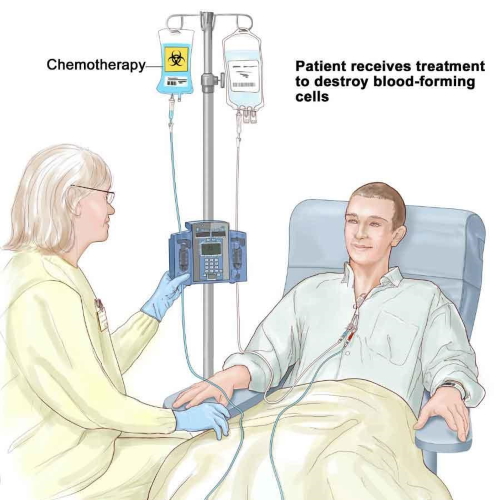
CAR T Cell Therapy
David Miklos, MD, Ph.D
In this interview, Dr. David Miklos talks in-depth about CAR T cell therapy, mantle cell lymphoma treatments, allogeneic transplants, and gives his thoughts on future therapies.
David Miklos, MD, Ph.D is an experienced and passionate specialist in blood and marrow transplants, as well as immunotherapy research. As Chief of BMT & Cell Therapy, and Clinical Director of the Cancer Cell Therapy program at Stanford University Medical Center, Dr. Miklos spends his time not only seeing patients but also focusing on the latest science in cancer therapies.

- Name: Dr. David Miklos
- Specialty: Blood and marrow transplant
- Roles:
- Chief of BMT & Cell Therapy
- Clinical Director Cancer Cell Therapy, Stanford University (2016 – Present)
- Experience: 25+ years
- Provider: Stanford Medical Center
We’d like to cure more and more diseases. What is cured?
People ask me all the time, ‘Am I cured?’ The difference between remission, where we have no measure of your cancer anymore on a scan or bone marrow or blood test, and a cure, is time.
Dr. David Miklos
- CAR T Therapy
- Video: Dr. Miklos on CAR T Therapy
- What is CAR T therapy in layman's terms?
- What is CAR (chimeric antigen receptor)
- CAR T expanding quickly
- Stanford’s latest work: CAR 22
- Disease progression and changing targets
- Promising results
- Role of CAR T therapy
- Newest study: ZUMA-2 clinical trial
- New clinical trial
- What are the drawbacks of this newest therapy
- Balance between therapy efficacy and adverse effects
- Why patients should consider clinical trials
- State of current and future therapies
- Dr. David Miklos' Full Interview on Video
CAR T Therapy
Video: Dr. Miklos on CAR T Therapy
What is CAR T therapy in layman’s terms?
It’s the use of the patient’s own lymphocytes. These are the immune cells that provide us our education, these are the things we’re talking about with COVID as to whether or not you have antibodies or immune responses. The question is how are we going to vaccinate ourselves?
We understand the power of the immune system. We know that there were no antibiotics until 150 years ago. We know we’ve had 10,000 generations of pond scum up to human beings at this point in evolution.
All that depended on our immune system but we haven’t been able to harvest the immune system to cure these aggressive cancers – until now.
The opportunities to try and vaccinate a cancer have been disappointing and so the general approach of the cancer cell therapy or CAR T program is to hijack the patients’ own immune cells to remove the lymphocytes from the body using a very simple procedure, apheresis, just like you see in the Red Cross donation centers where patients are giving platelets.
No pain, three hours, piece of cake.
What is CAR (chimeric antigen receptor)
Take those cells into the laboratory and introduce a new gene. We call that a chimeric antigen receptor, the CAR. And that modification of the lymphocytes becomes permanent in those cells, but it doesn’t go into the rest of the body.
You’re not going to become a GMO like the corn in Iowa.
We are modifying the lymphocytes. Those super-charged cells after one week of manufacturing and one week of safety evaluation in a lab, are brought back to the patient, frozen in liquid nitrogen, which is not only for ice cream, and those cells are then introduced back to the patient’s body in the same catheter that earlier the lymphocytes came out.
They expand from two million cells to 20 billion cells in seven days. It’s variable depending on what cell therapy we’re talking about.
The thing about that is cells dividing every seven hours and frequently, after a week of expansion, the CAR modified T-cells represent 50-percent of the white blood cells in the patient’s body.
These are cells that can do four things that have never been done in cancer.
These are cells that are proliferating in the patient’s body, localizing to the tumor, able to kill with cytotoxic killing, like we use for viruses like influenza, and then they persist, providing you surveillance until the cancer’s all gone.
In fact, some of these CARs are designed to last for years. Others are designed to simply go away over the next four to twelve weeks.
That’s the value of the excitement of the CAR T program. It’s a paradigm shift of using the patients’ own lymphocytes to kill cancer with all the power of the immune system in a way that was never done before.
CAR T expanding quickly
This was pioneered by Dr. Carl June and Steven Rosenberg at University of Pennsylvania and the National Cancer Institute, but really became available broadly to the lymphoma patients only in 2016.
I remember back to February 2016 when we treated our first patient here at Stanford. Now, we are treating 120 patients this year at Stanford with the CAR T-cells.
We anticipate increasing about 50-percent per year.

Stanford’s latest work: CAR 22
The initial work was targeting CD19, a series of cell-surface proteins and they have numbers. The B-lymphocytes important ii lymphoma and leukemia were the first successful use of CAR T. We have three targets: 19, 20, and 22.
Most of your patients have had rituximab, the monoclonal antibody, and I’m sure they recognize that bottle that infuses over three to four hours of clear liquid. That’s targeting CD20, but that’s an antibody.
You put the antibody in and it doesn’t grow, localize, or do any of the things we just said. It’s effective, don’t stop taking your rituximab. It’s an important part of our therapy.
But soon we’re able to go after additional targets. If a patient was treated with an axi-cell (Yescarta) or tisa-cel (Kymriah), or soon, liso-cel from the Juno work we expected to be approved, those are three soon-to-be commercially approved (axi-cel in October 2017, Juno’s liso-cel we expect later this month), three CAR T-cells commercially available that the doctors are choosing which one’s the best for that patient.
They’re all targeting the same protein and using the same binder on the surface of the cell. They’re all very similar, actually.
Creativity means let’s go after a new target.
Disease progression and changing targets
One of the biggest problems our research has shown that the patients receiving the CAR therapies who have disease progression, frequently two to three months afterwards, that progression happens in half the patients and half the patients have long persisted remissions that are out at three and four years now.
But the patients who have the progression – why? Why did the CAR fail? What we’re finding to be the most common reason is the lymphoma cells, the cancer cells stop making the target.
So what was there before as the target that the CAR bound onto and then interacted with and then was able to activate and kill, when the target disappears, the CAR has nothing to bind.
So antigen loss of CD19 can only be overcome by going to a new target. Here at Stanford we have been fortunate with our programmatic leader, Crystal Mackall, who came from the National Cancer Institute, and has brought some of the basic science constructs that are necessary to move into these new targets.
We’ve had great success recently with the target of CD22. Similar to the rest of the CARs it’s a chimeric antigen receptor, uses the patients’ own lymphocytes, harvested but manufactured here at Stanford in our own GMP laboratory.
That’s the clean room laboratory, like you see with Intel, the guy’s in a white gown dancing around.
That clean room mentality so that we can ensure that the virus goes into the lymphocytes, that it’s safely matured and that we collect enough cells after a week of production, and we bring them back to the patient.
Promising results
The excitement here is that in patients who had progressive disease after axi-cel, or tisa-cel, that we have witnessed seven out of nine of these early patients on clinical trial achieving responses.
Five out of nine in complete remission, and those durable remissions in our lead two or three patients are now out to a year. They have very low toxicity, low cytokine release problems that your patients probably know about.
What happens after CAR is you feel like you have the flu with fevers and aches, sometimes low blood pressure and cough or low oxygenation. We can manage that with steroids and a special drug called tocilizumab. Those toxicities are very low, so that’s very exciting to us.
Now please don’t run out to all your local hospitals asking for CAR22, this is an investigation being done here at Stanford where we are able to help patients who’ve had progression after axi-cel and patients do come from all over for this.
There are other clinical trials also targeting and helping patients who have had progression after they’re commercially available.
One of the most exciting areas there is instead of using the patients’ own lymphocytes, why not take cells that haven’t gone through two or three rounds of chemotherapy, haven’t existed for 60 or 70 or 80 years in somebody’s body, why not take a 21-year-old super donor lymphocytes, from someone healthy and fit, that has been made stealth-like by removing some of the histocompatibility markers, immune cells that would be rejected.
Those stealth cells are also expressing CAR T-cells. Some of the companies doing this work are Precision Bioscience and Allogene. They have different targets, CD19 and CD20.
And again, we’re using those opportunities to help our patients here at Stanford. I’m sure some of your patients can find those locally in centers near them.
The allogeneic approach is very exciting because you don’t have to wait to make the cells. You already have the cells in the liquid nitrogen freezer. It’s kind of one size fits all. You know how good those cells are because you’ve seen them function in other patients, previously.
So there’s potentially a lot of advantages to these allogeneic cells, but of course we have to make sure they will grow and expand, and not get immunologically rejected by the patients.
These are still early clinical trials, but very exciting opportunities for patients who have not benefited completely and have not gotten a durable response from the CAR T’s that are commercially available.
That’s how I think about the development of CAR T.
These are clinical trials. Patients can come to academic centers and participate in clinical trials. Other centers are doing very exciting work. Please don’t think we have all the answers at Stanford. There’s very exciting work, as you would imagine, the top 30 large cancer centers in this country. We’re very fortunate to have the support of the patients and their families.
In 2016, before we started our CAR therapies and what turns out to be axi-cel or the commercial trade name of Yescarta, the benchmark study of what happened to patients who didn’t go on to CAR T with relapsed/refractory lymphoma who’ve had three lines of therapy previously, was dismal.
That was an experience we’ll never want to repeat. The median time to death was five to six months. The one-year survival (rate) was 15-percent.
Now, with the approaches of Yescarta, tisa-cel, and I anticipate liso-cel, the one-year survival rates are 85-percent. We think with having additional therapies we can use in patients who are progressing, we’re going for 100-percent.
Who wants 85-percent? Let’s go for 100-percent.

Role of CAR T therapy
The axi-cel therapy was the first FDA-approved treatment in large cell lymphoma. That company is called Kite. They were purchased by Gilead. They brought forward a very similar construct.
The actual molecule that is placed into the patient’s lymphocytes is exactly the same as what’s been used for the last three years in large cell lymphoma. So it binds the same CD19 again, same story, here comes the CAR. We’re going to bind and we’re going to then kill the cancer.
It’s prepared in a very special way because mantle cell frequently has lymphoma in the blood, so we have to separate the lymphocytes away.
That’s the unique difference between Tecartus and Yescarta. Otherwise, they’re nearly identical therapies.
And the prep to do this is the apheresis, the places where you’ll receive the therapy, the lymphodepletion chemotherapy, and the three days before we put the special cells in. It’s all the same. The follow-up stay in the hospital, seven to ten days, staying locally for 28 days, it’s all the same.
The expected toxicities of cytokine release syndrome, that’s the fever, achy, flu-like symptoms, or the confusion and neurological problems that can follow patients who have had the cytokine release syndrome, again, very similar incidents.
Newest study: ZUMA-2 clinical trial
Here’s the excitement: the excitement is in that study you addressed called ZUMA-2, which began in 2017, there were 60 patients treated and this overall response rate was 93-percent.
The overall complete response rate, couldn’t find the cancer, was 67-percent.
Two-thirds of the patients, 28 days after given this Tecartus infused in their body, had no measurable cancer, a complete response. That response has remained durable. The publication that is responsible for the FDA’s approval showed 27 months of follow-up in patients.
That’s just over two years, so let’s not get carried away. We have two years of follow-up and in that population, the response rate was 43-percent remaining in complete response and 67-percent overall response.
So it’s very durable. Probably even more durable than what we saw in the original treatment with axi-cel in large cell lymphoma. There are similar side effects and it still needs to be done inside the hospital at centers that have experience managing patients with CAR T therapy. The higher response rates and they appear to be very durable treatments.
These are for patients who had had three lines of therapy previously, so they probably had CHOP, or bendamustine and rituximab, they probably had ibrutinib as one of the therapies. That trial required they had a drug that targeted the Bruton’s tyrosine kinase (BTK).
The FDA, when they made the approval of this therapy in July, recognizing what a game changer the therapy offered patients, did not require patients go through three lines of therapy.
The FDA has authorized the treatment in second line and I think that’s because they really want to help patients achieve long-term disease-free survival and benefit.
Now, physicians will have to decide who should receive BTK inhibitors and who should go right on to CAR T-cells, and that’s discussion with the patients and the families. That really is still being worked out.
»MORE: Read patient experiences with immunotherapy

New clinical trial
We’re going to be doing a new trial where we’ll be looking at patients who’ve had ibrutinib upfront or who have not had ibrutinib yet, and using the same therapy to see what the true incidents of benefit is in that second line.
But in the meantime, there are centers that can provide commercially-available therapy with Tecartus today. If somebody’s gone through all the available therapies, that’s a lifesaver.
As we decide whether we should use CAR T-cells in second line, that’s an individual decision at this point for the patients and their doctors.
What are the drawbacks of this newest therapy
I think we have to make sure the therapy does not cause more toxicity than the patient’s need warrants.
What I think is going to happen is we’re going to see less CHOP chemotherapy up front. We’ll probably be shifting more to the kinder, gentler bendamustine-rituximab, and maybe even in combination with ibrutinib in the first-line therapy.
The intent of that is to really clear the disease, make sure we get the highest response rate possible with the lowest toxicities, and frequency of going into the hospital with side effects like neutropenic fever. We want to avoid that.
I think that’s where the field is moving. Then the key decision, and I’m the Chief of Transplant (at Stanford) so I don’t want to malign my own therapy.
But whether or not auto transplant continues to be important in the management of mantle cell versus going right on to a targeted cellular therapy, is really the next question.
So that decision needs to be made. What we’re trying to judge is what’s the risk of the patient having cytokine release syndrome or really high-impact, really debilitating neurological toxicity.
Balance between therapy efficacy and adverse effects
A grade three neurological toxicity is when the patient is really unresponsive in the hospital, just lying there, eyes open, frequently having expressive aphasia, can’t talk, can’t find the words, can’t attend. That period of time lasts usually two to three days and patients are being treated with steroids.
Young people, like us, we may have the ability to have the reserve to get through something like that and easily bounce back.
But if you were 80 years old, having a similar treatment options, and trying to decide, I imagine the ibrutinib therapy would be the more appropriate, at least until it’s not working.
While patients are receiving those better-tolerated, maybe not curative therapies with very good efficiency or efficacy, we’re working on new therapies. We’re working on kinder, more gentler therapies, with less toxicities.
The companies we’re mentioning here are fully committed to trying to improve these treatments. Whereas maybe the drugs you took for your blood pressure and your diabetes are still the same drugs after 20 years, these drugs will not be the same drugs after five years.
We will be moving the development curve cycle into a very rapid change, because knowledge is what is going to drive the next therapy.
As we learn how to help the patients, how to improve the treatments, what happens as the universities will quickly disseminate through pharmaceutical companies to the patients’ care.
Why patients should consider clinical trials
It’s a very exciting time. It’s these small clinical trials that are able to demonstrate clinical benefit, but at the same time, we’re collecting blood samples and lymph node samples that allow us to test questions like:
- How did it work?
- How did the CAR expand?
- Did it go into the lymph node?
- Did the lymph node stop making the target?
- How do we make this treatment better?
We call that the virtuous cycle of correlative clinical trials and that’s what these large academic centers are all about. We’re trying to turn that cycle as fast as we can.
That’s a partnership with our patients, so when your patients go to a cancer center and the doctor says, “We have a clinical research trial and we have the standard of care,” it’s important to listen closely.
There are very good treatments in the upfront use of tisa-cel, axi-cel, and soon, liso-cel, so we want to be able to offer those therapies to people with 60-percent complete response rates.
But if you are having a recurrence of disease after that therapy, or that therapy is not appropriate, then it’s important to consider participating on a clinical trial in order to get access to the more promising treatments.
That’s the hardest conversation. Bring all your friends, bring your family to the doctor’s visit. You’re going to need lots of ears to be listening to why you should do this or could consider these other options.
Your doctor should be making recommendations, but you, too, have to participate as you consider the benefits and the risks.
State of current and future therapies
Multiple Myeloma
That’s my philosophical question. Let’s start with multiple myeloma, a disease we haven’t talked about but many of your patients have this.
There’ve been many advances in drug therapy since Ken Anderson in 1998, my Dana Farber mentor, said, “You know, you could take lenalidomide and dexamethasone and have a better outcome than chemo.”
That quickly changed into revlimid and that quickly changed into a whole bunch of drugs that now have really revolutionized how we think about the treatment of multiple myeloma. That’s actually changed the survival rate of patients with multiple myeloma.
You can follow in the first five decades, there was no improvement in the survival or myeloma patients. Now we can demonstrate improved overall survival every two to three years since the development of these small molecule drugs. That’s important.
There are patients with myeloma who are being cured. CAR T is coming into myeloma so that’s exciting.
We have shown that small molecule inhibitors, these phosphorylation-inhibiting drugs, these tyrosine kinase inhibitors, imatinib, ibrutinib, ruxolitinib, are having a profound effect and really better quality of treatment for the patients.
A small molecule pill instead of chemo with your hair falling out, that’s got to be good. Having a long-term disease-free survival, hopefully cure, is really advancing that field.
I think small molecule inhibitors are having a real impact on the indolent cancers.
CAR T Therapies
But the patients who have really aggressive cancers, cancers that are dividing and multiplying and doubling every two to three weeks, those small molecule inhibitors usually aren’t enough, unfortunately.
This is where harnessing the T cells and bringing CAR T cell or T cell engagers (comes in). We didn’t talk too much about that, you’re talking to a CAR T therapist so let’s say I’m a little bit of a fan, and I’ve seen these responses in patients go dancing out of the office on day 28, so I’m a big fan.
And no GVHD, no graft-versus-host disease. Pretty well-tolerated. We would like to prove the tolerability of the therapies and that’s what we’re working on.
Who’s benefitting from these therapies
I think that patients who have the blood cancers have benefited from all the advances and let’s bring it on. Let’s keep going. Let’s make this a story of only success.
What do I think is going to be needed are to apply these immune therapies into the tough cancers – the lung cancer, the breast cancer, the prostate cancer, the pancreatic cancer patients, where we haven’t small molecule inhibitors that are truly effective in this sense. Some are coming.
The checkpoint drugs we’ve seen benefit patients. Some people have really benefited from checkpoint inhibition of their own T cells, taking the brakes off their own T cells and letting their immune system fight the cancer.
That has shown benefit in many cancers. That will continue, but I think we want to figure out how to bring the response into lung cancer, into brain cancer, where we have nothing. And into all these diseases that people suffered through with the same old chemotherapies and toxicities, in ways that are not always providing long-term benefit and very few cures.
We’d like to cure more and more diseases.

What does “cured” mean
People ask me all the time, “Am I cured?” The difference between remission, where we have no measure of your cancer anymore on a scan or bone marrow or blood test, and a cure, is time.
So these exciting therapies that we’re talking about today, when I say I have a patient one year out, I hope she’s cured. But we need to wait till she comes back to my reunion in five and ten years. Until she brings her kids back.
The difference is time. And I know that your patients don’t want to wait for new developments. That’s why we have clinical trials.
That’s why testing new therapies is a partnership with patients who need treatment today and are able to be educated by their doctors and their care teams, so they understand the risks.
They’re getting the best therapies available offered to them quickly, so that they can benefit now.
I have the best job in the world, just in case you asked. It’s a bit of a vocation.
Dr. David Miklos’ Full Interview on Video
Other Oncologists
Dr. Christopher Weight, M.D.
Role: Center Director Urologic Oncology
Focus: Urological oncology, including kidney, prostate, bladder cancers
Provider: Cleveland Clinic
...
Doug Blayney, MD
Oncologist: Specializing in breast cancer | HER2, Estrogen+, Triple Negative, Lumpectomy vs. Mastectomy
Experience: 30+ years
Institution: Stanford Medical
...
Dr. Kenneth Biehl, M.D.
Role: Radiation oncologist
Focus: Specializing in radiation therapy treatment for all cancers | Brachytherapy, External Beam Radiation Treatment, IMRT
Provider: Salinas Valley Memorial Health
...
James Berenson, MD
Oncologist: Specializing in myeloma and other blood and bone disorders
Experience: 35+ years
Institution: Berenson Cancer Center
...
Jacqueline Barrientos, MD
Role: Hematologist, researcher
Focus: Chronic lymphocytic leukemia (CLL), lymphoma, 17p Deletion (Ibrutinib, Acalabrutinib, Venetoclax), IgHV mutation
Provider: Northwell Health (NYC)
...
Dr. D. Ross Camidge, M.D., Ph.D.
Role: Thoracic oncologist, Director of the Thoracic Oncology Clinical Research Programs
Focus: Lung cancer, small cell (Immunotherapy), EGFR (Osimertinib), ALK (Alectinib), ROS1 (Crizotinib), BRAF (Dabrafenib & Trametinib), NTRK
Provider: Univ. of Colorado
...
Edmund Tai, M.D.
Role: General oncologist, hematologist
Focus: Specialist in treating Chinese-speaking patients
Provider: Sutter Health (Bay Area, CA)
...
Irene Ghobrial, MD
Role: Clinical investigator and professor of hematological oncology
Focus: Multiple myeloma, Waldenström’s Macroglobulinemia, early screening, clinical trials
Provider:Dana-Farber Cancer Institute (Boston)
...
Tim Fenske, MD, MS
Role: Hematologist-Oncologist
Focus: chronic lymphocytic leukemia (CLL) & leukemia and lymphoma | CAR T, targeted therapy
Provider: Medical College of Wisconsin
...
David Miklos, MD
Date: Jan. 2021
Focus: Who benefits from CAR T, ZUMA-2 clinical trial, Stanford's CAR 22 Work
Provider: Stanford Medical
...
Kimmie Ng, MD, MPH
Role: Gastrointestinal oncologist
Focus: Young-onset colorectal cancer, microbiome
Provider: Dana-Farber Cancer Institute (Boston)
...
Farrukh Awan, MD
Role:Hematologist-oncologist, associate professor
Focus:Leukemias, Lymphomas, BMT
Institution:UT Southwestern
...
Kerry Rogers, MD
Role: Hematologist, researcher
Focus: Chronic lymphocytic leukemia (CLL), Hairy Cell Leukemia (HCL)
Institution: OSUCCC-The James
...
Nina Shah, MD
Role: Hematologist-oncologist, researcher
Focus: Multiple Myeloma
Institution: University of California, San Francisco (UCSF)
...
Rafael Fonseca, MD
Role: Interim executive director, hematologist-oncologist
Focus: Multiple myeloma, new drug development
Institution: Mayo Clinic
...
William Wierda, MD, PhD
Role: Hematologist, Med. Dir., Dept of Leukemia
Focus: Chronic lymphocytic leukemia (CLL), other leukemias
Provider: MD Anderson
...
Latest on CLL Treatment (2022)
Featuring: Nicole Lamanna, MD; William Wierda, MD, Ph.D
Hosted by: Michele Nadeem-Baker
Topics: Pirtobrutinib, new oral combinations, venetoclax updates, CAR T
...
David Miklos, MD, Ph.D
Role: Hematologist, researcher
Focus: How MCL treatments have improved, importance of clinical trials
Provider: Stanford Medical Center
...
David Miklos, MD, Ph.D
Role: Hematologist, researcher
Focus: Role of allogeneic BMT, response to graft versus host disease (GVHD)
Provider: Stanford Medical Center
...
CAR T Cell Therapy in Myeloma
Dr. Fonseca shares his insights on emerging T-cell therapies for multiple myeloma, describing the role T-cells play in our bodies and then focusing on chimeric antigen receptor (CAR) T-cell therapy and bispecific T-cell engagers.
...
Joseph Mikhael, MD
Role: Dir. Myeloma Research, CMO at International Myeloma Foundation (IMF)
Focus: Multiple myeloma
Provider: TGen/City of Hope
...
Ruben Mesa, MD
Role: Executive Director, Mays Cancer Center; Prof. of Medicine
Focus: Myeloproliferative neoplasms (MPN)
Institution: UT Health San Antonio MD Anderson
...
Srdan Verstovsek, MD, PhD
Role: Director, Clinical Research Center for MPNs at MD Anderson; Section Chief, MPNs; Prof., Dept. of Leukemia
Focus: Myeloproliferative neoplasms (MPN)
Institution: MD Anderson
...
Saad Z. Usmani, MD
Dr. Saad Usmani, Chief of Myeloma Service at Memorial Sloan Kettering, talks about CAR T-cell therapy, bispecific antibodies, novel therapies and combination therapies.
...
Vincent Rajkumar, MD
Dr. Vincent Rajkumar, a hematologist oncologist at the Mayo Clinic, talks about drug pricing and the impact of high prescription drug costs on patients and families.
...
The Doctor Talk w/ Dr. Gasparetto & Dr. Richter
Role: Dr. Cristina Gasparetto (Duke) and Dr. Joshua Richter Mount Sinai discuss latest relapsed refractory multiple myeloma treatments
...
Dr. Samuel Washington, MD, MAS
Role: Assistant Professor of Urology, UCSF
Focus: Treatment disparities in bladder cancer treatment
Provider: University of California San Francisco
...
Multiple Myeloma in 2023
Long-time myeloma patient and advocate, Jack Aiello, leads the conversation with Dr. Joshua Richter, Multiple Myeloma Director for Blavatnik Family Chelsea Medical Center at Mount Sinai and Dr. Muhamed Baljević, Plasma Cell Disorders Research Director for Vanderbilt-Ingram Cancer Center.
...
Matthew Matasar, MD, MS
Dr. Matthew Matasar, chief of blood disorders at the Rutgers Cancer Institute of New Jersey and RWJBarnabas Health, sat down with Dr. Samantha Spiegel, a Hodgkin’s lymphoma patient, to discuss some of the most exciting news coming out of ASH 2022.
...
DLBCL in 2023
The Patient Story founder and DLBCL advocate Stephanie Chuang leads the conversation with Dr. Josh Brody, who leads the Lymphoma Immunotherapy Program at Mount Sinai’s Tisch Cancer Institute, and Dr. Lorenzo Falchi, an oncologist at Memorial Sloan Kettering Cancer Center.
...
SABCS 2022 Highlights
Top breast cancer doctors Dr. Paolo Tarantino with Dana-Farber Cancer Institute and Dr. Lola Fayanju with Penn Medicine discuss the big highlights from this year’s San Antonio Breast Cancer Symposium.
...
Relapsed/Refractory Multiple Myeloma Highlights from ASH 2022
Multiple myeloma specialists Dr. Ajai Chari with Mount Sinai in New York and Dr. Sandy Wong with the University of California San Francisco discuss the big buzz at this year’s ASH: bispecific antibodies.
...
Myelofibrosis Highlights from ASH 2022
Dr. Serge Verstovsek and Dr. Naveen Pemmaraju discuss cutting-edge treatments and therapies, and combination therapy as a focus in treating myelofibrosis.
...
Newly Diagnosed Multiple Myeloma Highlights from ASH 2022
Dr. Caitlin Costello and Dr. Sagar Lonial discuss treatments for newly diagnosed multiple myeloma patients.
...
High-Risk Smoldering Multiple Myeloma Highlights from ASH 2022
Patient advocate Jack Aiello and hematologist Dr. Shaji Kumar discuss what high-risk smoldering patients can do to delay or possibly avoid progression to active myeloma.
...
DLBCL: The Latest in Treatment and Research
Discover the latest DLBCL treatments from two top lymphoma doctors and a diffuse large b-cell lymphoma survivor who is also a doctor.
...
Chadi Nabhan, MD, MBA
Dr. Chadi Nabhan shares how he got involved in the Monsanto trials, what he learned from the, and why he decided to write a book about the whole experience.
...
CLL Highlights from ASH 2022
Patient advocate Andrew Schorr and hematologist Dr. Nitin Jain discuss the latest treatment and developments in CLL coming out of ASH 2022.
...
Research on Black Myeloma Patients, Access & Disparities
Patient advocate Valarie Traynham and Dr. Shakira Grant discuss the barriers many Black patients face, how it impacts their care, and what can be done to help improve their outcomes.
...
Testicular Cancer: What Patients Need to Know
Medical oncologist Alok Tewari, MD, PhD, who specializes in cancers arising from the genitourinary tract, discusses what patients need to know about testicular cancer.
...
Lynch Syndrome: What Patients Need to Know
Medical oncologist Michael Hall, MD, MS, discusses Lynch syndrome, what cancers patients would be more at risk for, and who should get tested.
...
The Role of Bispecific Antibodies in the Treatment of Multiple Myeloma
Hematologist Alfred Garfall, MD, MS, from Penn Medicine discusses with multiple myeloma patient advocate Jack Aiello the advancement of immunotherapy for multiple myeloma, the difference between CAR T-cell therapy & bispecific antibodies, and the role of bispecifics in the myeloma toolkit of immunotherapies.
...
How to Build a Strong CLL Team
Nicole Lamanna, MD, from Columbia University Medical Center, Spencer Bachow, MD, from Boca Raton Regional Hospital, and CLL patient Lisa P. discuss the importance of building a strong support system and collaborating effectively with multiple doctors.
...
The Latest in Lung Cancer Treatments: Is a Clinical Trial Right for Me?
Leading experts Estelamari Rodriguez, MD, MPH, from the University of Miami Sylvester Comprehensive Cancer Center, Jason Porter, MD, from West Cancer Center & Research Institute, and Terri Conneran, founder of KRAS Kickers, discuss the latest in lung cancer treatments and ongoing clinical trials.
...
The Latest in Multiple Myeloma Treatments: What Clinical Trials are Available to Me?
Patient advocate Cindy Chmielewski, experts Dr. Carl Ola Landgren and Dr. Caitlin Costello, together with clinical trial nurse Christen Hawthorne uncover groundbreaking insights on the latest multiple myeloma treatments and clinical trials.
...
Clinical Trials and You: How to Navigate Treatment?
Patient advocate Ruth Fein Revell, experts Dr. Angela Fleischman and Dr. Ruben Mesa, together with clinical trial nurse Melissa Melendez delve into the cutting-edge realm of myelofibrosis clinical trials.
...
Let’s Talk CLL: Patients & Doctors Discuss the Latest LIVE
Patients, care partners, and a panel of CLL experts including Dr. William Wierda, Dr. Nicole Lamanna, Dr. Adam Kittai, and Jackie Broadway-Duren share the latest in CLL research, clinical trials, treatments, and comprehensive care strategies.
...
The Latest in Multiple Myeloma: Understanding Promising Treatment Options
Patient advocates Cindy Chmielewski and Jack Aiello, and experts Dr. Rafael Fonseca and Dr. Susan Bal discuss promising multiple myeloma treatment options.
...
The Latest in Hodgkin Lymphoma: Treatment Options in 2024
Dr. Matthew Matasar, chief of blood disorders at the Rutgers Cancer Institute of New Jersey and RWJBarnabas Health, discusses some of the most exciting news coming out of ASH 2023.
...
Optimizing Quality of Life: Reducing Toxicity in Hodgkin Lymphoma Care
Dr. Andy Evens from Rutgers Cancer Institute discusses how to reduce the toxicity of Hodgkin’s lymphoma treatments so patients can live their best lives after cancer.
...