Justine’s Stage 3B/4 Rectal Cancer Story
Justine shares her in-depth story dealing with a rectal cancer diagnosis that started at stage 3B when she was just 30 years old, then shifted to stage 4 when the cancer spread.
This cancer thriver describes in detail undergoing extensive treatment: chemoradiation, surgeries, chemotherapy, ablation, SBRT targeted radiation, and the Y90 procedure. The surgeries were a result of complications, so Justine had to quickly learn how to manage life with an ileostomy bag, something that is usually temporary if the surgery had gone according to plan.
Justine also delves into how she navigated life after the cancer diagnosis: managing the loss of fertility and of independence, the importance of tending to mental health, and finding the silver linings. Thank you so much for being so vulnerable with us, Justine.

- Name: Justine L.
- Diagnosis (DX)
- Rectal cancer
- Stage 3B
- Metastasized into stage 4
- Age at DX: 30 years old
- 1st Symptoms
- Increasing number of bowel movements (up to ~20 a day)
- A little bit of blood in my stool
- Pretty soft stool (irregular)
- Treatment
- Concurrent oral chemo and radiation 5 days in a row, weekends off, total of 5 weeks
- Oral chemo pills: capecitabine (Xeloda)
- Radiation
- Surgeries
- Was supposed to be 1, but complications led to 4 additional
- Ileostomy bag permanent after surgery
- Chemotherapy
- FOLFOX (Oxaliplatin & 5FU)
- 13 cycles: 1 day infusion, 2 weeks off
- SBRT – targeted radiation therapy
- Ablation (minimally invasive surgical method where special probes used to “freeze” or “burn” cancers without usual surgery)
- Y90 (radioembolization)
- Chemotherapy
- Concurrent oral chemo and radiation 5 days in a row, weekends off, total of 5 weeks
- Video: Justine's Story
- Getting Diagnosed
- Describe yourself outside of cancer
- What were your first symptoms?
- Describe the colonoscopy
- A sudden cancer diagnosis after the colonoscopy
- How did you process the cancer diagnosis?
- How did you break the news to your loved ones?
- Guidance on breaking the news to loved ones
- Researching fertility preservation options
- When did you get the full rectal cancer diagnosis?
- How did you process the rectal cancer diagnosis and prepare yourself for treatment?
- Did you get a second opinion?
- Chemoradiation & Side Effects
- Describe the chemo pill and any side effects
- There were minimal side effects
- You were doing radiation at the same time as the chemo pill
- Describe the radiation process and any side effects
- No side effects but also not many changes to the cancer
- How were you able to manage those 5 weeks of chemo & radiation?
- Were you able to drive yourself to and from radiation?
- Surgeries & Complications
- Describe the surgery
- Complications: they found your large intestine dead, which required 4 additional surgeries
- What do you remember from waking up from so many surgeries and being in the ICU?
- How was the recovery from multiple surgeries?
- Describe the transition to solid foods
- How long did it take for you to be able to walk around by yourself?
- What kind of help might patients need after surgery?
- How was the transition from living with parents to living by yourself again?
- Ileostomy Bag
- Cancer Metastasis
- IV Chemotherapy & Side Effects
- Describe what the plan was with the IV chemo (oxaliplatin and FOLFOX)
- What was the chemo cycle schedule?
- What were the IV chemo side effects?
- What helped you get through the side effects?
- When did the side effects hit?
- Guidance on getting through such a long treatment
- How was getting through chemo during COVID?
- Any guidance for others who have to deal with something similar?
- More Treatment: Radiation, Ablation, Y90
- What was the follow-up schedule post-chemotherapy?
- A discovery of a tumor on your lung meant targeted radiation (SBRT) and ablation
- Describe the ablation
- Describe the Y90 procedure next
- Guidance for others going into Y90
- Any specific questions you wish you’d have asked before the procedure?
- More tumors → more chemotherapy
- Navigating Life After Cancer Diagnosis
- Handling your stage 4 cancer like a chronic disease
- Dealing with the loss of fertility
- What not to say to someone who loses childbearing options after cancer
- The importance of listening to your body
- Navigating the loss of independence after diagnosis
- How important was finding a counselor for managing your mental health?
- Importance of trying to find the silver linings
- The meaning behind this “warrior” tattoo
- Last message for others
- Rectal Cancer Stories
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Video: Justine’s Story
How I Got Diagnosed
Going Through Extensive Treatment & Managing Ileostomy Bag
Navigating Life After Diagnosis: Finding Silver Linings
Getting Diagnosed
Describe yourself outside of cancer
I am a kindergarten teacher, and I have been teaching for 9 years. That’s my true passion. That’s the biggest thing about me. I’m a teacher, and I love working with kids.

What were your first symptoms?
Summary: Increase in bowel movements, a little blood in stool, different stool consistency
The summer of 2018, I started noticing that I had an increase in bowel movements. It just slowly got worse and worse to the point where I was going up to 20 times a day.
I should add that part of some of my other symptoms were a little bit of blood in my stool and pretty soft stool, which wasn’t really that normal for me.
February of 2019, I finally said, “Enough is enough. I need to figure out what’s going on.” I went to my doctor, and we just decided to do blood tests and a colonoscopy to get to the bottom of it.
Describe the colonoscopy
You do a prep before. I started around 5 the night before, and I didn’t get to eat anything all day. I started drinking the prep stuff; it flushes out your system.
I woke up the next morning, drinking a little more, and it flushed me out the rest of the way. Then I just checked into the hospital for just an inpatient procedure.
I was sedated, so I didn’t know what was happening. They were able to look inside my bowels.
A sudden cancer diagnosis after the colonoscopy
I went in for my colonoscopy on February 11th, and when I went in for it, I was actually really worried that they were just going to say, “We didn’t find anything. We don’t know what’s going on.”
Cancer never crossed my mind.
Other things like Crohn’s had crossed my mind, ulcerative colitis, but not cancer. I woke up from my colonoscopy, and my boyfriend at the time was there with me.
The doctor came out and told me he had found a tumor, and my world basically came crashing down. That was not the news I expected to receive at all.
They hadn’t even done the biopsy, but he said, “I’ve seen this many times before, and there’s not a doubt in my mind that it is cancer.”
From there, everything was fast-tracked. I went straight in for some blood work, and everything just went really fast from there.
How did you process the cancer diagnosis?
I don’t think that I ever really did. I went from, “You have a tumor,” to calling my parents and letting them know what they had just found. I don’t know if I ever really did get to process it.
»MORE: Patients share how they processed a cancer diagnosis

How did you break the news to your loved ones?
I started with telling my parents because I am extremely close with them. They knew I was going in for the colonoscopy. They knew I’d been struggling with my problems.
That was an instant for me to call my parents. Then from there, it took a little while to tell other people.
Guidance on breaking the news to loved ones
I think you just have to do what you’re ready for. You can’t worry about hurting anybody’s feelings that you don’t tell right away. It’s not their journey. It’s yours, and you just have to do it when it’s right.
I had a friend ask to do a GoFundMe, which is really how my news got out. I was okay with that because it took it out of it being in my hands to let people know. They just found out through that, which for me worked, and that was good.
Researching fertility preservation options
I did not think of it. It was my mom who brought it up that there was probably going to be a possibility of that treatment causing issues for me.
I started looking into it after she brought it up and talked to my radiation doctor. Radiation is what was going to initially ruin having kids. I wasn’t going to hold or carry a pregnancy. Then I was going to become infertile, which was also caused by chemo.
I looked into it a little bit. It was going to take time. The odds weren’t the greatest, and it was a lot of money that I don’t have. Ultimately, I decided to forego going through with egg freezing just for those reasons.
I also wanted to be able to be around to possibly have kids, and postponing treatment wasn’t the best idea considering I was staged at 3B, so I was already pretty far along.
»MORE: Fertility preservation and cancer treatment
When did you get the full rectal cancer diagnosis?
I met with a couple of doctors. I had my surgeon, whom I met with, the radiation doctor, and then the oncologist for the chemo. I had 3 doctors I was working with.
I feel like I was staged by my surgeon by looking at my tumor, but I’m actually having a hard time recalling exactly which of my doctors staged me, just that they staged me at 3B.
They said, “This is the protocol for this kind of rectal cancer. You’re going to start with 5 weeks of chemo and radiation. You can do your chemo by pill.” I was still really active, so that was what was perfect for me.
For the radiation, they said, “You’ll have a small break. You have to go through a surgery, remove the tumor, have a temporary ileostomy, and then finish up with cleanup chemo.”

How did you process the rectal cancer diagnosis and prepare yourself for treatment?
I hadn’t heard of rectal cancer. I did not know a lot about it. It was just a whole new world opened up to me, a world I never wanted to enter.
I told myself early on I was going to make a positive out of a negative situation. That was just being really open about my story, sharing, so that hopefully, number one, anybody going through a tough time can be inspired, but also anybody going through cancer. Just staying positive.
Keeping to my normal schedule was helpful to me. I still wanted to continue teaching and being there for my students, and that was how I handled what I went through.
Did you get a second opinion?
Yes, I definitely looked at other hospitals. That was more later on in my treatment. In the beginning, I trusted where I was at. I trusted the doctors that I had. There was a lot of research behind rectal cancer and the treatment plan, so I trusted the treatment plan.
I felt really great about my surgeon. He had just come from another area. He was very highly recommended and experienced. I felt really good about where I was at and all my treatment. All my doctors were amazing, so I felt really good about it.
I think if it would have been a little bit more of a confusing cancer where there wasn’t as much research, maybe I would have gone with the second opinion, but it was supposed to be a pretty straightforward process.

Chemoradiation & Side Effects
Describe the chemo pill and any side effects
I had to take the capecitabine (Xeloda) 5 days a week for 5 weeks, so I got the weekends off. I really had not a lot of side effects, and I did really well.
I was going to the gym every day through those first 5 weeks of treatment and continued my active lifestyle and teaching in the classroom as well.
There were minimal side effects
I did not experience very many side effects. I did pretty well on it. They said that the pill has less side effects versus doing it intravenously. The pill can be a little easier on you.
You were doing radiation at the same time as the chemo pill
Yes. I’d do 5 days of chemo, 5 days of radiation. I’d get the weekend off, and then I’d continue that. I did that for 5 weeks.
Describe the radiation process and any side effects
It’s nothing like you envision. I don’t know what I envisioned, but I didn’t envision what happened to me. You just go in this room, they played the music I like, I lay on the table, and this big machine went around me and made some beeping sounds.
Then I was out. It’s silent. You don’t feel anything. You can have side effects from it, like burning. Luckily, I never experienced any of that.
No side effects but also not many changes to the cancer
It was good not to have side effects, but I also found out later on that my tumor really didn’t do anything through my first set of treatment. Maybe that’s why. The tumor didn’t shrink in size or anything.
How were you able to manage those 5 weeks of chemo & radiation?
I feel like I was maybe a little numb to everything. It was still a lot to process, but I went in every day after work and would go to radiation. My mom or dad met me there every day.
It was fast, and they couldn’t even be in the room with me, so I was always like, “You don’t have to be there.” Then after they did it a few times, I found that I really liked having that support.
I liked coming and seeing them, and then coming out of radiation and being able to see them. Other than just it being an extra place to go after work each day, it really didn’t disrupt my life a whole lot in the beginning.
Were you able to drive yourself to and from radiation?
Yes, I was able to drive.
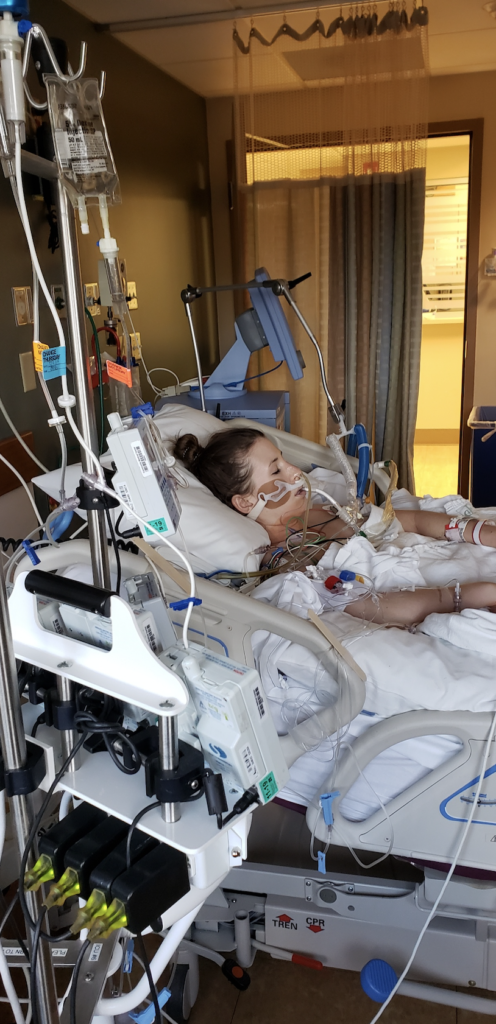
When I went in for surgery, they didn’t know that I would actually come out. That was definitely emotional.
Surgeries & Complications
Describe the surgery
They ended up removing my tumor and giving me an ileostomy. I ended up losing my large intestine and some of my small intestine, so my ileostomy cannot be temporary. It is permanent.
But for people going through this process, it would normally be a temporary thing for about 6 weeks, and then you get reconnected back up.
Complications: they found your large intestine dead, which required 4 additional surgeries
That was a really hard time. Probably the hardest part of my whole journey so far was this chunk of time that I had to spend in the hospital being completely helpless and dependent on everybody. It was a really difficult time, and I came through a lot of things that doctors did not expect me to, like being alive.
What do you remember from waking up from so many surgeries and being in the ICU?
The first thing I remember is trying to talk to everybody, and nobody could understand me. I was trying to sign language with them because I teach my students how to sign, and nobody knew sign language. Then I was trying to write messages.
I was super thirsty and just really uncomfortable. Then in a lot of pain. I really had no idea what had just happened to me. It still took being out of the hospital to fully understand what I went through when I was there.
How was the recovery from multiple surgeries?
Mine, again, was not quite straightforward. I went a lot longer not being able to eat, just because they kept having to go in. My bowels had to start working again, which took longer because I kept getting put under.
Your bowels have to wake up, and they have to see a certain kind of output before you can try eating. Then once you start eating, it’s just learning how to manage your ileostomy, or you can get a colostomy, too.
It’s just learning how to manage that and change that and all of that stuff that comes along with it. I had no idea what an ileostomy even was going into this. Even when I was told in my treatment plan, I still didn’t look it up. I figured I’ll cross that bridge when it comes.
The ileostomy phase came a little faster than I planned. I just woke up, and I have this bag. I had no idea what it entailed.
Describe the transition to solid foods
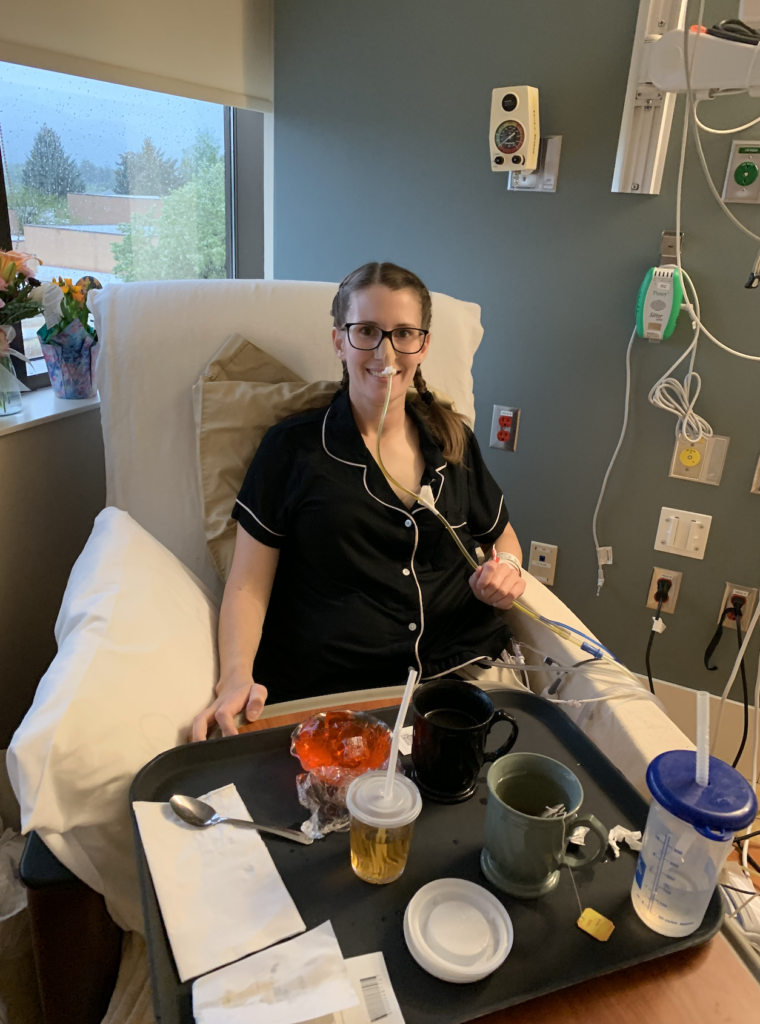
I finally had jello, some chicken broth, a little bit of juice, and tea. I was really excited about this because I went about probably 20 days without eating.
How long did it take for you to be able to walk around by yourself?
It was about 3 weeks in the hospital, 2 or 3 weeks. I would say most people would be up within a couple of days.
What kind of help might patients need after surgery?
You might be weak from being in the hospital and lying around. They usually say it’s about a week in the hospital, so it’s nice having help as you learn how to navigate your ostomy.
Sometimes you end up with drains, and the drains can be right in the way of where you need to put things. Having somebody who’s willing to help you with your ostomy is good. My mom and I totally teamed up and would change my ostomy together, at least in the beginning.
I was freaked out by it in the beginning, so having her to help me and guide me was really helpful. I would just say it’s just nice to have somebody there if you are struggling to get back on your feet. Not all people need that. My surgery experience was a lot different, more extensive.
How was the transition from living with parents to living by yourself again?
It was good. It was hard. I definitely was really weak, but I was very determined to get back into my own space. I did it, but it wasn’t easy.
The biggest thing was you lose a lot of your core strength, and I couldn’t lie flat, so it was important having enough pillows to prop me up. When I was at my parents’ house, I had a bed that could be raised. It was good to be back in my own space, though a little overwhelming to start doing all of the care on my own.

Ileostomy Bag
Learning how to deal with the ileostomy bag
I had a really amazing ostomy nurse who was very incredible, and she taught me a lot. A lot of it was also just self-research and learning stuff on my own. I became part of ileostomy groups on Facebook that I’ve learned a lot through. I would say that’s one of the biggest ways I’ve learned.
They take care of you in the hospital. It’s once you get out that you have to learn how to do it.
I definitely like to try to do things on my own, like trying to empty my bag. I have easy bags now. They’re just Velcro, but there were these weird clips when I was in the hospital that you had to try to learn how to use.
Just when you empty your bag, getting it in the cap and not everywhere else. You have to learn how to change it. You have a wafer that sticks to your skin. That only lasts so many days, so you have to learn how to cut the hole for your stoma and put that on every so many days. I guess throughout the process of being in the hospital, I was learning how to do all of these things as well.
Describe in detail how you manage the ileostomy bag day to day
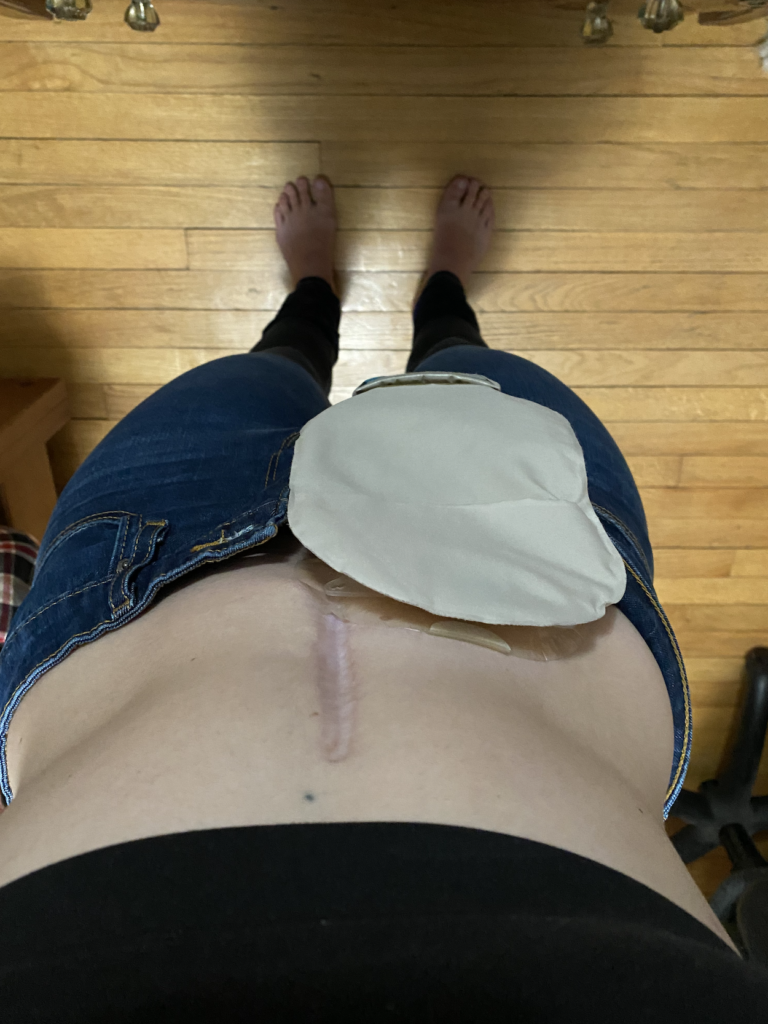
It’s just basically a giant sticker that sticks to your belly. You don’t really get to choose where it goes, and it covers whatever. I never have a belly button because it’s always covered by my stuff. It covers some of my scar.
You don’t get to pick how high or low it goes. Even just figuring out how to dress after was a really big obstacle, as well as finding tools to help me dress and just feel normal. You would never know I have my ileostomy just looking at me. It’s all very hidden.
Any guidance for others on managing the ileostomy?
I would say my biggest thing is research. Find groups that are ileostomy groups. They’re super helpful. People ask really great questions.
Also see if you have an ostomy nurse in your area who will be able to help you and guide you once you are recovering and getting out of the hospital. They’re very helpful.
There were times I was going through leaks, and I couldn’t figure out why I couldn’t get stuff to stick on me and stay. I’d go to see her. She could help me, but also, I just researched a lot and used the groups that I had.
How have you dealt with the transition on body function and image?
I still struggle with this at times. I’m very used to what my body used to be capable of. It can be frustrating being 32 years old and not being able to do what I used to be able to do, but you need to give yourself grace and accept the new body you have.
These bags save your life. In the realm of things, most people that have a bag wouldn’t be here today if they didn’t have the bag. I had to learn to accept that.
I’ve definitely worked with a counselor on just accepting it, feeling good about it, being in a relationship, having a bag, and being intimate.
There are a lot of obstacles to get past, but there are a lot of people out there who are willing to share ideas and stories that can help you through having an ileostomy.
Any tricks or tips with managing the ileostomy?
I definitely found that having a cap or something to empty into was easier in the beginning. I kneel down a lot and empty into the toilets when I’m at home. I find that easier. Facing the toilet versus facing away is easier to empty for me. Everybody finds what works for them.
Cancer Metastasis
During scans pre-cleanup chemo, your team found your cancer had metastasized
Once I was strong enough to go through cleanup chemo, my team had me come in for scans, just to give them a baseline of how everything was looking. In those baseline scans, they found that my cancer had spread to my liver.
Again, not the news I was ever expecting. It never even crossed my mind that that would have happened. It’s definitely another really hard conversation.
They decided to continue. I got these baseline scans. I was supposed to get my port on Monday and start chemo. They decided for me to get my port, and then they had to come up with a new plan of treatment for cancer that had spread, which is considered metastatic.

How did you process another sudden change in plans?
I still wonder how I got through all of these moments. I remember when my doctor called, I was in the shower, just crying.
You have to allow yourself to still breathe, but then for me, just continuing on and still sharing my story and continuing doing what I love is really important to me.
Cancer can become your story and what consumes your life. That’s the topic all the time.
Still, just having a little bit of normalcy was important for me. My students are a huge drive for me to even keep fighting, in all honesty. I adore them, and I just want to be a good role model for them and just persevering through whatever life throws at them.
That’s really important to me, just continuing to live my life, take the news in stride, and allow myself time to cry when I needed to cry, but then get back up and keep going.
How was it waiting for the results of your tumor biopsies?
I definitely had to learn. I’m a big planner, and I like to know what to expect. I like to plan and stick to that plan. Cancer kicked me in the ass and said, ‘You’d better lose that right now.’
I had to learn very early on that I couldn’t plan. I had to really just take it day by day. Honestly, when they told me I had tumors on my liver, I really didn’t even feel like I needed a biopsy to confirm.
I already had cancer. The fact that it had spread was not shocking. For me, the biopsy didn’t hold a whole lot of weight. I already knew and was thinking, “Okay, this is the deal.”
I still did not really realize just what metastatic cancer meant, though. “You’re treatable, but you’re not curable,” is how the doctors described it. I never get to escape this. This is always going to be part of my life.
That’s something I still struggle with from time to time. That’s a hard realization, but again, I allow myself to feel those feelings and then continue on.
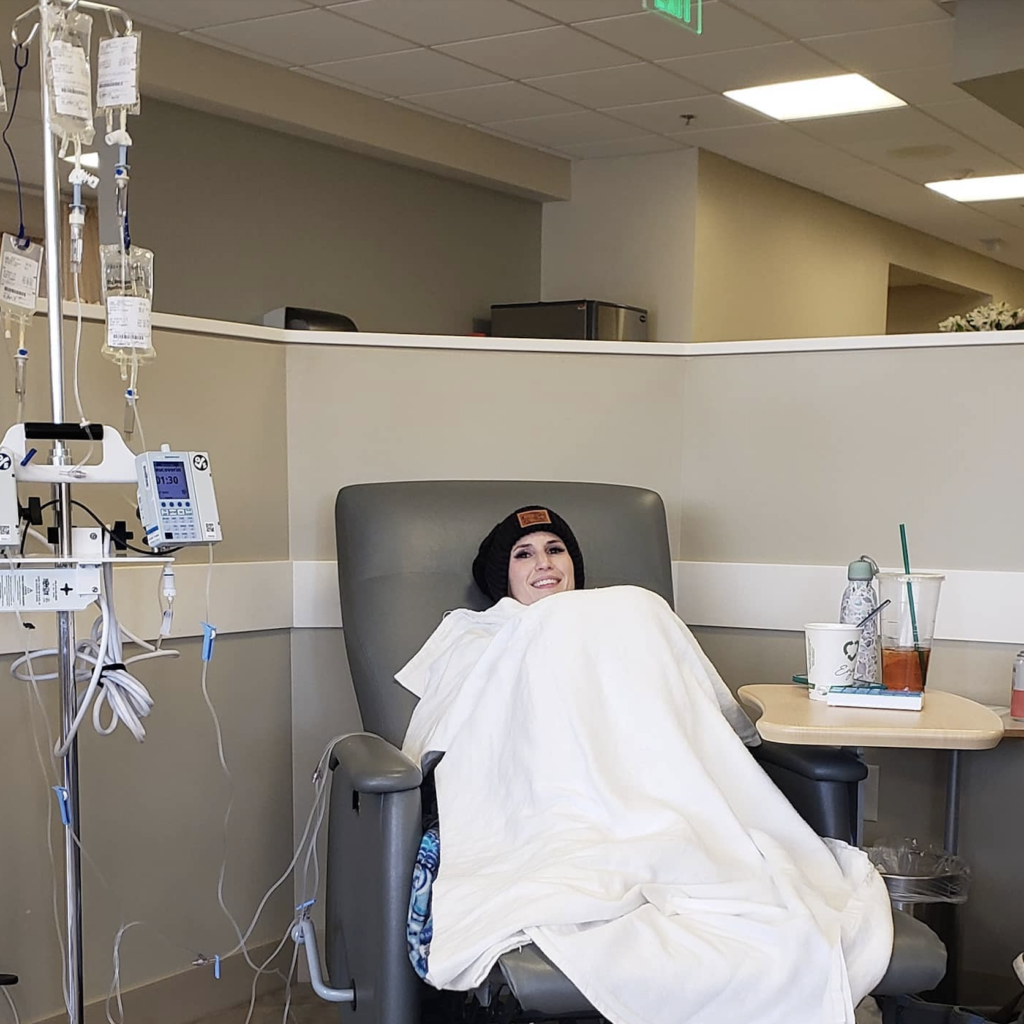
IV Chemotherapy & Side Effects
Describe what the plan was with the IV chemo (oxaliplatin and FOLFOX)
The plan was to start with 8 rounds of chemo as the cleanup version. I ended up going through about 13 rounds just because they kept trying to get my tumors a little smaller in order to do procedures.
It was back and forth, like, “You’re going to do 8,” and then they would reevaluate, and then they’re like, “We want you to do 2 more rounds.”
I went back and forth a lot. I never really knew just how many I was going to end up doing. The intravenous chemo was definitely a lot rougher.
When I was going through it, I’d like to think I was doing really well, but looking back, it was very miserable.
What was the chemo cycle schedule?
Summary: 1 day of infusions, 2 weeks offs
It was a day of infusions. The FOLFOX I would get infused for a day in the cancer center, and then I’d leave. I’d get hooked up to another chemo, which was in a ball that I would then carry for 3 days while it went into me.
Then that ball would empty after 3 days. I’d get to disconnect, and then I’d get to wait until I would go in 2 weeks later.

What were the IV chemo side effects?
It made me extremely sick, a lot of vomiting, no appetite. You get a cold sensitivity from it that is terrible. I couldn’t eat anything cold or drink anything cold.
I had to heat everything up, or else it felt like shots of glass in your mouth. We live in Montana. Even the cold to step outside was tough. I was going through this starting in September, so I had to go through this in winter as well.
I’d step outside, and just to even breathe through my nose, my nose would feel like pieces of glass in it. It hurt my fingers to touch anything cold. I would say the cold sensitivity was definitely a really big thing. Then I ended up with neuropathy in my fingers and toes.
What helped you get through the side effects?
I would heat my cereal up, which is so gross. I wore gloves. I’ve got a vest that was heated with a battery. I had this vest I wore every day over my clothes that was heated because I was miserable.
I had no body fat and would get cold easily. I did that. I’d just always been trying to dress really warm to help warm things up.
When did the side effects hit?
As soon as they start infusing, the cold sensitivity starts within 10 minutes. Then the cold sensitivity in my mouth would subside about a week and 2 days after, and then I could start maybe eating a little bit of cold stuff again.
Then I’d basically start chemo again, and then they would go back. I’d get maybe 3 days where I could eat things that weren’t totally warm.

Guidance on getting through such a long treatment
Physically, make sure you have a good nausea medication. That was helpful to me. Mentally, just staying positive and knowing that it’s temporary and that you will get through it.
Use the people or your support system around you. When people ask how they can help, don’t be afraid to ask for things.
I am not super good at asking for help, but if it’s that you need a meal, don’t be afraid to ask people for those things so that you can focus your energy and your strength on treatment and fighting.
How was getting through chemo during COVID?
It definitely sucked. There’s no easy way around it. I really counted on those people being there with me and just entertaining me through it.
It ends up being a long day. It’s not comfy. You don’t feel well, and you like having those people there with you to chat. To have to do it alone was hard.
Any guidance for others who have to deal with something similar?
Just make sure you FaceTime people. I definitely would sit there and FaceTime. If you have a good show or a good book, make sure you bring it, but if you’re really missing the people that help you get you through the tough time, use FaceTime.

More Treatment: Radiation, Ablation, Y90
What was the follow-up schedule post-chemotherapy?
I got scans. I’d go through some rounds, they’d do some scans, and they’d check in. I started seeing some doctors down in Portland at OHSU.
They were all collaborating, talking about my case, and deciding what they felt was the best plan of action. It’s been a lot of back and forth because mine hasn’t been super straightforward.
One time, they wanted me to do 2 more rounds, and then they would do scans. I went through that a lot. Again, just being able to take it day by day and one treatment plan at a time, not looking at the big picture.
Just looking at, ‘Okay, what is happening now?’ versus, ‘Okay, they’re going to do this, and then this is going to happen.’ That doesn’t always work out that way.
There was a time I was going to leave for a procedure, and they called me the day before and canceled it. You don’t know. I found that setting my mind to something didn’t do me any good.
A discovery of a tumor on your lung meant targeted radiation (SBRT) and ablation
I went through targeted radiation and an ablation procedure as well during that time. Ablation was done on my liver, and targeted radiation, which is called SBRT, was done to my lung.
SBRT was painless like radiation, where you’re just in there. I did have to do some breath-holds. I build my breath for like 40 seconds, which was the toughest part, and I had to do that about 15 times per treatment. I did 5 days of this.
I’d come each day and go through the same thing, but they’d do some baseline scans and some mapping and give me my tattoos that help line them up.
Again, it’s just painless, and you don’t really know anything’s happening.
Describe the ablation
For the ablation, I actually had to stay in the hospital and get put under. They use probes and stick them through your skin. They’re hot, and they burn the tumors. I had a couple of spots that they went in on.
When I woke up, it was a little painful, but it was a fairly easy recovery.
Describe the Y90 procedure next
Y90 is where they insert radioactive beads into my liver. They did a bunch of mapping through my arteries to check that my blood flow went through my liver.
They didn’t want to put these beads in and just have them go all over and ruin parts of my liver that are still good. They focused on my right lobe first, and they put a catheter in to block blood flow to certain parts of my liver.
Then they do this all through an artery in your groin. It was a day of all this mapping and then figuring out the best path to insert them. Then the next day, I’d come back, and they insert the beads.
It was an interesting procedure. I didn’t realize just going in through your groin, that major artery, how big of a deal that was and how serious that can be. That actually caused me the most pain.
You’re awake for it all because you have to hold your breath at times, so you’re sedated but aware and able to hold your breath. I can see all this stuff going, which is a little freaky.
Guidance for others going into Y90
Research. Ask your doctors as many questions as possible. I don’t feel like I asked enough questions to fully understand what I was going to go through.
Again, sometimes that’s what’s best for me, just not knowing exactly and just going in. I’ve just learned to really endure a lot of pain, and I don’t get as nervous anymore. I just go with it.
I trust my team, and I just get through it. I need the trust so much because I’d normally say, “Embrace your family members and whatnot.” But they don’t get to be there with you during something like the pandemic. The relationship with your medical team is helpful.
I had really great nurses, who were very comforting. Making sure you’re confident where you’re receiving treatment is also really helpful so that you just feel comfortable in their hands.
Any specific questions you wish you’d have asked before the procedure?
Maybe just more of what it entailed. I just go with it, but also, I’m doing this at a distance because of the pandemic. I don’t always get as many appointments as you would if you were in person.
More tumors → more chemotherapy
In March 2021, I had an MRI and CT scan to see if the Y90 worked. Unfortunately, I received more devastating news. The Y90 didn’t work.
My tumors have grown, and I have yet another new one. The new one is in a location that can’t be determined if it’s a tumor within the liver or a lymph node. If it’s a lymph node, that is extra concerning. Lymph nodes enlarge when cancer is breaking through the current location, which in my case is my liver, and try to spread elsewhere in the body.
One of my doctors at OHSU said chemo is going to be the next step. He said we’d be chasing our tails trying another procedure to see if it works. In the meantime, cancer can grow and spread, and we’d find ourselves wishing we had done it sooner.
I would have to agree. I’m not willing to do another procedure that comes with risks and side effects that we don’t even know will work. They will be presenting my case at the tumor board.
This is a step he feels we will need because the chemo they will recommend will be a bit unorthodox, and insurance will fight it. This means the chemo I will go through is not one I’ve been through before.
I don’t know when I’ll start, how long I’ll go through it, or what side effects will be. I will hopefully learn more soon. As much as I hate chemo and everything that comes with it, it is something I know works.
I’m grasping at straws trying to understand why I can’t catch a break. I know many are at a loss for me as well.
All I can do is trust the doctors know what they are doing, trust we will find something that works, and keep fighting. Your continued love and support is appreciated so much.
Justine on her CaringBridge
Navigating Life After Cancer Diagnosis
Handling your stage 4 cancer like a chronic disease
This is my new norm, I guess. It’s just going to be a part of my life — appointments, scans, a constant fear, but also just being thankful that I’m here and embracing the time I do get, regardless of how long that is.
Dealing with the loss of fertility
That was definitely a huge blow to me. I’ve always dreamed of having kids. I know there’s other avenues, but it’s all super hard.
What not to say to someone who loses childbearing options after cancer
Don’t tell me there’s other ways that you can have kids, but that’s not the only way. It’s not what somebody wants to hear when that’s what women do. We have kids. I don’t really want to hear that.
The importance of listening to your body
Definitely just listen to your body. If you feel like something’s wrong, go to a doctor. If they don’t listen, go to another doctor.
I’ve met other ladies on this journey who were not as lucky and did not have a doctor who listened as well. It’s easy for them to sometimes say, “Well, you’re too young.”
Then they’re not the doctor for you, and you should seek advice somewhere else. Just be proactive.
It’s easy to worry about the cost of a doctor’s appointment, the cost of a scan, but I guarantee you the cost of what you would get if you are diagnosed with cancer is far greater, so it’s just important to just be on it.

Navigating the loss of independence after diagnosis
I still struggle with it, and it’s definitely something that I talk to my counselor about, because it’s hard to ask for help. I was a very independent person that did everything for myself. Then I was diagnosed with cancer, and I really had to ask people for help. That’s hard.
Cancer takes so much from you, and that’s just another thing. I have to also remind myself I won’t always need this help.
My sister tells me that there are a lot of people who need help constantly throughout their lives. I’m just needing it all at once. I just have to remind myself that it’s temporary, and it won’t always be like this.
How important was finding a counselor for managing your mental health?
It’s really hard. I feel like when you go through cancer, you’re constantly shielding everybody from your real feelings. You’re shielding them from the fact that you’re fearing dying. You’re shielding them from the fact that you have a pretty major illness. You’re always shielding people and not getting to really express yourself exactly how you might want to.
A counselor is just a great way to be able to let those things out without having to protect anybody else’s heart or feelings. You get to just go there and talk, and it can be what you want it to be. I have found it very helpful.

Importance of trying to find the silver linings
Finding the silver linings has been my biggest tool for getting through things. It’s easy to get bogged down by all the crappiness and hard times, but just being able to find little silver linings makes a difference.
For me, my sister and I didn’t have a very good relationship before all of this. A huge silver lining is that we do now. The things that it’s done for our family are big silver linings, so I just try to find those. Sometimes, I have to dig real deep for them.
There are things that have happened, and I’ve had to dig deep for them, but I always try to find a silver lining in everything that I go through to help me get through it and just remind myself.
The meaning behind this “warrior” tattoo
Going through what I did was a huge inspiration to me. I always said that when I beat cancer, I would get it. Everything just kept dragging on. I don’t ever fully get to beat it, so I finally was like, “I’m just doing it. I have no other tattoos other than my radiation tattoos,” which I have plenty of.

This tattoo, I designed on my own with a little help from pictures. The 4 dots on the W stands for my stage 4 cancer, and the ribbon is for cancer. It brings me a lot of strength when I look down at it.
Warrior has been the word that a lot of people use to describe me and how I handled the situation and journey, so it’s just a really meaningful word for me and brings me strength.
Last message for others
I think I’ve said it all, but just to reiterate: it’s your journey, and you’ll find what works for you. Don’t be afraid to reach out for help and ask for help.
There are lots of really great groups that you can find to help you. Counselors are very helpful, and just stay strong and positive.

Inspired by Justine's story?
Share your story, too!
Rectal Cancer Stories
Joanna H., Rectal Cancer, Stage 3
Cancer Details: Rectal adenocarcinoma
1st symptoms: Rectal bleeding, bloating, stomach aches
Treatment: FOLFOX chemo, radiation
Catherine P., Rectal Cancer, Stage 3
Cancer Details: Rectal adenocarcinoma; 98% of rectal and colon cancers are adenocarcinomas
1st Symptoms: Rectal bleeding, constipation, bloating
Treatment: Fertility treatments, chemo, radiation, tumor resection surgery
Jackie S., Rectal Adenocarcinoma, Stage 3B, Lynch Syndrome
Cancer Details: Rectal adenocarcinoma; 98% of rectal and colon cancers are adenocarcinomas
1st Symptoms: Blood in stool, constipation
Treatment: Chemo, radiation, surgery, immunotherapy
Maria A., Rectal Cancer, Stage 3C
Cancer Details: 7cm mass found
1st Symptoms: Fatigue, weight loss, fast heart rate, bladder infection
Treatment: Chemo, radiation, surgery for tumor removal
Justine L., Rectal Cancer, Stage 3B/ 4
Cancer Details: Metastasized to stage 4
1st symptoms: Increasing bowel movements (up to 20/day), some rectal bleeding
Treatment: Chemoradiation (oral pill capecitabine + radiation), colectomy, FOLFOX chemo, SBRT radiation, cancer ablation, Y90 (radioembolization)
Amy H., Rectal Cancer, Stage 3B, Lynch Syndrome
Symptoms: Feeling off, abdominal pain, bloating, weight loss, blood in stool, thin stool, massive shift in bathroom habits, exhaustion
Treatment: Radiation, chemotherapy (Xeloda & oxaliplatin), surgery (total proctocolectomy with ileostomy, APR reconstruction, and radical hysterectomy)
Symptoms: Fatigue, anemia, irregular bowel movements, loss of appetite, heavy periods Treatment: Laparoscopy, chemotherapy, partial hysterectomy
Ananda P., Rectal Cancer, Stage 3B
Symptoms: Intermittent rectal bleeding
Treatment: Surgery, chemotherapy (FOLFOX)
Jelena T., Colorectal Cancer, Stage 3
Symptoms: Blood in stool, change in gas
Treatment: Chemotherapy, radiation, surgery








3 replies on “Justine’s Stage 3B/4 Rectal Cancer Story”
Justine,
My prayer for you is that God will perform a miracle on your body taking every single cancer cell away and cleanse your body completely. You are a tremendous inspiration to so many people. I bet your students are crazy about you! Keep fighting and ask God to take it all from you. You will be in my prayers Justine.
As a medical professional and a relative of Justine’s I’m extremely impressed by the Patient Story format; the video’s, the time line, the story and the photos give an accurate over-view of how she has dealt with her diagnosis. Justine’s courage and strength during this period of her life is remarkable and gives her friends and family hope and inspiration. She is a fierce warrior in the very best sense of that concept, someone who is challenged every day and who accepts those challenges in a positive way and does the best that she can be/do for herself, family, friends and community. We love Justine and her family.
Mark, thank you so much for sharing this. I feel blessed to have been able to get to know Justine and her story so well.