Kara’s Stage 1B Synovial Sarcoma Story
Kara shares her stage 1B sarcoma story, synovial sarcoma subtype, and going through treatment: chemotherapy, surgery, and radiation therapy.
In her story, Kara also highlights how she navigated life after the cancer diagnosis, including hair loss, how she was able to ask for help, and managing life as an AYA (adolescent young adult) cancer patient. Thanks for sharing your story, Kara!

- Name: Kara L.
- Diagnosis (DX):
- Synovial sarcoma
- Type of soft tissue sarcoma
- Age at DX: 24
- Staging: 1B
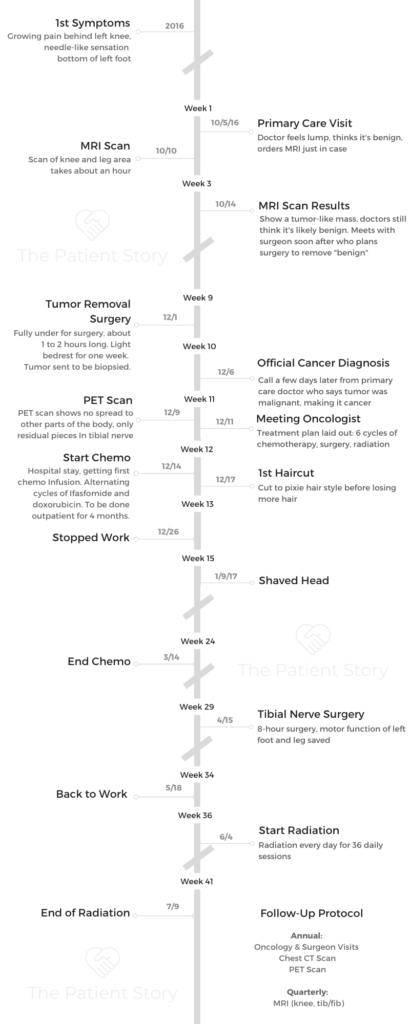
- 1st Symptoms: Pain behind left knee, needle-like sensations on left foot
- Treatment:
- Surgery to remove misdiagnosis of benign tumor
- Chemotherapy
- Ifosfamide & doxorubicin
- 3 cycles each, ended up cutting one short because of neutropenia
- Outpatient (attached to chemo pump)
- Surgery: tibial nerve removal
- Radiation
- 36 sessions (36 days)
I’m not grateful for my cancer by any means, but I’m grateful for the transcendence that came about from my trauma. That post-traumatic growth is not out of reach for you if you’re a cancer patient and going through this journey. Post-traumatic growth can happen.
Kara L.

- Video Interview: Kara's Story
- First Symptoms and Steps
- What were the first symptoms?
- How bad was the pain on scale from 1 to 10?
- What got you to go to the doctor’s
- What happened at the first doctor appointment?
- Describe the MRI
- Did you experience “scanxiety” waiting for results?
- How long did it take to get MRI results?
- Cancer was not on your mind
- What were the next steps?
- 1st Surgery
- Cancer Diagnosis
- Treatment Decisions
- Chemotherapy
- Hair Loss
- Tibial Nerve Surgery
- Radiation Therapy
- Reflections
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Video Interview: Kara’s Story

First Symptoms and Steps
What were the first symptoms?
I had a needle-like sensation on the bottom of my left foot, so it was like my foot was falling asleep frequently. I couldn’t stretch my quad because I felt like there was this pain behind my knee.
I wasn’t able to pinpoint exactly where it was coming from. It was recurring for about a year or so. I went to multiple physical therapists, and nobody could exactly pinpoint what I was experiencing.
They said it could be a pinched nerve, you could just be sitting down too much, you might want to look into a standing desk, but nothing concrete or definitive.
How bad was the pain on scale from 1 to 10?
It was really around a 4 or a 5. I would say the most pain was when I tried to stretch my quad. After spin class — I did spin very often, that was one of the main reasons I was able to pinpoint that I couldn’t stretch my quad properly — that was when it was most painful. Other than that, it was really more of an annoyance than a pain.
What got you to go to the doctor’s
I remember really vividly sitting on my bed, stretching after a spin class, and I was putting my hands under both of my knees. I squeezed or pressed behind my left knee. A shooting pain went down my leg from my kneecap down to the middle of the bottom of my left foot.
I was like, “Oh, there’s something there.” I noticed there was a tumor or something there. I was like, “It’s probably just a cyst,” but that definitely motivated me to get a doctor’s appointment penciled in swiftly.
What happened at the first doctor appointment?
It was a physical that I already had scheduled but moved up. She said it was most likely a benign tumor or a cyst, like I thought, but let’s just get an MRI to triple-check. So I moved forward with the scan.
Describe the MRI
An MRI is sometimes 30 minutes, up to an hour or more, depending on the body part, but you essentially sit in this space-like machine. It makes a ton of noise. You’re either wearing a pair of headphones and listening to music or have earplugs in.
That was my first MRI that I ever had. I remember being like, “What is this thing?” I wasn’t stressed; I was fairly calm actually, but it’s more annoying. You can’t move for about an hour. For me, the most stressful part of the scan is waiting afterwards, not necessarily during it.
Did you experience “scanxiety” waiting for results?
I don’t remember any scanxiety at that point because I was working so much and was moving at such a fast pace that I didn’t really think anything of it. I think a lot of cancer patients can relate to this when they were diagnosed. Everyone says they’re Superman or Superwoman, invincible.
I didn’t have any scanxiety after that first scan, but today the scanxiety is most definitely real and there. I don’t think it really ever goes away. You just learn how to manage it a little bit better.
For me, I hone in on those rituals and routines that are spiritual and wellness oriented. They helped me stay grounded, calm, and composed.
But I vividly remember when I got the results back, where I was and how that felt, when I saw that it was a tumor. It came back as benign, but just the word “tumor” freaked me out. I left work instantly.

How long did it take to get MRI results?
It took about one week.
Cancer was not on your mind
I thought it was a benign cyst, for sure, because all of my doctors were pretty nonchalant about it. Nobody was really that concerned, so I wasn’t that concerned. Cancer wasn’t at the forefront of my mind at all.
The word ‘tumor’ when I saw the results, even though it was benign, freaked me out.
I remember calling the nurse at my primary care and getting her verbal confirmation that she could send me the results. She sent me my MRI results via email.
I read them and saw the word “tumor.” Although next to the word “benign,” still freaked out. I had that paralyzing moment where I saw double vision. I panicked and left work.
What were the next steps?
I ended up calling my doctor, and she calmed me down [and] introduced me to a surgeon to take next steps. I remember going home, and her nonchalant nature and attitude made me feel more at ease.
At that point, I wouldn’t say I was that tapped into my own sense of self or listening to my gut. In retrospect, I feel like I knew something was wrong. I was just masking my fear and leaning on other people’s opinions and words a little too much.
1st Surgery
Misdiagnosis of benign tumor
The first surgeon who I met with was the one I moved forward with. He was fairly arrogant and honestly overly confident. He even told me I could keep the tumor in my leg, that it wasn’t that big of a deal, a benign tumor.
I remember second-guessing his energy and my relationship with him, my conversation with him, [and] going back to my general physician and being like, “Are you sure you recommend him? Is he the best of the best?”
He was an orthopedic surgeon, and she responded, “Yes, he comes highly recommended. I personally haven’t used him for surgery, but he comes highly recommended from other patients.”
That’s when I really should have listened to my gut because I did move forward with that surgeon, thinking it was a benign tumor. Low and behold, we found out it was malignant after the surgery.

How were you feeling going into surgery?
Overall, again, listening to other people’s confidence that it was benign put me at ease. I’m fairly fearless and trusting, sometimes to a fault, and I would say in that surgery I was more in the New Yorker attitude, where I just wanted to get it done.
Get the tumor out so I could get back to my day to day, get back to my spin classes and my working out, and [get] my life back on track. I was looking to check the box and move forward.
Describe the tumor removal surgery
My surgery was just to remove the tumor. The tumor was intertwined within my tibial nerve on my left side. That is a nerve that gives you motor function, essentially, and sensation on your left leg, bottom of your left foot, and calf.
We were going in and removing that tumor. I was fully under. It was an hour or two; it wasn’t anything too extensive. I was on bedrest for maybe a week, but I could really put pressure on it and kind of start walking on it right away. I had a three-inch scar behind my left knee, and that is different to where I’m at today.
Getting a second opinion
In retrospect, I would have done things differently. I would have gotten multiple surgeon opinions and talked to multiple people, maybe do a biopsy testing before.
But you can’t change the past. It was always the plan to biopsy it at some point after the surgery.
How did the benign diagnosis affect your overall treatment?
I could get emotional talking about it in all honesty. It could’ve changed the entire trajectory of my treatment. My first surgery, they ended up leaving pieces of the tumor in my leg, thinking it was benign.
I can’t get into the details. I haven’t asked my doctors that much, because you can’t change the past. You don’t want to drive yourself insane. But my treatment most likely would have been less intensive if we would have taken a more thorough approach when it comes to pre-surgery.
Advocating for yourself as the patient
Be your own advocate. Trust your gut. Get multiple opinions.
There’s nothing wrong with more information that can help bring more clarity to your own opinion and perspective. There’s nothing wrong with talking with more people, in my opinion.
You do have to take those opinions with a grain of salt at times because your fear can get in the way. Yu can spiral, so just take your opinions and get quiet. Process them. Unpack them to form your own opinions and perspective.
»MORE: How to be a self-advocate as a patient
Cancer Diagnosis
Describe the moment you got the diagnosis
The day I was diagnosed, I remember so vividly I was sitting in my bed, my leg propped up on a pillow, and I was working remotely. I was blogging, writing. I was a partnerships editor at Hearst at the time, and I was writing for 27 different publications.
I was back at it in that New Yorker mentality.
I remember I was having routine nurse follow-ups. Nurses would call you a couple times a day to check in how you were feeling, how you were doing, what your pain was 1 to 10.
My phone rang, and I picked up, completely still in the work zone, not paying attention and not realizing it wasn’t just a nurse calling me, but it was my general physician.
I remember stopping what I was doing when she said the words, ‘Are you sitting down?’
I can still get so emotional. After that, speaking of remembering it vividly, I don’t remember anything after that. I completely blacked out. She said the word “malignant,” but I was like, “I don’t even know what that means.”
When you’re not a cancer patient or it hasn’t touched you in some shape or form, you don’t really understand this medical lexicon, this vernacular.
I remember her saying “malignant” and being like, “What is that?” She said the word “cancer.” Tears streamed down my face, and my body was red hot. I was convulsing, almost dry-heaving. It was an out-of-body experience. I really felt I was in a complete nightmare. It wasn’t real life.
After that I cried, then went through the motions and called my loved ones right away. I didn’t even take a pause.
»MORE: Patients share how they processed a cancer diagnosis
Breaking the news to loved ones
I called my mom and dad first. They were driving. My family lives in Colorado. They were driving from the mountains. I remember not being able to get words out.
Parents know you so well. My dad asked, “Is this about the surgery?”
I said, “Yes, I have cancer.”
I completely blacked out. I get so emotional even thinking about it, because your parents feel your pain so much more than you do. I remember calling my boyfriend as well and seeing him later that evening.
»MORE: Breaking the news of a diagnosis to loved ones

Advice on how to share the news of the diagnosis
There’s no right way to tell your loved ones. No one knows how to talk about cancer or talk about a diagnosis. It’s more that you get it out.
In the past, I compartmentalized everything and held everything so close. Releasing that in some way is so important.
Having that transparent channel of communication, not even just telling your loved ones that you’re diagnosed, but throughout your entire treatment, maintaining that transparent communication.
For me, with other loved ones and friends, I felt obligated to tell everyone. I think that’s something that I would be mindful of moving forward.
This is your journey, and this is your time to heal and be selfish. It’s not your duty to convey to the world or to every single friend that you were in contact with that you were diagnosed.
I think that’s something I put a lot of pressure on myself to do that was unnecessary.
When it comes to talking to my friends, I just gathered everyone in one place. Tried to condense the calls as much as I could, to make it easier on myself. Instead of doing 100 calls, you could do 10.
I had a list of people, and I was like, “Why am I doing this to myself?” It felt like a lot of work that was unnecessary in retrospect.
»MORE: Breaking the news of a diagnosis to loved ones
Treatment Decisions
How did you pick an oncologist?
Coincidentally, I had moved a couple blocks away from NYU Hospital, which was home to the oncologist that invented [one treatment] for my particular cancer, sarcoma.
So I was very lucky; it was very kismet. I was not even moved into my apartment in my room yet. I was, but I still had boxes everywhere. It was very new.
I was recommended to that doctor, and I met with him and then started to trust my gut now that it was a more serious circumstance. Given he invented [a treatment] for my cancer, I moved forward with NYU.
I still talked to other doctors even during and after my chemo. Even after I started, I talked to second, third, and fourth opinions regularly to ensure I was on track. Given the cancer was rare soft-tissue cancer, it was a circumstance where we had to move very quickly.
PET scan
I had my PET scan before I met with the oncologist. The PET scan, you get contrast (dye). You drink an awful drink, like pineapple milk. It’s gross. It lights up if there’s any malignant activity anywhere in your body.
You sit for a long period of time, but it’s a full-body scan. You can’t drink coffee or eat sugar for I think 24 hours. I do one once a year now, so it’s not as frequent as my MRIs.
PET scan results
My PET scan thankfully came back completely clean, other than the area in my left leg where we knew the cancer was, because the tumor was out of my leg at that point, but there were still pieces left on the nerve.
How did your oncologist characterize the treatment plan?
He took me through the trajectory of my treatment and that we needed to move quickly because this was a rare cancer. I had both of my parents there, who flew out right away. They were with me through my PET scan. I had my now ex-boyfriend there with me as well.
That’s something I would really recommend, bringing support to not only that first appointment, but to a lot of appointments because sometimes it’s really emotional, so you don’t remember or know what’s going on in those appointments.
To have a second or third person there who could be writing notes and asking questions on your behalf was really important and integral in my treatment.
Especially that first appointment, we were so confused. We were like, “Where do I go when I go to the hospital? Do I meet downstairs?”
There were so many different questions that we didn’t ask. We just didn’t know what to expect. So even having that second or third pair of ears was really important to me and helpful.
Chemotherapy
Getting a PICC line
I liked the PICC line, and I have small scars from it. It ended up working really well for me. I went on Amazon and got all different kinds of covers and shower bags that would help keep it dry.
It wasn’t painful at all. I remember being so scared to get that PICC in, and it was nothing. At the end of the day, it was more emotional than physical pain.
»MORE: Read more PICC line experiences
Describe the chemo regimen
I started a week later, so it was very quick. I was still trying to juggle my job at the same time. I didn’t know how the chemo was going to interact with my body, so I moved forward with confidence that I was going to be able to juggle both.
Spoiler alert: I wasn’t able to juggle both.
First, I want to say everybody and every cancer is very different. But for my cancer, synovial sarcoma, there was to be six chemo sessions. Three high-dose of ifosfamide and three of doxorubicin, also known as the red devil, which is such a horrible name.
Six chemotherapy treatments that were not inpatient; I was able to go home. The infusions ranged from around six hours.
The ifosfamide was around eight or nine days, and the doxorubicin was three to five, depending on my white blood cell count and my overall blood panel, how I was doing immunity-wise.
That took four months to complete. I wasn’t able to complete my sixth session because my body wasn’t able to bounce back. I was essentially neutropenic. Then I moved forward with surgery and 36 rounds of radiation afterward.
Chemo pump and the outpatient experience
I went to the hospital, got infusions, but I actually was attached to a 24/7 pump when I was not in the hospital.
I called it my toxic boyfriend because it just kept on coming back into my life. It was a little fanny pack.
I remember stuffing dryer sheets in it because it just smelled so chemical and awful.
I was attached to it through my PICC line 24/7. I would go in for my infusions at the hospital and get fluids, sodium bicarbonate, to help support my body and keep everything in check.
Thankfully, I was nine blocks away, so some days I wasn’t able to walk, but most days I was able to walk to the hospital, which was unbelievable.
I would go in every single day. The ifosfamide was a longer treatment, so it was around that one-week to nine-day mark. The doxorubicin, I would go in every single day around three to five days.
How many days did you have “off” of chemo infusions?
I had two weeks off. That one week to 10 days right after my chemotherapy treatment, I was knocked down. I was neutropenic, so I wasn’t able to completely function. I wasn’t able to function at all, actually. I was bedridden.
Then I would have one week a month where I could go around the city, go to other doctors, like a physical therapist. I was working with a trainer. It was one week a month where I could really live.
Chemo side effects
Summary: dehydration, fatigue, nausea, a few mouth sores, bone pain (from Neulasta shots)
I was really nauseous; I was dehydrated; I was fatigued. I definitely got sick regularly, but I was really able to hone in on what was working for me toward the end of chemotherapy.
One of the most important things for me, being a petite woman, was to gain weight rather than lose weight. So I would really try to nourish my body with pretty much whatever I could get down and keep down. I would eat and nap right after so I wouldn’t get sick.
I remember being so fatigued and in pain, too. The bone pain from Neulasta and some of these shots that happen after you do chemotherapy to help maintain a stable white blood cell count — they’re so painful. The bone pain is excruciating.
I remember taking these baths at 3 or 4 a.m., filled with Epsom salt, trying to soothe my body in any way that I could.
Baths were a huge ritual for me that I started to integrate into my routine and still do all the time today.
Fatigued, nauseous, and that bone pain were really the main ones. And mouth sores! I got a few really painful mouth sores as well.
What helped with the chemo side effects?
The Claritin didn’t work for me (for the bone pain). I took it, but I still had crazy pain. There was another one outside of Neulasta that worked better, Neupogen. It worked better for my body.
Things that worked for me — baths were huge. Seaweed baths, Epsom salt baths. I used salts a lot to ease body pain and help me relax.
I didn’t go to therapy during treatment, but I went to Reiki in between every chemotherapy treatment, which was huge.
I started to meditate regularly. I really leaned on my family and friends. I had an incredible support system, and they were really my army.
I was able to get through my treatment and the cancer because of that, because of their support and having that cathartic release by talking and having these raw and real conversations.

Getting your PICC line out
It was a really emotional journey when I got my PICC line out. I burst out crying. It was a huge milestone for me to get that PICC line that had been in my arm for months and a part of me, part of the journey.
It was such a release physically, mentally, emotionally — all of the above.
Hair Loss
How did you decide what to do with your hair before losing it?
I remember that was the first question that I asked the oncologist in our meeting. I come from a fashion background, and I was a young 20-something-year-old. I was like, “Am I going to lose my hair?” First question I asked.
It’s part of your identity as a young woman, for sure. It was really tragic for me to think about. My doctor was like, “I would get it cut right away.”
I started chemotherapy, and in the middle of my first chemo session, a high dose of ifosfamide in that nine-day long chemo cycle, I had all of my friends come with me to Bumble and Bumble in NYC.
They gave me a private room, and we threw a dance party as I cut my hair into pixie. My hair wasn’t really falling out, yet, but I wanted to just get to it and maybe try to cut it so I could donate it or make a wig out of it.
By the way, there’s a very particular way you need to cut your hair if you want it made into a wig. I even talked to my stylist. They said they were going to do it correctly, but it ended up being the wrong way, so I wasn’t able to make a wig out of my real hair. Do your research on that.

I got a pixie cut. At first I thought it was going to be a really traumatic and emotional experience. Because I had an amazing support system, it was almost like a celebration. A liberation.
Looking back, it’s a very bizarre feeling and experience for that type of situation. I really have to thank my friends and support system for that being a more celebratory time in my mind, rather than a really sad moment. Not to say that that sadness didn’t kick in; it did.
»MORE: Dealing with hair loss during cancer treatment

When did you notice hair falling out?
At the time, after I finished my first treatment around the two-week mark, I really started seeing my hair falling out. It was around New Year’s, and I remember waking up next to my then boyfriend.
My hair was just covering my pillow. I had a porch right off my room, and I remember shaking my pillowcase on my porch.
My boyfriend woke up and said, “What are you doing?” I said, “It’s everywhere.” It was so hard for me. I said, “I need to just buzz my hair.”
I ended up going to a salon down the street, which I would not recommend doing. I would recommend getting electric clippers and doing it yourself, because post-chemotherapy, my immunity was low, and I ended up getting a rash on my head. So it’s better if you buy your own hair clipper and do it yourself.
I went to a random salon down the street and had someone else do it for me and brought my friends there. Tried to make it a more celebratory experience, but that one was when I was in a darker state. I was also starting to feel more sick, so that was a little harder for me.
I was fully bald probably a month in. It was really quick.
Tibial Nerve Surgery
Deciding post-chemotherapy treatment
I remember going back a couple of times for what was supposed to be my sixth chemotherapy treatment, and my counts were just not rising.
I could not get my body back to a point where I could take another round of chemo, so we decided and landed on five chemotherapy sessions, getting a scan pre-surgery, then moving forward with a tibial nerve removal.
Deciding on which surgery to pursue
I had multiple options there. There’s a spectrum, liberal surgery on one end and more conservative surgery on another.
I could have taken out part of my tibial nerve. I did take out my entire tibial nerve, which was the middle-of-the-road option. The most radical option was amputation, which had the lowest rate of recurrence.
Again, this is a situation unique to every person, their age, where they live, what they do, but it really resonated with me most to take the middle-of-the-road option and move forward with tibial nerve removal.
That was a decision that I took. I didn’t take it lightly and talked to multiple doctors and multiple surgeons.
In addition to my chemotherapy, the decision to stop early, I talked to multiple oncologists and multiple doctors to ensure that I was taking the right route. That felt best for me.
At the end of the day, it’s your decision. That’s the most important. You have to feel good and confident moving forward with that decision.
I have a unique circumstance because I didn’t have a tumor in my body. We couldn’t see if the tumor had necessarily shrunk or not.
The pieces left in my body were so small that we weren’t really able to see if there was a material difference in size, but overall, we were optimistic that it was working.

Describe the tibial nerve surgery
I was on full-on warrior mode at that time. I was moving forward. I really wasn’t showing that much emotion at that time. My family and friends were feeling it for me. I took time after to feel the feels, but it was a really long surgery, really extensive.
It was eight hours. I went in thinking I was actually going to lose motor function of my left foot, so I was going to have drop foot. This is something I was mentally prepared for and spoke of with my surgeon very frequently, and with my friends and family often. I had all these tools and wraps to help me recover.
I was mentally there, but after I got out of my surgery, I remember waking up in my recovery bed and I was able to move my foot instantly. I had a miracle surgery. They were able to save this motor function of my left foot.
They couldn’t see anything in the scans that would show I would save my motor function, so they were able to see it when they opened my leg up. It was a miracle surgery.

Processing the news of best-case surgery results
My life could be completely different. My doctors told me that I was never going to do yoga again, never going to run again, or do all these things that I’m so blessed and so grateful to be able to do today.
It’s crazy that your life can change so much. To realize that this can happen to anyone as well. I’m just so blessed with my journey. I think I really have to thank not only my doctors, my nurses, and my community, but I wholeheartedly believed that this was a miracle surgery.
I was so steadfast in moving forward. I was like, “I will be fine.” I remember telling my doctors after they were like, “You know, you might not be able to run or do yoga again.” I was like, “You don’t know me.”
Although people can say so many things that can cause roadblocks in your mind, keep that positivity and optimism because miracles can happen, as cheesy as that sounds.

Getting surgery and radiation at a different hospital
I was split at that time between NYU and MSK, my radiation and surgery, because I was more diligent about getting second opinions and meeting with different surgeons. My oncologist was at NYU, and my surgeon and radiologist was at MSK.
Radiation Therapy
Describe the radiation plan
It was 36 days, which was originally 30 days, but we had to bump it. I can’t remember why we increased it. I think they wanted to take a more aggressive approach.
How were the radiation sessions?
It was really short. I started going to radiation fairly quickly after my surgery, a few weeks after. I remember I was back to work during radiation as well.
I was doing half days. I can’t remember the exact amount of time, but it was way quicker than what I thought radiation was going to be, maybe 10 to 15 minutes. I could listen to my music, and that’s when I leaned into meditation a little bit more.
Radiation side effects
I definitely got extremely fatigued. I did get burns, but I am a clean beauty enthusiast and started to lean into that more as well. As I started to expand my knowledge about wellness, clean beauty was a part of that.
I did see burns during the latter part for a couple weeks and saw peeling, but I was really diligent about applying creams, serums, and oils.
»MORE: Read other patient experiences with radiation therapy
How did radiation treatment end?
I remember being like, wait what? You wait for that moment throughout the entire treatment journey. I’m so excited for that day. I’m so excited to ring that bell (for radiation).
When that day comes, you’re like, wait. You’re losing that support, which was for me a mental switch. I was leaning on them so much that it’s like you’re flying the coop. It can be really scary.
It was a ton of mixed emotions, which is completely normal. You’re celebrating but really scared at the same time, but that’s what life is about. There’s so much uncertainty day to day. You just have to keep on moving forward.
Overall, it was such a beautiful and celebratory moment. I flew with a ton of my friends to Colorado. We had a celebration, a party. At the end of the day, tons of mixed emotions, but the majority were so positive.
It was a huge sense of relief to not be living on this timeline where I was consistently looking two weeks down the road to my next chemo treatment, next doctor’s appointment, or next scan.
I have scans regularly now, but it’s different and on a timeline that’s more mine and my life, rather than the doctor’s.

Reflections
PTSD
I would take my computer into every single surgical consultation and conversation and write down all of this.
I never looked back on that. I probably have a little bit of PTSD and blocked it out of my memory.
Dealing with emotions in the beginning vs. later in treatment
I had to be a little more gentle with myself. As you go through treatment, more emotions start to unearth. You start to go through this roller coaster and this tumultuous health journey.
In the beginning, it was definitely lighter, and I was starting to immerse myself in this dark journey.
There’s light along the way, but it was harder to deal with as I started to look more and more like a cancer patient.
How did you ask for support?
That was one thing I was very good at, transparent communication, because I didn’t have the energy. I definitely needed support.
Today we have Uber and Lyft, but I had to be careful when my counts were low to be using those types of vehicles, to be very cautious of germs, wearing a mask and everything. So I had support in transportation there.
Meals, I was very lucky to be connected with a lot of meal delivery companies through my journalism and editorial background. I had delivery regularly. I was ordering so much people got me Seamless gift cards and everything.
I was able to make that work because I was so transparent with my community, with my friends and family on what I really needed and when I needed help.
Something that was really amazing for me that I did in the beginning before I got really sick was make a Google calendar of my chemo appointments. I had a group text with all of my friends and family. I sent my Google link of calendar with these dates and said, “This is when I need support. This is when I need help.”
I have such an incredible support system that they were able to all take charge and pick a day that worked for them, if it came to working remotely or taking time off. It was really about me creating the infrastructure for success.

How did you process the experience as a young adult cancer patient?
I don’t think there’s any way to process it, right or wrong. It was really hard for me to look in the mirror, seeing myself change and not looking like myself. That was really when I started to embrace a deeper journey of self-care and self-love.
This sounds cheesy, but I was really embracing affirmations and saying them out loud to myself in the morning. I looked in the mirror, and as I was seeing myself as a bald alien, being like, “I still love you. You’re still healing. I am healing, I am love, and I am still beautiful.”






One thing coming from a fashion and editorial background, I had photoshoots scheduled when I was healthy and when my immune counts were good in between chemotherapy sessions. That made me feel like me again.
I used Rent the Runway and would get dressed up. Those moments were so fun for me. That can look different for different people. Photoshoots were a big thing for me, and getting out every now and then with my friends was a big thing for me.
Accepting that you’re in this state, making the best of it, but also doing things that make you feel you again. I don’t think there’s anything wrong with that.
One thing I did with my girlfriends is we had a wig brunch at a fun brunch place and all wore colorful wigs to celebrate the end of my treatment and my journey.
Again, there’s no right or wrong way to deal with your physical body changing throughout treatment.


How did cancer change your life perspective?
For me, it was about embracing a deeper sense of love and acceptance. Going through cancer did that for me. It provided a deeper perspective on life and a deeper appreciation of my body as this beautiful vehicle and vessel of life.
Whereas I was coming from the fashion industry, where you get caught up in the material things. When you’re stripped down to just your core, you have nothing else to embrace but that.

Last message to other patients
It was dark and a shitty, tumultuous journey going through cancer and treatment, but at the end of the day, it has been such a positive catalyst and conduit for change in my life.
It enabled me and motivated me to launch my own company and to embrace spirituality and bring this mindfulness to the masses. To share my story and help others.
It’s been a beautiful journey at the end of the day. I’m not grateful for my cancer by any means, but I’m grateful for the transcendence that came about from my trauma.
That post-traumatic growth is not out of reach for you, if you’re a cancer patient and going through this journey. Post-traumatic growth can happen. It doesn’t always have to be PTSD.
That’s something I’m really embracing right now. I feel very grateful to be on this upward journey.

Inspired by Kara's story?
Share your story, too!
Synovial Sarcoma Stories
Kara L., Synovial Sarcoma, Stage 1B
1st Symptoms: Pain behind left knee, needle-like sensation in left foot
Treatment: Surgery to remove what was thought to be benign tumor, chemotherapy, final surgery, radiation (36 sessions)
...
Jillian J., Synovial Sarcoma, Stage 3
Cancer Details: 5% to 10% of sarcomas
1st Symptoms: pain in leg over 15 years
Treatment: Tumor resection, thoracotomy
...

