Caregiver Stories
Spouse of Non-Hodgkin Lymphoma Patient
Refractory, CAR T-Cell Therapy

The analogy I always use is when you’re on a plane and the flight attendant tells you to put the oxygen mask on yourself before your child.
It’s because if you can’t take care of yourself, you can’t take are of anyone else.”
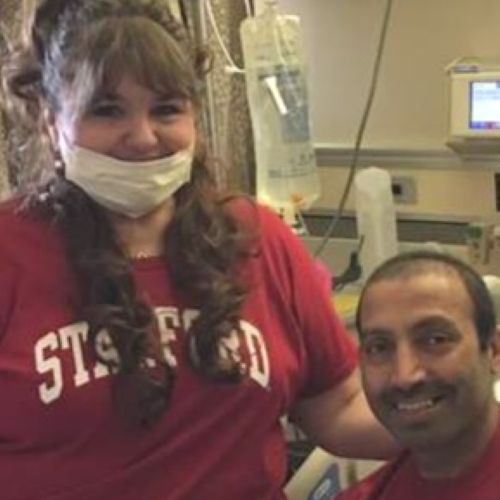
Nicole Bhat
Nicole was with her husband, Shahzad, every step of the way through multiple misdiagnoses, travel for treatment, and even helped save his life by taking research into her own hands.
She admits it may not be the easiest life, but says you can still live a very full life. Most of all, she wants to remind caregivers to remember to take care of themselves first.
- Name: Nicole Bhat
- Relationship to Patient: Wife
- Patient Diagnosis:
- Non-Hodgkin Lymphoma
- Subtype misdiagnosis: Mantle Cell Blastoid
- Subtype final diagnosis: Diffuse Large B-Cell
- Non-Hodgkin Lymphoma
- Treatment(s):
- R&B: Rituximab, Bendamustine
- R-ICE: Rituximab, Ifosfamide, Carboplatin, Etoposide Phosphate
- R-EPOCH: Rituximab, Etoposide Phosphate, Prednisone, Vincristine Sulfate (Oncovin), Cyclophosphamide, Doxorubicin Hydrochloride (Hydroxydaunorubicin)
- CAR T: Chimeric Antigen Receptor T-Cell Therapy
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Being a Cancer Caregiver
How did you handle the diagnosis
When I first heard the diagnosis I had never head the word “lymphoma” before, so I had a learning curve.
I was actually doing it over the phone, long distance. I was in another state (working) and there were times I’d be on the phone during visits to speak with the doctor directly, but that became very difficult and so I came back to be with him full-time.
I will be honest. There were times I had anxiety attacks. The information was just overwhelming, even for me.
What was helpful during treatment
- What worked really well for me is to keep a notebook or datebook, every time you go to an appointment, you write down who you saw, what the lab works were, what medication were given or stopped, especially with chemo because all that information becomes necessary down the line and there’s no way anybody can remember it. It’s just easier than reading through charts!
- I’m a big fan of resources and I don’t put all my eggs in one basket. I think there are phenomenal organizations out there that are resources and then they can make referrals to others, whether it’s moral support and communities where you can engage with other patients with your same diagnosis, same staging, financial help, or research and clinical trials, there really are a lot of resources.
There’s even patient advocates, professional ones, that will help you and give you links and resources to turn to so absolutely rely on them, depend on them, use them, that’s what they’re there for and they will be most helpful because sometimes the family and friends aren’t able to. - You need to be on your own best advocate, you can’t rely on others to hand you information. You need to go out and look for it yourself, but again, there are so many out there and free resources to help you.
What support did your husband need most
I told everybody, “Here’s my phone number. If you want to speak to him, you call me, he needs to focus on being a patient, healing and working all his way through chemo so let me answer the questions, let me navigate all that stuff.”
So that took it off of him.

Learning everything about the treatment process
I became almost obsessed with it. I wanted to learn everything I could, all the options, everything out there, what to expect emotionally, what to expect physically, what to expect financially, what to expect from others or not expect from others.
As far as the physical aspects, it was just back-to-status quo, cooking and cleaning like normal. The diet’s a little more detail-oriented.
To be honest, that’s just a part of my personality so it came very [naturally] and easy. I actually enjoyed it because I’m learning. Everyday that you learn is a great day.
When I see a problem, I naturally just try to figure out how it works so I can figure out how to fix it. I realize that’s not something in everybody’s DNA, but I think once you understand the rules and the process, you can figure out how to navigate through them. There’s really no simple answer.
Caring for Yourself & Your Family
How did you take care of yourself
It’s important that caregivers take time to take care of themselves and I was pretty good, whether it was a hot bath or the gym or a trip to the beach to reset, even a glass of wine with a girlfriend, whatever it is, a concert.
I didn’t limit myself from going out and living a normal life when I could. That was really how I let off my steam.
What was your emotional outlet
When I got overwhelmed, I let myself cry. I just got it all out and then a good night’s sleep. I’d wake up the next morning, ready to take on the world again.
I allowed myself to cry but not in front of him. I always stayed strong in front of him and kept everything positive even when we had to tell our son he had three months to live.
I didn’t want to tell [our son] until I knew CAR T-cell therapy was an option so that I delivered bad news but I could come back with something positive.
Did you tell your son about the cancer
Summary: In the end, yes, so he could be involved and not create his own fears.
With our son, I did keep it from him for a few months because I didn’t want him distracted from school. So he came in for, I don’t remember, Spring Break, and when we got to the airport I said, “Okay, I need to tell you something but I also need you to know it’s going to be okay.”
I told him and he’s like, ‘I kind of already knew.’

He sensed it somehow and later when we got the three-month notice, again I kept it from him and he got very angry with me for that. He told me he was old enough, cared enough, and didn’t want to be left out.
We involved him from the beginning, he saw his dad in chemo, he was able to ask the oncologist any questions he wanted, he went with us to the lymphoma conference so he could learn, and I think he felt involved in the process. So he never felt isolated or scared.
Even the young ones, they need to be aware that their parent is ill so they can be more sensitive, and not expect the same physical reactions and energy levels. If you don’t tell them, they create their own fears and I don’t think it’s a great idea.
Each parent needs to know their child and what they’re able to comprehend and feel. But in my opinion it’s always best to be honest, open, and upfront because the moment you lie to them, they’re losing trust in you.
Advice to other caregivers
Do your research. Learn as much as you can and question everything because people do make mistakes, even doctors and nurses. I would definitely suggest a second opinion to be 100-percent sure.
Don’t look at statistics on the internet. Stay away from that stuff because each patient is different, each subtype is different, each experience is so different, you can’t compare yourself to a graph or statistics. It just doesn’t add up.
Do things that make you happy because yes, you’re in this. I always refer to this as “we” because we’re in this together even though we have different participants, but your own sanity and health are equally as important. The caregivers are not the ones with the cancer so they don’t have to treat themselves like they are.
Advice to people who want to help the patient and caregiver
My advice to people who want to reach out to caregivers is [say], “Let me know if there’s something I can do for you.” Because myself, I’m never going to take you up on that. Be specific.
“Hey, can I cook you guys a meal?”
“Hey, do you need help with rides to the doctor?”
“Hey, do you need me to take your kid or do the laundry?”
Something specific because when you leave it general it sounds disingenuous from our perspective.
Story Summary
There was never a moment when Shahzad had to navigate his cancer diagnosis alone. His wife, Nicole, made sure of that.
It wasn’t easy from the beginning. The path to diagnosis for Shahzad took over a year. He had extreme fatigue and so much pain in his feet that he could not walk.
After being sent home from urgent care multiple times, a couple biopsies, an an attempt at a stem cell transplant, he was diagnosed with a rare, aggressive form of Non-Hodgkin Lymphoma: Mantle Cell Blastoid. He finished chemotherapy on Halloween in 2016.
Doctors congratulated Shahzad – he was in remission.
But three weeks later, right before Thanksgiving, he, his wife, Nicole, and son, Adam, got the shock that the cancer was back. Not only was it Stage 4, it was more widespread. He underwent RICE, a much more harsh chemotherapy regimen than the “R&B” one he had undergone before.
Then came the real shock: They learned that he did not actually have Mantle Cell Blastoid. He actually had Diffuse Large B-Cell Lymphoma (DLBCL) all along. After more chemo, a scan showed that the cancer was still there.
Nicole remembers exactly what came next.
The doctor called and said, ‘I’m sorry your husband has relapsed, he’s refractory, he’s no longer responding to chemo, there’s nothing we can do.

Based on how quickly the cancer had spread before, doctors estimated Shahzad would have three months to live.
Thankfully, Nicole had been researching all treatment options and paying constant attention to new developments.
Just 24 hours before hearing she and her son were going to lose the rock in their life, the FDA had approved a commercial drug, Yescarta, for Diffuse Large B-Cell Lymphoma.
Nicole went to work. What she did next helped to save her husband’s life. The Patient Story features what happened next with their experience with CAR T-cell therapy.

Inspired by Nicole's story?
Share your story, too!
Caregiver Stories
“If you volunteer, just make sure you can be there. Be whatever they need you to be, but don’t force yourself into a situation because that can be really frustrating.”...
Dr. Heather Paulson
Naturopathic Doctor: Part of integrative cancer care, help with complementary therapies
Experience: 15 years
Treatment Center: Integrative Clinic
...
“If you can't take care of yourself, you can't take are of anyone else.”...
“A critical ingredient we need throughout our lives in all circumstances is hope. Hope can exist and persist even when a cure is not possible. You can attach hope to anything.”...
Lisa Matthews, Spouse to Prostate Cancer Patient
"It’s just that tough. It’s scary and difficult, and you need to give each other some space, but also give each other that support and love."
...
"You need to take care of yourself as well as you take care of the person that you love so much who's going through it."...
Joe T., Spouse of ALL Cancer Patient
"You've got to take care of yourself to take care of your patient. You've got to. You're not infinite. You're not just a well of giving."...
Kelsey K., Spouse of ALL Cancer Patient
"Caregivers need caregivers. It never ends. We all needed each other."...
Marsha Calloway-Campbell, Spouse of Myeloma Patient
"Once you are taking care of someone with myeloma, be their advocate because it’s a journey. It can be challenging at times so they need somebody."...
Financial Toxicity of Cancer Treatment
Dr. Fumiko Chino opens up about her late husband’s diagnosis and the financial toll it had on them.
...
Carley G., Spouse of Hodgkin’s Lymphoma Patient
“If your glass is empty, you can’t fill anyone else’s and that’s something that I wish I would have done more of.”...