Sheree’s WM Non-Hodgkin’s Lymphoma Story
Sheree shares her story of Waldenstrom Macroglobulinemia (WM), a subtype of non-Hodgkin’s lymphoma. She describes undergoing 6 rounds of chemo, side effects, self-advocating as a patient and what support helped her the most.
- Name: Sheree N.
- Diagnosis:
- Waldenstrom Macroglobulinemia
- Subtype of non-Hodgkin’s lymphoma
- Staging: N/A
- 1st Symptoms:
- Feeling anemic
- Treatment:
- Chemotherapy
- Bendamustine and rituximab
- Infusions for 3 days every 4 weeks, for 6 rounds (6 months)
- Days 1 & 2: Bendamustine, 1-1.5-hour long infusions
- Day 3: Rituximab, ~8-hour drip
- Chemotherapy
- Diagnosis
- Treatment
- When did your doctor start talking about the need for treatment?
- How did your oncologist describe the chemo regimen?
- Why did you decide the IV instead of getting a port?
- Tip: No coffee before infusions!
- Describe the allergic reaction (3 cycles) to the rituximab, both at the clinic and at home
- What were some of the "smaller" side effects?
- When did the allergic side effects get better?
- A positive change with the side effects
- What drove you to go elsewhere for treatment?
- Advice on going to larger or smaller treatment
- What were the different side effects for the remaining 3 cycles of chemo?
- Finishing Treatment
- Reflections
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
My biggest need for support when I’m going through a health concern is nurturing and compassion. Someone else may be totally different. My husband was with me through chemo, and I had 3 of my best friends who’d sit with me as well.
That’s really important. It would give him a break if he was getting to the point where he needed to do some work or stressed out with my issues because the spouses go through stuff, too.
For me, it was nurturing, compassion, conversation, the friendship, the hubby being there, knowing you can count on them to be with you.
Sheree N.

Diagnosis
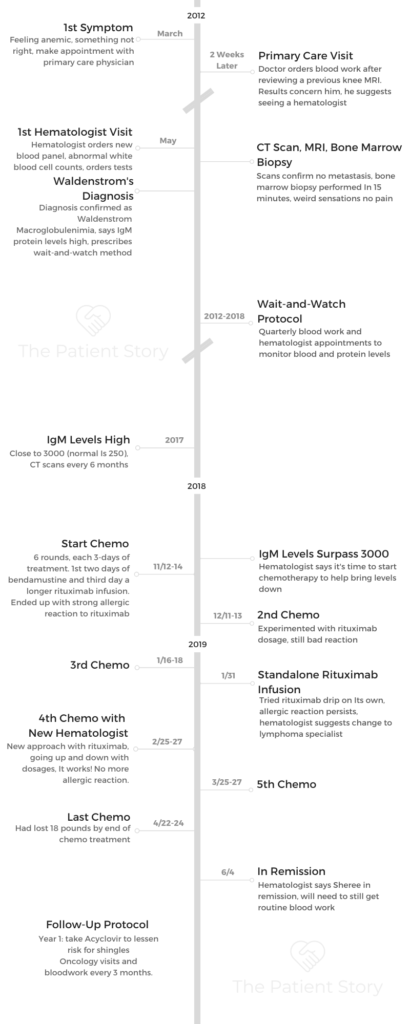
What were your first symptoms?
I don’t know if there’s this intuition that you’re feeling something is wrong with the body. I was feeling really anemic and not myself. I did have a medical doctor appointment. They decided to run blood work.
My primary care doctor was so smart. He took a look at all my other records that were on file, and he said that he noticed something was going on with my knee MRI.
There was a hotspot in there. Something doesn’t seem right. He wanted to run a blood panel on me because he was concerned maybe I had an autoimmune disease.
They ran the blood test, and he said it appeared there was something serious going on with my blood. He wanted me to see a hematologist.
How did you choose which hematologist to see?
My primary care doctor recommended one, but I remembered that my cousin worked at Washington University St. Louis. I called him that night. I asked if he knew any good hematologists. I had already looked up on Google for St. Louis’ best hematologists and asked if he knew anyone at the Siteman Cancer Center.
He didn’t but offered a friend who did know someone and would connect me with her. Fluke thing, the very next day at 10:30 a.m., the office of Elaine Majerus called me to schedule an appointment. You can’t even get in to see her because she rarely takes referrals.
Describe that first meeting with the hematologist
When I got to her office, I called my husband at work and said I needed to pick him up from work because we were going to the appointment now.
They did a blood panel, and she said she saw something in there that looked like my white blood cell count was off. They did a body scan, and I was scheduled for a bone marrow biopsy. It came back that I had Waldenstrom’s. That was June 2012.
Describe the CT and MRI scans
The CT scans are not scary. The very first one was because I didn’t know what to expect. It’s a donut hole you can see out the other side, and it wasn’t a big deal.
On the other hand, for the MRI I had to take an Ativan to do it because if I can’t see out of the end of the MRI or if my head is in the MRI, it’s a little nerve wracking, to be honest. But they only did scans down from the chest to the pelvis, so my head was typically out. If I looked up, I could see the ceiling.
That was the only thing out of the MRI machine — my nose, eyes and forehead. I didn’t like the MRIs at all.
They were always looking for cancer in my organs, lymph nodes. They checked that to make sure the blood cancer hadn’t spread to my organs.

Describe the bone marrow biopsy
I am not a person to take pain pills. I can’t stand them. When I was in the hospital for liver surgery, they gave me Percocet, and it wigged me out. I’m an ibuprofen or Tylenol type of gal.
I did get nervous before my first bone marrow biopsy, and I asked if I could have an Ativan. They said they couldn’t give me a pill form but could give me a sublingual (under the tongue) form. It’s a strip you put in your mouth, and it dissolves like a pill. It really makes you relaxed.
I was lying face down, so I didn’t know what was happening. They numbed the site where they were going in. The instrument was like a drill screw in a cylinder. I didn’t ask to see this thing before I did my first bone marrow biopsy. I did not want to know.
I was face down, and they were playing a jazz station. My husband was in the room with me. They were giving me prompts, like, “We’re going to tap. Tell me if you feel any pain or sensation in your legs.” Then they said I would feel a twisting.
When they would tell me ahead of time what I would feel, I wouldn’t be surprised by it. The whole area was numb, so I didn’t feel anything except a weird sensation in my limbs.
They would get to the point and say they would aspirate, meaning they would take some bone marrow. They took some bone marrow out. I asked to see it, which a lot of patients do not, but I just thought it looked interesting.
It looked like this beautiful crimson-white seahorse the first time it was taken out of my body. I thought it was wild. It was really beautiful. I’m looking at my bone marrow!
I was just really kind of excited by the whole thing. My husband took a picture for me so I could save it, which I still have somewhere on my computer.
The whole procedure probably took less than 15 minutes. I did not let the biopsy bother me. Then I had another bone marrow biopsy before chemotherapy, which was in 2018.
That was at a different location. When they did that one, it looked like a little beautiful white-crimson snowflake. I’m an artist and photographer!
She said they would keep watching me, and I would get scans and blood work.
Your doctor prescribed wait and watch
After my bone marrow biopsy, I had a follow-up appointment with the hematologist. She said that they were going to monitor me.
My IgM protein levels were way out of whack. I think it was somewhere in the thousands, and a normal person is under 250 for that protein level.
She said they would keep watching me, and I would get scans and blood work.
My faith also helps me, because I try to turn it over to God. Sometimes I forgot and I tried to take control of the situation, but it was easier when I let it go.
Sheree N.

How did you process this initial diagnosis?
My father passed away from stomach and liver cancer, so cancer was part of my life. I had been around friends with cancer as well.
My cousin had non-Hodgkin’s lymphoma. I’m not sure what the particular name was, but he lived with it all his life. He never had chemo. I was hoping I would be like him.
When I was told I was going to be monitored, I wasn’t too worried about it because it was just a monitoring phase.
My faith also helps me, because I try to turn it over to God. Sometimes I forgot and I tried to take control of the situation, but it was easier when I let it go.
I’ve also had about 13 surgeries in my life on other parts of my body — organs, limbs, neck — so I’m used to being poked and prodded all my life.
This was just another obstacle to get over.
The main thing my hematologist told me was that the answer was that Waldenstrom’s was manageable and treatable. I could deal with that. I could live with that. Those words were important to me.
»MORE: Processing a cancer diagnosis
Treatment
When did your doctor start talking about the need for treatment?
The routine scans and blood work went on like that up until 2018, and then my numbers started to spike.
I looked at my chart once I got on the BHC network and noticed in 2018, my IgM levels were going up to 3,000, which is really abnormal.
In the beginning of 2018, my hematologist said she was thinking that I’d have to do chemo that year. I responded, “Okay, let’s get this done. Let’s do it.”
My husband said I was very ready to go.

How did your oncologist describe the chemo regimen?
That was the first doctor, Elaine Majerus. She said I’d need 6 months with 25 days off in between treatments, so 3 days of treatments.
The first 2 days would be bendamustine, which would take an hour or hour-and-a-half to go in my body. The last day would be rituximab, and they estimated that as an 8-hour drip, at least.
Why did you decide the IV instead of getting a port?
The port probably would have given me anxiety since I knew it was only going to be 6 months of treatments. This thing sticking out of my chest, I wouldn’t have been able to sleep, so I chose to go with getting stuck each month.

Tip: No coffee before infusions!
Anybody going through chemo, don’t drink coffee before you get the IV in your arm, if you’re not doing a port. What it does is dehydrate your veins.
One time they took 3 tries before they could get it in, and the nurse said no coffee before chemo. The moment it was threaded in my arm, I would send my husband for coffee!
Describe the allergic reaction (3 cycles) to the rituximab, both at the clinic and at home
At the chemo infusion center, they would start with a certain milligram of rituximab and keep increasing it. Each time they got it to the next level, I’d have some sort of reaction.
The first 3 months, the reactions ran the gamut from headaches to feeling like my throat was closing up, feeling like I had the flu. One month they thought I was having a heart attack, so they hooked me up to an EKG.
Each time I had a reaction, they had to stop the IV drip and wait at least 20 minutes, give me a Benadryl and restart the drip.
The first 3 months, I was only able to get 40 to 50% of the rituximab in my body. The very first month at home, about the second day after the chemo treatments, it was a living hell, to be honest.
It started in the evening when I started throwing up with nausea. Really bad headaches, I felt like I couldn’t catch my breath, couldn’t get enough water or liquid in my body. I was to the point where I was throwing up bile.
My husband urged me to call the nurse, so I called them.
My husband had been to Target about 6 different times to get me different things to take at the recommendation of the nurse, because we didn’t have any Benadryl in the house. He got that, probiotics, yogurt, anything I could try and keep down using the BRAT diet.
I took a partial Ativan and slept for a couple hours. I got up, took a bath and then it would start all over again until about 3 in the morning. I was calling the exchange, again, and they were advising me what to do.

There was something you put in your throat to make it moist. My husband went back the next day to Target to get more things for me. I think I called the nurse 6 times in less than 24 hours.
By that point, I was so anxious and wigged out because of the reactions from the chemo that they advised I take another Ativan. I took a full Ativan, and I slept through the rest of the day. I got up to eat dinner and was able to keep some applesauce and probiotics down.

What were some of the “smaller” side effects?
My tastes were changing, because nothing tasted good to me. I would drink a soda, and it would make me throw up. It may have been the sugar. It was one of the harder times of my life during that weekend.
They tell you not to go anywhere for the first 4 days after treatment because you are immunocompromised. I remember one time we were driving around looking for food to eat because I couldn’t make up my mind. I’d say something was good, and then 5 minutes later I would change my mind.
I was literally driving my husband crazy because I think I wanted something to eat, but in a few minutes I would change my mind. It was really hard to plan meals for a while!
The really sad thing is I lost my taste for coffee for the first 2 months. I am writing a poetry book about coffee, but it was really sad because even the smell of coffee made me sick.
When did the allergic side effects get better?
By about the fourth or fifth day of the first treatment afterwards, the nausea started to go away. That was a great thing. By the tenth day, I got my taste back.
A positive change with the side effects
A good thing that happened was when you’re sick, your body knows it and rejects certain foods. My body rejected junk food. I would get sick, stomach cramps or vomit on junk food. That was a good thing because I started eating better.
The meals we had when we cooked were healthy meals. To this day, I still try to do that. I used to have this love for Fritos. They actually just turn my stomach now. I used to be able to eat an entire bag of Fritos in one sitting, and they’re nothing but grease and oil!
I don’t want that. To this day, I hate sugary drinks. No sodas, no sugary juices, no sugary lemonades, even coffee syrups. I don’t drink any of that and haven’t for 2 years. It’s mainly water for me, herbal teals, black teas and small amounts of coffee.
I love red beets now. My mom used to feed me red beets nonstop as a little girl, and I got so sick of them. But the moment I went through chemo, I just had this craving for red beets again.

What drove you to go elsewhere for treatment?
Dr. Majerus actually had a meeting with me. She tried to do a rituximab session by itself within a couple weeks of the third infusion. That did not work either.
She referred me to Dr. Neha Metah-Shah. She said she is a lymphoma goddess.
When I got turned over to her, I met her team: her nurse practitioner, Jennifer, and nurse, Becky. Becky is the one who figured out a spreadsheet to give this rituximab in my body where they would go slowly, take it up, but the next level they would bring down.
I was up and down, up and down all day. The first time in 4 months, I got out of my treatment in 6.5 hours.
I did have a little reaction at the end, which was the sniffles or the flu. That was the last hour, and they gave me Benadryl. It was relief. They did that at a different center.

These are some of the nicest nurses I’ve ever met in my life. They’re just amazing.
Advice on going to larger or smaller treatment
I did some of my treatments at the West County in St. Peters location, the short days. They did not see that many patients, but the downtown location, this is all they do all day long. There’s different chemo treatment pods, and the hallway I was in must have had 8 treatment pods.
You go into a pod. There’s normally 6 people in the room with you. These nurses, this is what they do all day long from the time they get up to the time the facility closes at night.
They are there for the long haul. You have your morning nurses, and you have your afternoon shift that comes on. These are some of the nicest nurses I’ve ever met in my life. They’re just amazing.
What were the different side effects for the remaining 3 cycles of chemo?
I slept and became tired.I had no other problems with anything, maybe a little nausea, but I was just tired. Day of treatment, I would go to bed when I got home. I usually slept great periods of time for at least 2 days after and woke up feeling like a new person.
My sense of taste got “smaller,” and the nausea always stuck with me for a couple days instead of 5 days.
Finishing Treatment
How were they monitoring your progress?
They were monitoring all of my levels, but the IgM protein was the main one they needed to get and check. They did a CBC (complete blood count), among other tests. Once they got it to a more normal range, that was it for me.
The doctors know it takes about 6 cycles of treatment from experience. Then we were done.
Describe what happened at the end of chemotherapy
I got to ring the bell twice.
I rang the bell the night of my last treatment at Downtown St. Louis. The nurses presented me with a certificate, which was very sweet, that I had gone through chemo treatment and survived. They gave me a survivor keychain.
We all took a picture together, and on the seventh floor there was no one in the waiting area. It was me and my husband. He videotaped me ringing the bell, and I did a little goofy dance. That was the first time I rang the bell.
The second time I rang the bell was when I went for my check-up, which was in the beginning of June at the doctor’s office at the West County location. She said, “I just want to tell you you’re in remission.”
I started crying. It was different ringing the bell when you finish treatment, because the first time, I really didn’t know what the numbers were going to be like or what was going to happen over the next couple of months. Was I going to be in range?
I went out in the lobby and asked the nurse, Becky, ‘Should I ring the bell? I don’t know if I should. I already rang it when treatment ended in April.’
She was like, ‘Girl, you go ring that bell!’
I went out in the lobby and rang the bell, and everyone in the waiting room clapped for me. I got emotional again, probably more emotional than the first time because it was still an unknown. I started crying and walked out.
It felt different because someone tells you you’re in remission. It felt good. I was like, “What does it mean, exactly, to be in remission?” My doctor said the lymphoma was gone. They would still have to monitor me, and I would get quarterly check-ups.
What has the follow-up been like?
I just had a check-up 2 weeks ago. We were all masked up (because of COVID-19) of course. I had my CT scan the week before, and that was normal.
My numbers are starting to climb a little bit, but they said it’s no concern. I believe my IgM level was at 472, and normal is 250. But like I said, my doctor doesn’t really get concerned until you hit the 2,000 range for some reason.
I’m thinking it took 1 year to climb 200 points, so maybe I’ve got another 10 years before I have to do chemo again. Hopefully, I don’t have to ever do it, but it’s not something that you can just say that you won’t ever have chemo again, because you may.
Reflections
Guidance on self-advocacy in choosing the right doctors
Be open to what the doctors say to you. If you don’t jive with your doctor, get a new doctor. For me, I researched the best hematologists in St. Louis. Why not go to one of the best ones?

You don’t have to go to a doctor whom your primary care doctor recommends if you don’t want to, if that’s not what you feel in your heart is right. You go to the best doctor for you in that field.
We have 2 other friends, my husband and I, and all 3 of us were diagnosed with lymphoma within a couple weeks of each other in 2012.
I think that our one friend Dave is a walking miracle, and our other friend Rick had lymphoma twice. He’s been in remission. They found the best doctors for them.
Don’t settle, because it’s your life we’re talking about. You do what you want and go to whom you want. If they don’t jive with you, go to someone else. That’s a big part of being comfortable and hopeful in your journey.
»MORE: How to be a self-advocate as a patient
That’s really important. It would give him a break if he was getting to the point where he needed to do some work or stressed out with my issues, because the spouses go through stuff, too.
What was it you needed the most support for?
My biggest need for support when I’m going through a health concern is nurturing and compassion. Someone else may be totally different. My husband was with me through chemo, and I had 3 of my best friends who’d sit with me as well.
That’s really important. It would give him a break if he was getting to the point where he needed to do some work or stressed out with my issues, because the spouses go through stuff, too.
For me, it was nurturing, compassion, conversation, the friendship, the hubby being there, knowing you can count on them to be with you.
»MORE: What kind of support cancer patients say helped the most
What helped you get through the hardest times?
I relied on my friends a lot to talk. If I wanted to have a good cry, I’d give them a call, and we’d talk for a long time and visit. My faith helped me get through the journey, and my husband was there for me along as well, even though I probably drove him crazy! Like I mentioned, he went to the store 6 times in less than 4 hours.
I even went to talk to a counselor on my own. It was someone we’d used before for something else, but I didn’t get that compassion from him. It may be more of a “woman” thing. I think women feel comfortable talking to women about stuff like this.
I did have anxiety. I typically had anxiety the first 3 or 4 days after chemo. I don’t know if it was from the chemo or if it was from the Ativan I was taking. Ativan is supposed to help you, but sometimes if you’re coming off of it, you get jittery.
I made sure for the last 3 months, I weaned myself down to a quarter of a pill if I needed something, and that might be twice a day for the first 3 or 4 days. I prayed a lot and got out. When I could walk in nature, usually after the third or fourth day I felt comfortable being to the park with the dogs.
I still do that to this day. Every morning I get up I do my breakfast routine, take care of the animals, and the first thing we do is get out the door, get in the car, go to the park and walk. It’s good for them, and it’s good for me. It helps me get my head straight for the day.

Guidance for patients and their caregivers
If you’re the person going through the cancer, for me, it was always just trying to stay focused and listening to what the doctors were telling me.
It’s going to get bad at some point. You are going to go through storms, but those storms are going to be over with, and then you wait till the next storm happens. You just go through it.
Don’t be afraid to take an Ativan if you have to. It does help relieve some stress. You don’t want stress in your life. I’ve been getting too stressed out lately with my other health concern.
It goes back to the team of doctors you have. If they make you feel confident, then you’re very hopeful. Praying helps.
If you’re the caregiver, realize that the patient may go crazy sometimes, as my husband has probably found out. I think it’s hard for them because they don’t know what you want. One minute you want something, the next minute you might want something else.
They’re trying to keep up with your requests, and it stresses them out as well. Just a note for the caregivers, be patient and compassionate and nurturing. It helps the patient be calm.





Inspired by Sheree's story?
Share your story, too!
Waldenstrom Macroglobulinemia Stories
...
Pete D., Waldenstrom Macroglobulinemia
1st Symptom: Irregular blood test results during a regular workup for Crohn’s
Treatment: Chemotherapy, surgery, radiation, monthly IVIG
...
Sheree N., Waldenstrom Macroglobulinemia
Cancer details: Only ~1000-1500 new cases in the US each year
1st Symptoms: Feeling anemic
Treatment: Chemotherapy (bendamustine and rituximab)
...
Cindy S., Waldenstrom Macroglobulinemia
Cancer details: Only ~1000-1500 new cases in the US each year
1st Symptoms: Hyperproteinemia
Treatment: Chemotherapy
...



