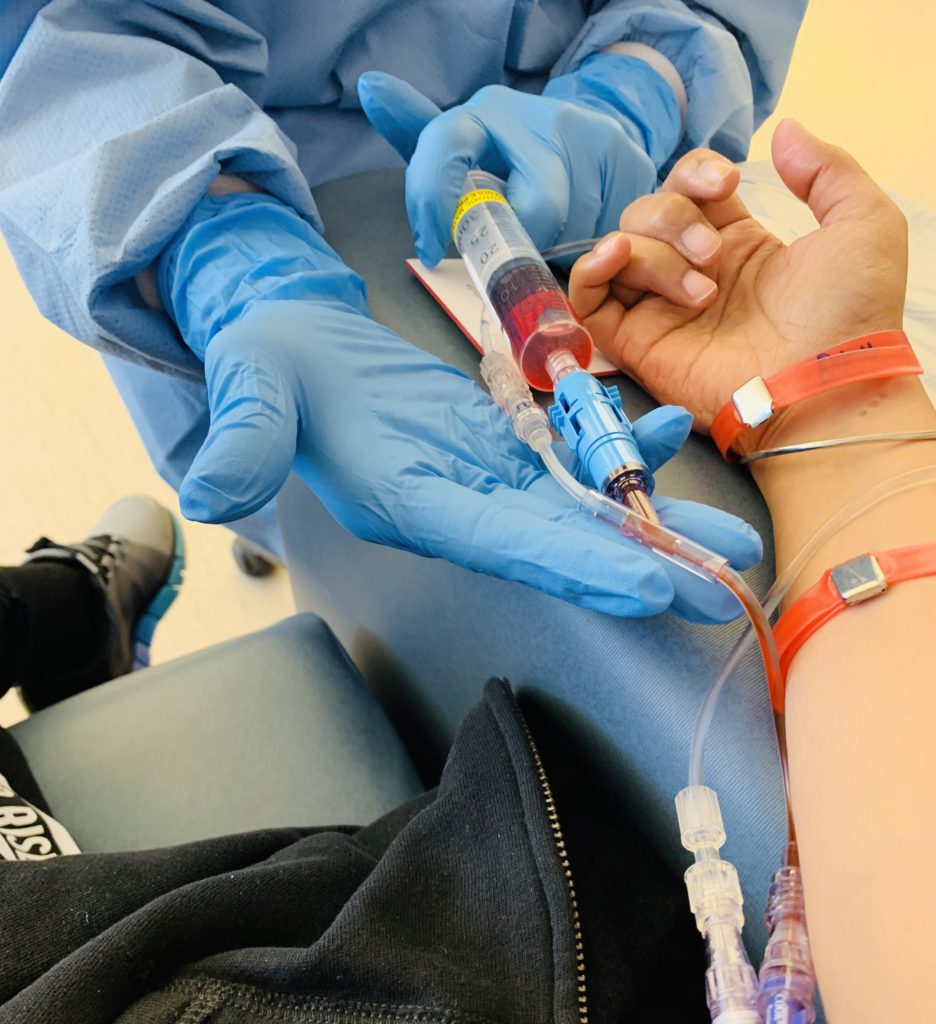
Describe the biopsies you underwent
My husband planned to take me back to India to get treated there because we had no answers. The doctor’s team recommended a bone marrow biopsy, which was a last resort to put a name to my illness.
My bone marrow reports were sent to a special pathology team in Calgary, and multiple special tests were done on my biopsy.
I had 5 biopsies and had no answers from our doctor because they were waiting for the final report. I became frustrated and impatient.
I felt I was treated as a research patient for registered doctors in a university hospital for a relatively new and rare case with fevers and no other major symptoms.
What led to the diagnosis?
Days were passing by, but we didn’t hear anything from the doctors. One day they noticed drastic changes in my blood counts and decided to do a skin punch biopsy from my lower back.
My husband and I were not at all willing to get it done but gave in to pressure eventually. My husband was massively irked and asked the doctor to discharge me from the hospital and get my papers ready to take me to India.
We decided to book a flight for the 30th, 2 days after I would’ve been discharged. As fate would have it, right before my discharge, I received the most devastating news of my life. The skin biopsy came out with a positive diagnosis.
My world flipped upside down in one swift motion. I was diagnosed with stage 4 cancer — non-Hodgkin’s lymphoma, specifically T-cell lymphoma.
How did you process the cancer diagnosis?
At that time, I did not know what my doctor was talking about. I asked her again what she meant. She answered that it’s a type of blood cancer and not to worry because it is curable.
She kept going on about how and when we can start the treatment, but my mind could barely register one word. I was numb.
After listening to that, everything paused for a few moments, and everyone was silent. It had taken them 3 months to diagnose my cancer. I didn’t understand much of the information at that time, as I was trying to wrap my head around the enormity of what had befallen me. At last, I burst in tears of helplessness.
I had just received the most horrifying, heart-wrenching news. The mind screamed in disbelief and denial. I thought, “How could this happen to me? Why me? How is this happening to me? What have I done wrong to deserve this?”
I was only in my 30s. I used to have a positive outlook on life. Being diagnosed with cancer is news no one wants to hear in his or her lifetime. It was completely unexpected.
I always heard about this C-word. Still, I never expected this to happen to people I know and love — or me. I had my mom, husband and brother with me when I got the news about my cancer.
»MORE: Processing a cancer diagnosis
Deciding where to get medical treatment
My doctor said, “I want you to stay here and not plan to go to India. We want to start your first chemotherapy treatment tomorrow. You will get better treatment here.”
The pathology team would do the final report of my bone marrow biopsy. We were still waiting to hear back from my oncologist about my full diagnostic report on the hemophagocytic lymphohistiocytosis (HLH).
What was the full non-Hodgkin’s lymphoma diagnosis?
I was officially diagnosed with stage 4 cancer, specifically subcutaneous panniculitis-like T-cell non-Hodgkin’s lymphoma with HLH, an autoimmune disease.
It’s an aggressive type of cancer and rare diagnosis with only 150 cases reported worldwide.
I was transferred to the Hematology Department the next day on August 29th for my first chemotherapy treatment. I was not sure what was happening around me. I was confused. Everything was happening so fast, and I had a thousand questions.
How did you break the news to loved ones?
Telling people about my cancer diagnosis was the most challenging thing for me. I had to share this news with my family and friends, as they were worried. I was not ready to share this news socially.
Luckily, my husband tried reaching out to my close friends and my colleagues. My mom reached out to my family in India. My dad was in India, and my family back home was hesitant about telling him this news.
My dad could not stop himself from crying. He felt helpless; his daughter was going through all this, and he was in India far away from me. He planned to come to Canada as soon as possible.
»MORE: Breaking the news of a diagnosis to loved ones
Treatment & Side Effects
Did you get a port or PICC line?
I had to get a PICC line insertion done to get started in my right arm for my chemotherapy treatment.
»MORE: Read more PICC line experiences
Describe your chemotherapy regimen
On the first day of chemo, I was nervous and anxious. The day the oncologist walked in my room, he pulled up a chair and told me about my cancer, its complications, and how aggressive my treatment would be.
I still have his sheet explaining how rare this cancer is and that there was less research on this type of cancer. I had stage 4 lymphoma, so my chemo was a high dose. They planned to give me 6 CHOEP treatments, including the “red devil” chemo.
I had to go for 6 chemotherapy treatments for my regimen, having one session each month. I used to get rigors and fevers, so I had been in this routine to get blood tests before getting chemotherapy to see if I had an infection or a virus.
I was in the University of Alberta hospital until my 2 chemotherapy treatments were complete. My further treatment was done at Cross Cancer Institute Edmonton as an outpatient.
How were your chemo infusions?
The whole day went by in a blur, and yet it was painfully long. I had a million things running through my head, and I wasn’t sure how to process any of it.
After my second chemotherapy treatment, I was told that this could be the week when I might start feeling chemo side effects.
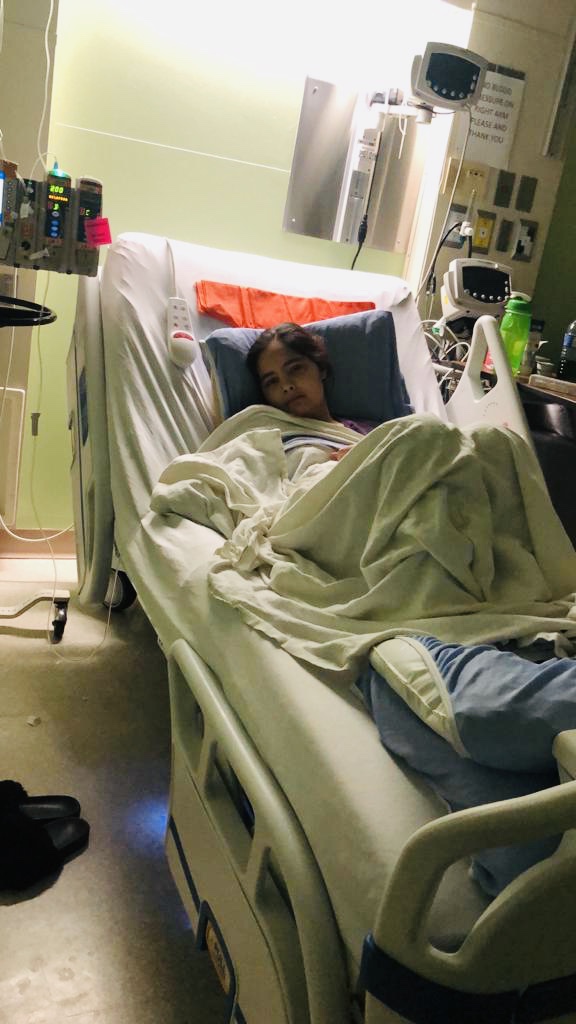
Describe the chemo side effects
Some of the side effects of chemo were losing my hair, feeling weak, fatigued, nauseated, insomnia, slight fever and night sweats.
I have seen good and bad days. Chemo is a bitch. It’s as bad as they say it is. The pain was indescribable. I was bedridden for months in the hospital due to pain, aching bones, nausea, high fever, no taste, mouth sores, tingling fingers, mood changes and chemo brain.
»MORE: Cancer patients share their treatment side effects
Describe the hair loss
The worst part for me was when I started losing my hair after my second chemotherapy infusion. My eyelashes and eyebrows were gone, too. Losing your hair is horrifying. It’s a part of who you are, and losing it makes you feel naked, different, and ugly.
The physical changes of having cancer have affected me mentally. My husband cut my hair and made it shorter, so I don’t feel as much pain in my head.
I used to wear beanies most of the time during my treatments. I tried a lot of wigs, but they were not so comfortable for me, so I used to avoid them for long hours.
»MORE: Dealing with hair loss during cancer treatment
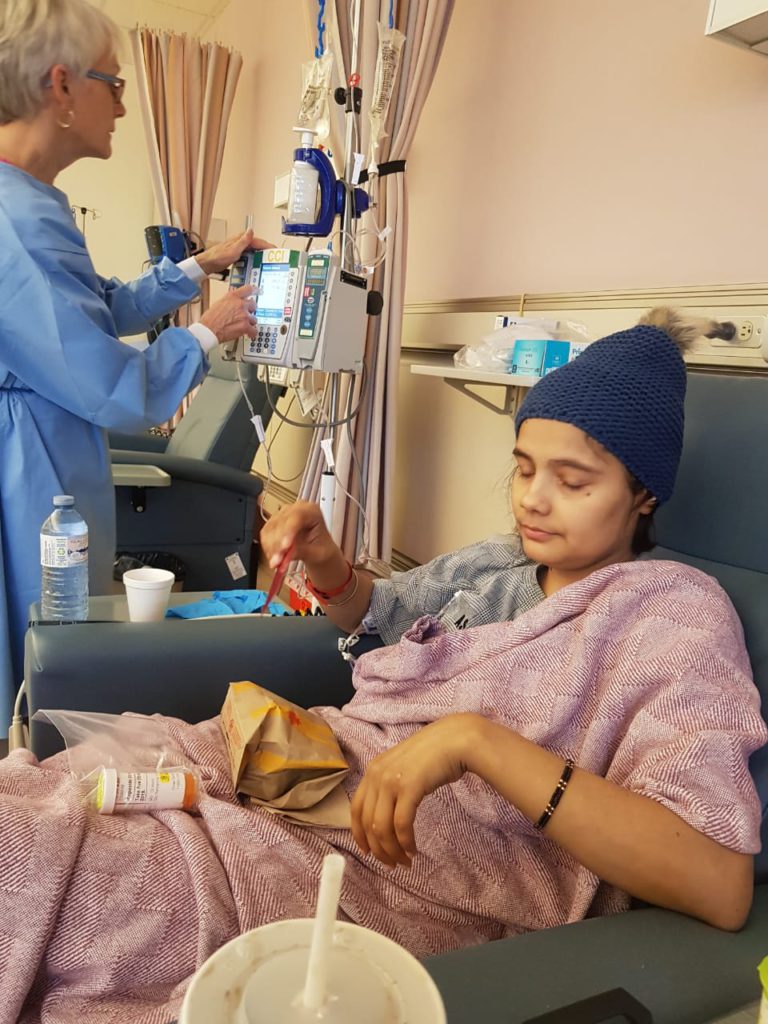
Mentally processing the identity changes
Cancer isn’t just about chemo, radiation, losing hair or losing weight. It’s also about losing yourself, who you are, what you look like, your job and your life.
For me, I was being overloaded with anxiety and anger.
How effective was the CHOEP chemotherapy?
Through 3 chemotherapies, my body was showing some improvement, but my blood counts were still low. I was still getting some fevers and infections.
I used to get my blood tests and blood cultures done on a daily basis to rule out any infections or viruses. I had my PET scan scheduled for November 14th, 2019.
After my fourth chemotherapy treatment, my body showed minimal improvements. I still had signs of cancer cells in my body, which were not responding to the treatment and were still progressing. Additionally, there were signs of HLH.
After completing my 6 cycles of chemotherapy, I got a call from my oncologists for a visit. He said I have to go for 6 more cycles of salvage chemotherapy this time.
Treatment plan addition: stem cell transplant
To top it off, I was told that the best treatment option given my medical scenario would be a stem cell transplant once I hit partial remission.
I was told my stem cell treatment would be in Calgary. They would review my case and suggest options for my transplant and chemotherapy.
I was in the hospital on and off because of high fevers, low blood counts and infections. My chemo journey had been quite rough with many obstacles in the way. I had lost most of my muscle mass, and I could barely walk. My hands were so shaky that I couldn’t even pick up my phone.
What was the discussion about fertility preservation?
I had to visit the fertility clinic to see if the doctor could freeze my eggs or if there was any chance of me getting pregnant. Still, the answer was no, as I had already gone through heavy doses of chemotherapy.
I lost my fertility and was thrown into menopause. The news devastated me. I had always wanted to have my own family.
»MORE: Fertility preservation and cancer treatment
More side effects hit later
In January 2020, I started getting some blurry vision in my right eye. After reaching out to my oncologist, he said it was the side effect of the medications I had been taking, like the dexamethasone (steroid). He said it should go away with time.
One evening, I was watching TV, and suddenly I could only see partially through my right eye. We went to the emergency room that night. The next morning, I had an appointment with my ophthalmologist.
My doctor told me that my retina was heavily damaged, and he was unsure if it would ever heal because I had gotten the cytomegalovirus retinitis (CMV) viral infection in my right eye. Apparently, due to low immunity, I could catch any infection or viruses very easily.
How did doctors try to get rid of the CMV eye infection?
They tried giving me some injections in my right eye before I had a couple of eye surgeries. I also underwent a biopsy to check if the lymphoma had progressed to my right eye.
Thankfully, there were no signs of lymphoma in my right eye, which was a relief. However, since the retina of my right eye had taken on significant damage because of the CMV virus, the vision loss is permanent.
What was the second chemotherapy regimen?
In February, I started 6 rounds of GemCis as my chemotherapy treatment every 2 weeks. It was ongoing because I was in partial remission and getting ready for my next phase of the stem cell or bone marrow transplant. Originally, it was scheduled for the end of March.
Overall treatment recap
During 7 months, I had:
- Countless number of physical examinations, blood tests, X-rays, ultrasounds, nuclear medicine scans, MRIs, CTs, and PET scans.
- ICU for 24 hours for my surgery
- 3 surgeries, 7 biopsies, blood and platelet transfusions, emergency night visits due to high fever and pain, 30 Grastofil injections (to fight infections), 6 ganciclovir injections (into my right eye)
- Lost vision in my right eye due to CMV
- Lost fertility and thrown into menopause
- Underwent 12 rounds of high-dose chemotherapy
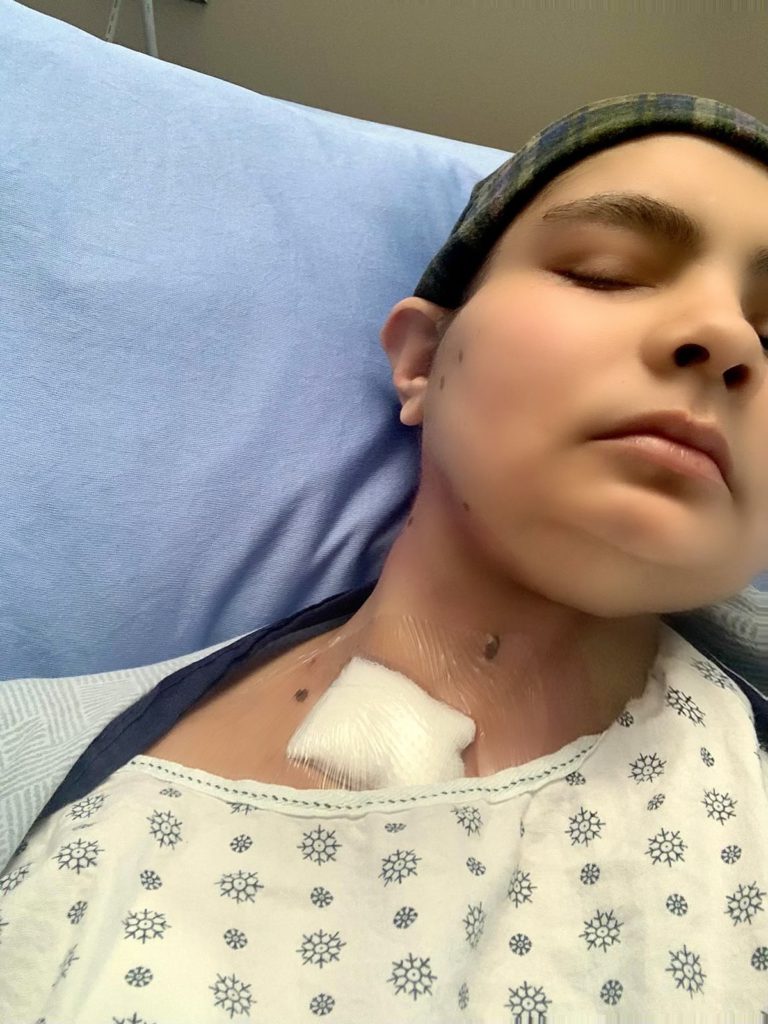
Stem Cell Transplant (Allogeneic)
Describe the transition between chemotherapy and stem cell transplant
I completed my 12th chemotherapy treatment in the first week of March 2020, just as the world was coming to terms with the fact that we were in the middle of a deadly global health crisis.
As per my PET scan on March 13th, I was in partial remission. It was time to start with the stem cell transplant journey of fighting and removing these cancer cells and HLH out of my system.
I met with the stem cell transplant (SCT) team in Calgary. They seemed happy enough with my PET scan report to move forward. The transplant would involve a 4- to 5-week hospital stay in isolation. My SCT team started with my paperwork, blood tests, scans, and medical examinations.
For your allogeneic stem cell transplant, your brother was your donor
I was undergoing an allogeneic stem cell transplant. My donor was my little brother, who was a 100% DNA match.
I had mixed feelings about all this. I was happy that I could finally do this part of the treatment, which was also the most challenging bit. I also had to go for another bone marrow biopsy (my 8th) before the stem cell transplant process. I was impatient and stressed out due to the delays caused by COVID.
What was the preparation ahead of the stem cell transplant?
I had to be isolated for 30 to 40 days in the hospital for my stem cell treatment. I couldn’t see my family or have any visitors.
COVID ruined everything.
The doctor already warned us the treatment would be intense for me and that there could be a 15% chance of dying during this whole SCT process.
The very first part of the SCT process was conditioning therapy. I would be given 7 days of conditioning chemotherapy and radiation to damage and possibly wipe out my bone marrow. It was a tough time for me and my family.
I had to get a CVC line inserted. My treatment was 5 days of fludarabine and busulfan, 3 days of anti-thymocyte globulin (ATG, which is an infusion of horse or rabbit-derived antibodies against human T-cells), and 2 days of total body irradiation.
Describe the day of your stem cell transplantation
It happened on April 14, 2020 — my stem cell transplant day, also known as my re-birthday! The doctors and nurses were quite incredible and supportive that day, knowing that I was all alone for the procedure.
It all went very smoothly. It’s like getting a blood transfusion. Infusing the donor stem cells takes several hours.

How was the recovery following the transplant?
The days that followed the SCT weren’t any cakewalk. After 3 to 4 days of SCT, I started developing mouth and throat pain, a known side effect of chemo and radiation therapy called oral mucositis.
I had trouble speaking, eating, and even opening my mouth. I was prescribed soft foods, popsicles, yogurt, and boost drinks. My doctor advised me to get a food pipe insertion as I could barely eat, and my body needed nutrients to keep me going. The conditioning chemotherapy treatment drained me emotionally, physically, and mentally.
There is no way to sugarcoat it. The transplant without a doubt was an excruciating experience that I wouldn’t want anyone to ever have to go through. I was never ready for this persistent sickness, weakness, and pain I endured over weeks.
I spent most of my time lying in bed watching Netflix, playing online games, and FaceTiming my family and friends. There were days and nights when I would scream in pain.
I was not even able to talk to anyone due to my sore mouth and throat. The doctors put me on daily narcotics (a pain pump) to keep the severe pains at a reduced level. Due to narcotics, I was sleeping a lot.
My oxygen level was low, so I was put on oxygen 24/7 for 2 to 3 days. I was living with trauma, feeling irritation and anxiety.
I could not even recognize myself in the mirror anymore with that swollen face, eyes, and lips; the dryness; and the radiation tan.
Describe the recovery at home
I sometimes still cannot believe that I crossed that finish line, and I have a body of new cells that will hopefully keep me cancer-free for the rest of my life.
After 32 days of hospitalization, I was finally home.
I’m still fragile, and I can’t walk far, but I am just so grateful the worst of the symptoms have passed. The first 100 days of post-stem cell transplant are crucial because the transplant can be rejected, and I could get critically ill.
During this time, my blood counts were low, as I got the BK virus and EBV virus after my SCT. Fatigue had been affecting me a lot more than I anticipated. I felt constantly exhausted. I was aware it would take a long time, but thankfully it was mostly recovery from here.
Your low blood counts persisted
More than 6 months post-stem cell transplant, my blood counts were not rising as they should after an SCT. My PET scan report didn’t show any signs of cancer.
My doctor was not sure why I had these small lumps on my legs and thighs. She wanted to go for another bone marrow biopsy. Honestly, my body and mind were begging for a break. I had been through a lot already after the transplant.
Mentally, the last few weeks were quite difficult with a lot of ups and down. It’s hard because although I finished treatment, I still felt like my life was completely on hold, and I couldn’t really put treatment behind me.
I was still neutropenic, which means I had deficient white blood cells to fight infection, hence the need for isolation. I still got Grastofil injections every week.
My oncologist was still not sure why my counts were low. They just wanted to wait and watch for my symptoms, as this disease doesn’t have much work-up and diagnosis has not been so easy. After listening to all this, I could just hope and pray for the best in life.
What has the follow-up been?
I have to go to Cross Cancer Institute for blood work every Monday and an oncologist appointment the third week.
Reflections
What was the hardest to go through?
During my pre-diagnosis, more than a month had passed by, and still, no one had any answers to what was going on with me. My reports were all adequate, and my body was not indicating any other symptoms.
My husband advocated for me and fought to get a full-body CT scan done. It had been more than a month, and my condition was not getting any better. It was deteriorating day by day.
We tried our best together by talking to different departments of doctors when I was in the hospital for 2.5 months to get answers. It ended up taking 3 months for them to diagnose my cancer.
During my treatment, my doctors and team were really supportive. My oncologist made sure that I could get better treatment. We had a lot of concerns after my third chemotherapy, as things were not clear about HLH. The only option was to go for SCT.
Dealing with so many treatment questions
I was not sure what was happening around me. I was confused. Everything was happening so fast, and I had a thousand questions.
Chemo? Radiation? Surgery? Infertility? This doctor or that doctor? Cancer was a condition I could not control, but the way I fight it was up to me.
I used to cry when I was alone in the hospital. I was scared. I didn’t want to leave the world like this. Life is vital to me. I had lots of plans for the future.
Despite my momentary weaknesses, I knew I couldn’t afford to lose faith or hope. I had to fight and beat cancer. I kept encouraging everyone around me and telling them that it was okay, and I was going to be okay.
The power of positive thinking
The only way to cope was to keep a positive mindset, stay healthy, and have faith in God. Every day I decided to face this challenging time with strength, determination and positivity.
I am grateful for my incredible husband, family, and close friends, who went above and beyond to support me during these dire times. This made me feel strong enough to fight this battle like a warrior. I was not alone in this fight to defeat cancer.
During this whole journey, I have battled many hardships. I was anxious about what would happen next. Will I survive and win this battle? This messed up my head, but I had to stay positive to keep my strength.
How important was it to have support?
To the best parents who never fail to support me, I can’t imagine what they might have gone through to see their daughter face something like this. I am thankful for them and my husband every day.
I am strong because of my family and their continuous support. They have been my full-time caregivers since day one. I am grateful to my husband, who is my companion, best friend, and rock; my brother; and my close friends.






Were you able to work through treatment?
I haven’t worked since June 2019. I have been on a long-term disability plan since then until now, thanks to the Canadian government and my employer for their medical benefits.
It really helped me and my husband to cover my medical bills and expenses. I have insurance, so it covers 80% of my medical bills.
How has survivorship been?
I still have a long way to go, but I’m already so far from where I used to be even 5 months back. You don’t always think about how much identity you take from your appearance till it’s taken from you. I have hope that it will only be for a short while.
I’m going to come back stronger.
The hair will grow back, and my strength and energy will come back better than ever! This is just one phase that will lead to a much better one, and I am eternally grateful for this opportunity.
How do you cope with the ongoing follow-ups and maintenance?
Mentally, it’s been quite difficult with a lot of ups and downs. It’s hard because although I have finished treatment, I still feel like my life is completely on hold and like I can’t really put treatment behind me.
It’s emotionally draining to keep being scanned and keep waiting for results. To keep going back to hospital every Monday — that has so many traumas associated with it. I am not “all clear.” I am NED (no evidence of disease), which is very different and makes life seem rather fragile. It can be snatched away again so easily.
With every passing week, I feel better and better. I was worried that I wouldn’t know how to live my life without cancer. I’ve been exercising and sleeping normally. I have joined cancer groups to keep myself busy and also to be with those people who have been affected by this trauma: the Young Adult Cancer Center and The Leukemia and Lymphoma Society of Canada.

Any last message to other patients?
I am a survivor, a warrior. I have learned that the human spirit is stronger than any adversity. No matter what your battle is, just keep going and keep fighting.
I’m finally starting to process a bit more of what I have been through the last year and a half. I had the biggest reason to continue fighting: my loving family. I have endured the worst and now intend to embark on a new journey with my loved ones.
Focus on being well and focus on being healthy. It took all the strength and motivation to survive this, and I felt it down to every fiber of my being.
I am acutely aware of how lucky I am to be given a second chance to live.

Inspired by Harjeet's story?
Share your story, too!
Metastatic Non-Hodgkin’s Lymphoma Stories
Erin R., DLBCL & Burkitt Lymphoma, Stage 4
Cancer details: Characteristics of both subtypes
1st Symptoms: Lower abdominal pain, blood in stool, loss of appetite
Treatment: Chemotherapy (Part A: R-CHOP, HCVAD, Part B: Methotrexate, Rituxan, Cytarabine)
...
Emily G., Diffuse Large B-Cell (DLBCL), Stage 4
1st Symptoms: Pain in left knee
Treatment: R-CHOP chemo (6 cycles), high-dose methotrexate chemo (3 cycles)
...



One reply on “Harjeet’s Stage 4 Subcutaneous Panniculitis-like T-cell Lymphoma (SPTCL) Story”
You are such a strong girl. You are an inspiration to many ❤️