Stephanie’s Story:
5 Years Cancer-Free
Lessons Learned & Top 10 Tips for Other Cancer Patients

It’s been 5 years since Stephanie Chuang, founder of The Patient Story, was told she was NED (no evidence of disease). As part of Blood Cancer Awareness Month, she celebrates by putting together a very personal video diary with the top lessons she learned since the Non-Hodgkin lymphoma diagnosis.
She hopes her documented ups and downs will resonate with some of you out there and be helpful to you.
- Looking back
- Tip #1: Emergency Department may lead you to faster care
- Tip #2: Break the monotony
- Tip #3: Seek out the humor
- Tip #4: Draw your boundaries
- Tip #5: You are a big part of decision-making during treatment
- Tip #6: Don’t chase the side effects, especially nausea
- Tip #7: There will be ups & downs and that is okay
- Tip #8: Wear loose clothing without metal
- Tip #9: Earlier appointments may help you get results faster
- Tip #10: Speak up for yourself!
- Give yourself grace
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Looking back
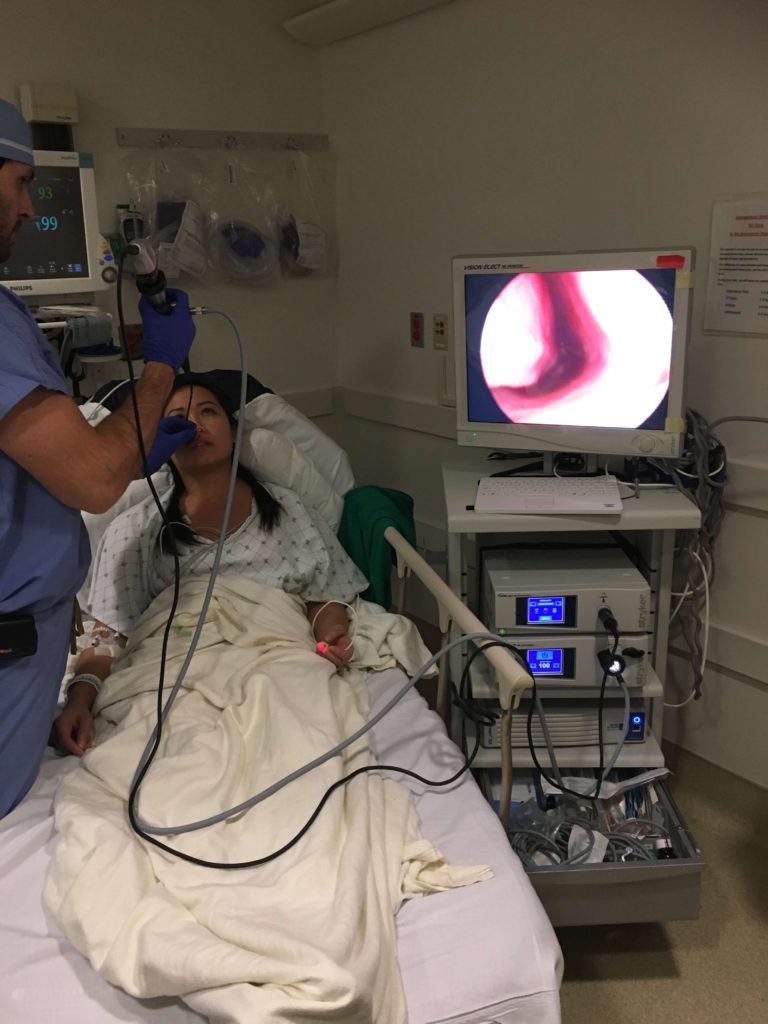
December 10, 2016. Fun times on a date with my family in San Francisco. These would be the last non-cancer memories captured on my phone. Just three days later, I would hear, “I’m sorry you have lymphoma,” and be thrust into an out-of-body experience — stuck in the hospital while doctors ran tests and scans for an entire week to figure out what was wrong with me.
Alien-like images from dozens of tests and scans. This was the hardest period — not knowing what the diagnosis was and just trying to figure it out. There were tests upon tests in under a week. I was poked and prodded constantly, including an excisional biopsy (where I was fully under so they could remove and test the lymph node) to the bone marrow biopsy (that only required local anesthesia before the “drilling” began).
Now, no evidence of disease for five years and, for that, I am really grateful. This is a walk-through of all the high and low lights that I’ve gone through with the main goal of sharing the top tips I’ve learned throughout this process and throughout the years. I hope it will resonate with you and help you in a meaningful way.
A lot of this, I filed away and forgot that it happened. And that’s married with a lot of things that have happened in the recent years of survivorship. Feelings of anxiety, stress, and a lot of emotion. Anxiety from scares of recurrences and a lot of tears. Working in a space where it can get pretty somber and where we’ve lost some pretty incredible people.
However, the main message I hope you take away is, you are not alone. After speaking with hundreds of other people impacted by a cancer diagnosis and having in-depth conversations, we really do share a lot of the same thoughts, feelings, and emotions. You are not alone. We are definitely not alone.
Tip #1: Emergency Department may lead you to faster care
If you already have some test results — at least a partial diagnosis or a start of one — it may be faster to get care if you go to the hospital emergency department rather than try and schedule an oncology appointment. That’s what I did and it worked for me. It was advice from our friend David, a doctor at UC San Francisco, where I went for my cancer care.
Five years later, I can admit: my husband convinced me at one point to sneak out to go all the way across the street — but it was just the other side of UCSF.
What I found is that actions first can lead to emotions later and joy can follow.
Tip #2: Break the monotony
Find moments to break up the monotony of treatment, the tests, and everything that feels so sterile. [I’m] not encouraging you to break rules per se but to live a little.
What I found is actions first can lead to emotions later and joy can follow. It’s not easy, but it can happen.


Tip #3: Seek out the humor
Seek out the humor in situations, if you can. Of course, there are some [days] where it will seem next to impossible. But if you can, it really can help.
For instance, the nurses and physician’s assistants who were taking my temperature [during my] first week of hospitalization, it was happening all the time and they were announcing the number so often, I joked that it sounded like a radio jingle.
For me, my family really was everything.
Tip #4: Draw your boundaries
Draw your boundaries and pick your people. You don’t owe anyone a call. Let people know about your diagnosis if you want them in your corner and you know they’re going to give you the kind of support you want and need.
Though I have to say, my people started a support campaign and it was incredible. Love poured in from my closest inner circles to people I may have only met a couple of times. It was truly uplifting.
But for me, my family really was everything — from home-cooked food at every meal to helping me with blood thinner injections twice a day, every day. And those really added up.
Tip #5: You are a big part of decision-making during treatment
Don’t forget, you are a big part of treatment decision-making and with that also comes the quality of life decisions.
I was two months from getting married when I was diagnosed. The cancer was very aggressive — diffuse large B-cell lymphoma with double expressor, they said. My hematologist oncologist and my family all wanted me to go into treatment right away. I didn’t want to. I had read about how one of my chemo drugs, Cyclophosphamide or Cytoxan, was a high-dose alkylating agent, which meant it could cause or contribute to infertility. That scared me.
I went ahead and froze embryos with my then-fiancé. Again, people may not understand, but it was so important to me and I knew that.


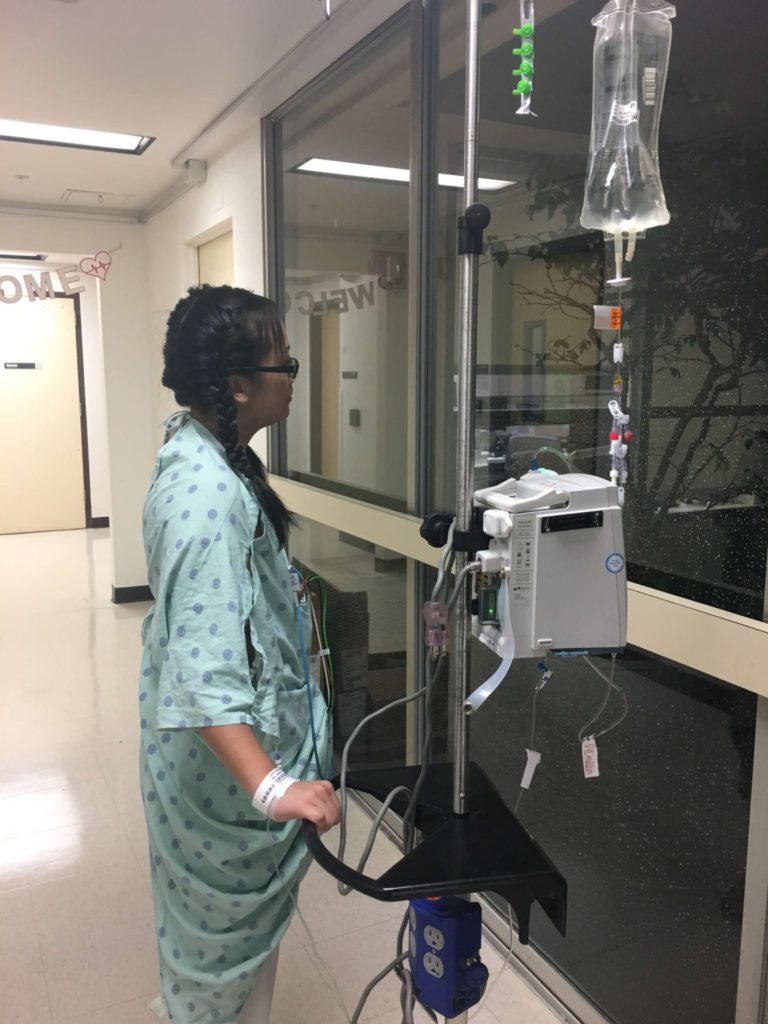
First up: ovarian stimulation with lots of shots. I got a lot of help with some of those shots. Then came the egg retrieval surgery and then embryo freezing. They did try to preserve my fertility during chemo by giving me a shot of Lupron beforehand. (Spoiler alert: My husband and I were blessed with two children in the last few years without dipping into our reserve. And for that, I am so, so grateful.)
Next up was the first cycle of chemoimmunotherapy. Always really unsettling to see the nurses put on hazmat suits just to touch the bags — and that’s bags of stuff that would be going inside of me.
By the end of treatment, more than 600 hours of infusion. The drugs killed both the bad and the good cells, and that’s where side effects came in.
You are a big part of treatment decision-making and with that also come quality of life decisions.
Tip #6: Don’t chase the side effects, especially nausea
By the time you feel it, it’s too late. And trying to get rid of nausea with the pills after can be really, really hard.
One of the worst side effects and most well-known is hair loss. Many other patients I spoke with who also lost their hair due to chemo shared the same experience as me. It started to fall after the second cycle and this does depend on the treatment you get.
The worst feeling was seeing clumps of hair on my pillow. That’s when I decided to do the first step of getting a haircut. The shaved side that looked like Cassie, the singer. It’s a style I wouldn’t have ever gotten on my own.
I never wore the real human hair wig I got that cost a ton. It was too itchy for me. I liked the hair that was attached to the baseball cap because the top was so much more comfortable; that material actually felt okay.
The worst feeling was seeing clumps of hair on my pillow.

Tip #7: There will be ups & downs and that is okay
This experience is not going to be a straight line and that is okay. Anxiety is natural to have. I’ve struggled to push it away, but I’ve had some scares of the cancer coming back.
I pushed for extra scans a few years after treatment. My doctor did not advise it, but she also gave me room to decide and I appreciated that.
This experience is not going to be a straight line and that is okay.
Tip #8: Wear loose clothing without metal
For those of you headed to a scan, wear loose clothing without any metal. I didn’t have to change into a gown because I wore loose clothes and sweatpants. No buckles, no metal, no zippers. If you’re a woman, you use bras usually — just don’t have any wiring. That way, you don’t have to change. Again, loose clothing in case you need IV so that they have access.
Tip #9: Earlier appointments may help you get results faster
Schedule your appointments earlier in the day. It may help reduce the wait time, depending on where you go.
What I found in the past, at least at UCSF, getting the morning appointment sometimes really does let you have these results later that day, which is amazing. As you know, “scanxiety” is a huge part of not wanting to wait. Just give me something to go on so I can have a plan if I need to have one.
Tip #10: Speak up for yourself!
We are the only ones who can and will. For me, there’s never been a day that passed without feeling around my neck and my chest for swollen lymph nodes because that’s how I got diagnosed the first time.
I don’t want to waste my doctor’s time. I’ve thought a lot about that. Oh, she’s too busy. She’s got more important cases than me. We feel that way and we think that. But there was enough for me to feel like something wasn’t right so I worked up the courage to see her in person, where she would feel around my lymph nodes and check me in person.
At the end of the day, we want doctors who will listen to our concerns. The good ones do listen. And when it comes to treatment options, for the most part, the good ones also encourage second opinions.

Life with and after cancer is not easy, it’s not pretty, and it’s definitely more brutal for some than for others. But there is a lot of hope.

Give yourself grace
I try to remind myself all the time and I find it’s pretty hard to do, but that is to give yourself grace and don’t “should” all over yourself. It’s something I really do need to internalize.
I’ve struggled a lot throughout the work I do for The Patient Story to fight survivor’s guilt. Why do I get to live when others don’t or didn’t? It’s especially hard after becoming friends with incredible patients and advocates, and unbearable when we lose them.
I’m not going to say who, but there’s someone I got to know — an incredible woman — and she’s been letting me know in her words, “It’s getting pretty bad.” She said, “I’m going down fighting.” When I read her message, it really stung because it’s happened multiple times in the last few years that I’ve been working on this and it just gets hard.
I’m still a work in progress, but I try to remind myself to celebrate each win that we get to amplify the voices of these amazing people.
4 replies on “Stephanie’s Story: 5 Years Cancer-Free”
Stephanie,
5 years NED? And so much life ahead of you? You’re a SURVIVOR, ma’am!
I just passed 2 years in December, and everyone treats me like “I made it!”, and Sloan-Kettering is no longer holding their breath. The stats that predicted Doom and gloom in the first place, now trend the other way, and I may not have another recurrence of cancer before I go.
Life, the web, and medical miracles, have given you the opportunity to create this wonderful website, which has already inspired me to do MORE to escape my funk and get moving again! Bless you for that!
Lease keep in touch.
Over 5 years NED is fantastic. I am so happy for you.
I am also so appreciative that you are willing to share your story AND all your hard work in putting together “The Patient Story” to allows others to do the same. CA can be a very lonely journey. The connection you feel when you read others’ stories is so powerful. Being allowed to share someone else’s journey allows insight in so many ways. For me, it is one of the best ways to process and “feel” my feelings. Love your questions, your tips and the way you encourage people to share.
Hi Stephanie, congratulations on surviving lymphoma. it is a very nice blog and i am so proud of you of how you have put out your journey. the tips given by you are so helpful and great. Non-Hodgkin Lymphoma is a type of cancer that generally develops in the lymph nodes and lymphatic tissue found in organs such as the stomach, intestines or skin. medications like Zandelisib, Odronextamab, along with meditation, optimism can help you treatnon-hodgkin lymphoma. companies like AstraZeneca, Regeneron Pharmaceuticals are developing the Non-Hodgkin Lymphoma drugs. A few days back i read a report by a marketing research firm which i think you will find helpful. please click here to read it. here
Great recommendations, Stephanie. So happy to read about your good reports. You help so many. xoxo