Leaving the Hospital: Emotions & Support

A hospital stay can mean different things to different people. It can be anxiety-ridden, or it can make a patient feel safer to know they’ll be surrounded by doctors. It can make some patients feel trapped. For some, going home is a relief; for others, leaving can be scary. It’s important to remember that your medical team knows best, and you have the support you need.
Read on for answers from real cancer patients about how can you navigate the feelings that come along with hospital stays.
For some patients, the hospital can feel like a jail sentence. It’s important to not lose hope.
Being away from home for prolonged periods of time while being hooked up to machines and feeling sick can take a toll on a person’s mental health.

Stage 4B cervical cancer survivor, Brittany Wagner says:
I thought, ‘I might not ever leave the hospital at this point. If there’s nothing they can do, this might be where I start just getting sicker and sicker.’

Jude Abella went through stage 3 multiple myeloma and is in remission currently only needing follow-up blood work. She stayed in a rehab facility and says she felt alone.
Finally, I said, ‘I have to get out of here. I want to leave.’
My mom said, ‘You can leave, but you have to do the things they’re wanting you to do first.’”
How can you help if someone you know is having these thoughts and feelings? Jude says visits helped her through the toughest times.
- Visit
- Bring familiar items from home (clothes, blankets, books, etc.) with the doctor’s permission
- Call or text frequently
- Bring an outside favorite food if the doctor approves
- Help them get up and walking
- Encourage them and remind them that their hospital stay won’t last forever
On the other hand, leaving the hospital can cause anxiety for some patients.

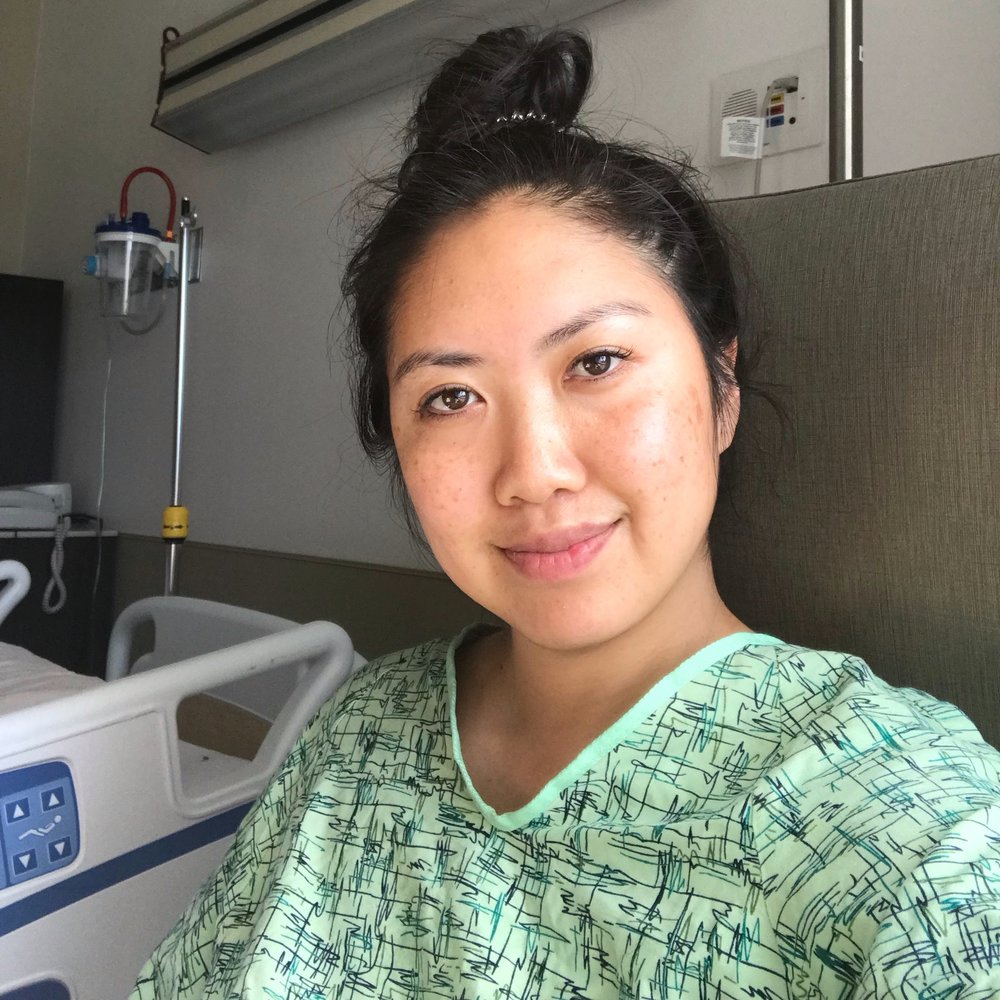
Rachel Rhee is a renal cell carcinoma survivor. She went through a partial nephrectomy and overcame her cancer. When asked how long she stayed in the hospital after surgery, she responded:
Two nights and three days. I wanted to stay a third night, but the whole team said it would be better if I went home. I think it was just the fear I had creeping up again. I wanted to be around medical professionals because the what-ifs were kind of paralyzing for a little bit.
It can be scary to leave the medical team who has taken care of you. It can scary to think about the what-ifs.
It can be hard to imagine that you’ll be able to make it on your own after having around-the-clock care.
These are all normal feelings.
Just ask Casey Head. She stayed more than 100 days in the hospital including a stay for a stroke after chemotherapy complications.
I started having panic attacks about leaving the hospital. I was like, ‘Oh my god, my team’s not going to be here. What if something happens?’
Everything starts going through your head and you start freaking out. They were like, ‘You have to leave. It’s time to go home,’ but I just kept asking if they were sure. My mind kept going to worst case scenarios.
While going home can cause anxiety, it’s important to remember that your medical team wouldn’t send you home if they didn’t think it was safe and in your best interest.
Rachel was admittedly anxious about leaving, but she says that now she’s had some separation from the experience, she knows her doctors were doing what was in her best interest.
The doctors and everyone wanted to get me out of there. Not because they didn’t want to take care of me, but they said that my recovery would go a lot quicker and smoother if I did it at home.
In hindsight, I totally agree, but at the time I thought it was too fast. I thought, ‘what if something goes wrong?’ I was also just very afraid of the pain. At the hospital, you just ring for a nurse, and they’ll take care of you immediately if you’re in a lot of pain. I wouldn’t really have that at home, so I was nervous about that.

You would not be sent home if your medical team didn’t think you could handle it.
Keep in mind there is usually there is some sort of stipulation depending upon your diagnosis and treatment – i.e. you have to be able to walk up the stairs on your own, go to the bathroom on your own, etc.
Kevin Reamey is a kidney cancer survivor who believes in relying on your family, doctors and caregivers to get you through. When asked about his release from the hospital he says,
You can’t leave the hospital until you can pee, and you have to pee on your own or they won’t let you out.
Casey used something similar as her motivation for getting out of the hospital when she decided she was ready to go home:
My husband knew that if I couldn’t get well enough to walk and get up stairs, they weren’t going to send me home. We came up with a plan for me to do laps. The first time I did it, it took me five minutes to go one lap around the nurses station.
So, that was what started me on setting daily goals and getting out of my own head. That really changed my mindset.
It’s important to remember that there is so much support for you even after you go home.
This support can come from anywhere. It can come from your family, friends, spouse, pet, medical team, plant – anywhere. It can come right from TPS. Remember: you will have all the support you need to get better.

Bernadette Lucas-Burch is a nurse navigator. She is generally there when a patient gets their diagnosis and follows them through their treatment helping them navigate all the options and emotions. She says,
The navigator can assist at least reminding the patient that there will be ongoing support when they’re discharged.
We usually introduce ourselves and especially follow up when they’re discharged home because we want to ensure that they know there’s ongoing support when they leave the hospital.

Barbara Kivowitz is a clinical social worker, healthcare innovation consultant, and author. She wrote a book about the impact of chronic illness on a spousal relationship. Her insight on how a spouse can support a patient after leaving the hospital is:
When they go home, it’s so easy for illness – who has a very loud voice and a demanding personality – to take over and to make the decisions for the partners.
It’s easy for the patient and caregiver to abdicate their authority and potential to the demands of the illness. What mitigates that is the power of their relationship.
It’s hard for either one to stand alone and tell illness to back off, but the two of them together digging into what really matters is a wellspring that can get people through.
Arielle Rosen went through Primary Mediastinal B-Cell Lymphoma. She says that through her non-Hodgkin lymphoma, she realized she got support from anywhere and everywhere she could.
During her stay in the hospital, she stimulated her brain with TV and found comfort in the characters. After leaving the hospital, she relied on a little bit of everyone.

I don’t think that you can ask to get everything, all your needs met from one person. I don’t think that’s true in life in general.
So, I could get certain emotional needs met by my wife, I could get certain emotional needs met by what ended up being some of my oldest friends and some of my newest friends.
It can be so many different things but for me the point is that I had needs that needed to be met.
I had emotional needs, I had physical needs, logistical needs, I needed people to drive me places to go to the doctor, and I had to get those met by others. By television. And by myself.
No matter what you’re feeling about leaving the hospital, just breathe. Whatever you’re feeling is normal. Whether you’re scared, nervous, indifferent or any other emotion – someone else has been there before.


One reply on “Leaving the Hospital: Emotions and Support”
Very good information keep it up