Brianna’s Stage 2B ALK+ ALCL Non-Hodgkin’s Lymphoma Story
Brianna was diagnosed with stage 2 anaplastic large cell lymphoma (ALCL), a non-Hodgkin’s lymphoma T-cell subtype, specifically the ALK-positive (ALK+) ALCL.
Brianna talks about undergoing surgery and chemo, as well as quality of life issues including hair loss, advocating for herself as a patient and preserving fertility.

- Name: Brianna B.
- Diagnosis:
- Anaplastic large cell lymphoma (ALCL)
- Non-Hodgkin’s lymphoma subtype
- ALK+
- Staging: 2B
- Treatment:
- Surgery
- Removal of left ovary, fallopian tube, lymph node
- Chemotherapy
- CHOEP
- 6 cycles; infusions for 3 days every 28 days
- Radiation therapy
- 20 sessions
- Surgery
- Diagnosis
- What were your 1st symptoms?
- What made you finally go to the doctor?
- After you were admitted to the hospital, what tests did they run?
- What was the lymph node biopsy like?
- What happened after the misdiagnosis?
- What was the exploratory laparotomy like?
- How did you get officially diagnosed?
- Processing news of a cancer diagnosis
- How did you break the news to your friends and family?
- Describe the bone marrow biopsy
- Treatment
- First meeting with your oncologist
- Describe the procedure to get a PICC line
- Is there anything you wish you had known up to this point?
- Describe the CHOEP chemotherapy regimen
- What were the chemo side effects?
- Advice for someone who’s about to start chemo
- Why did you need to have radiation?
- How did you feel going into radiation?
- What's radiation like?
- Radiation side effects
- Biopsies after radiation
- Results after radiation
- Survivorship
- How did you react to being told you were in remission?
- Processing the entire cancer experience
- What is your ongoing follow-up protocol?
- What was the biggest surprise for you during treatment?
- How has cancer changed your perspective?
- How did the hair loss affect you?
- Advice on dealing with hair loss
- Was there a point when you had to advocate for yourself?
- What’s your advice for someone who’s nervous about standing up for themselves?
- Preserving fertility using Lupron shots
- What is your “new normal” after cancer?
- Support
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.

Try to take care of yourself, but if you can’t, know there are people who will surround you and help when you can’t do it on your own.
Allow yourself to feel however you need to feel. Don’t bottle up emotions. Don’t try to hide. Don’t try to pretend that you’re happy or fine when you’re not. Your feelings are valid and need to be expressed.
You’re allowed to feel scared. You’re allowed to cry into your ice cream after you’re told you’re in remission. You don’t have to be the happy, strong cancer warrior all the time.
Brianna B.
Diagnosis
What were your 1st symptoms?
Loss of appetite and weight loss, which I misconstrued as something that was happening on purpose because I was trying to lose weight at the time.
Everything snowballed after that. I was getting lots of fevers, inflammation and stuff like that. The initial symptoms were the weight loss and loss of appetite, though.
»MORE: Read more patient experiences with first symptoms of lymphoma
What made you finally go to the doctor?
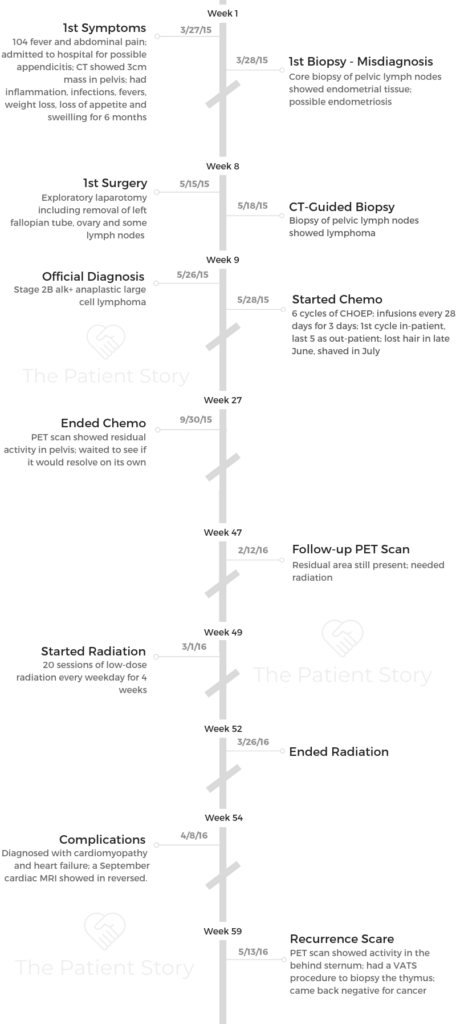
I first went to the doctor for swelling in my left leg. They did some ultrasounds. What really got the ball rolling was when I went to the doctor for a fever of 104 and some abdominal pain.
They sent me to the ER for what they thought was appendicitis. They did a CT scan that showed a small 3 centimeter mass in my pelvis. That’s when I was admitted to the hospital, and all the real tests began.
After you were admitted to the hospital, what tests did they run?
They did a lymph node biopsy, but I’m not sure it was done correctly. There was so much inflammation that they ended up getting endometrial tissue and diagnosing me with endometriosis, which I don’t have.
What was the lymph node biopsy like?
It was painful. I have had a few now, but the first one was the worst of all the biopsies I’ve had. I was in a lot of pain at the time, and I had inflammation everywhere. I was feeling so sick. I had to lay flat for quite a long time.
It took them a while, and they hadn’t numbed me super well. When they took the core biopsy, I felt like I got punched in my stomach, so I flinched. That made it even worse.
The results didn’t take too long. Initial results only took a few days.
What happened after the misdiagnosis?
I was referred to a gynecological oncologist. He decided he would do an exploratory laparotomy to see how bad the suspected endometriosis was. I also had a cyst on one ovary that he was going to take a look at.
He didn’t find any endometrial tissue outside of where it should be, so there was no endometriosis. He removed a cyst from the ovary and had to take the ovary and fallopian tube with it. He removed some lymph nodes from my left side that were causing the swelling in my leg.
After that surgery, he did a CT-guided lymph node biopsy in my pelvis that ultimately found the cancer.
What was the exploratory laparotomy like?
They made an incision from my belly button down to my pubic region and opened it up to explore. Recovery was difficult. They had cut open my abdomen through the abdominal wall. That made it hard to get up and move around.
How did you get officially diagnosed?
To break it down, at the end of March, I went to the ER with the suspected appendicitis. That’s when they admitted me and did the first biopsy.
I got a misdiagnosis of endometriosis. Over the next 2 months, I was in and out of the hospital with infections, dehydration and fevers.
During that time, I met with the gynecological oncologist. He did the exploratory laparotomy on May 15th. After that surgery, they did a CT-guided lymph node biopsy.
On May 26th, I got a phone call with the results from the biopsy. That was my lymphoma diagnosis.
The next day, I went in to have the staples removed and met with my oncologist. I was admitted to the hospital, got my PICC line in, and I started chemo the day after that.

Processing news of a cancer diagnosis
Up until that point, I kept saying to myself, “As long as it’s not cancer, I’ll be okay.” Then it was cancer. I still can’t describe the emotions that I felt.
There was some relief because we finally had a diagnosis after I had been struggling for months and months. I felt so scared and shocked that I cried with my dad and then was in a daze for the rest of the day.
»MORE: Processing a cancer diagnosis
How did you break the news to your friends and family?
I had my dad call my mom because she was at work. He told her to come straight home instead of going grocery shopping. He wound up telling her. They told our relatives.
I have so many aunts and uncles and cousins. I texted my friends because I couldn’t say the words out loud.
»MORE: Breaking the news of a diagnosis to loved ones
Describe the bone marrow biopsy
It wasn’t too bad. I was more nervous about the results than anything else. The lidocaine shot to numb me was the worst part. It burns a lot. They laid me on my side.
The rest of it was just a lot of pressure. They wiggle the needles around to loosen up the sample, and that’s a weird sensation. It wasn’t very painful, but that might be because they gave me Ativan and morphine.
Results took a couple of days. Full results take longer than that. I didn’t have marrow involvement, which showed up on the initial results. That means the cancer hadn’t affected my bone marrow.
Treatment
First meeting with your oncologist
It was basically just telling him that I had a very aggressive cancer and that we needed to start right away. He laid out the next few days for me, so I knew what to expect. I ended up mostly listening.
I was too upset to even think of asking questions. My mom asked if there was anything that caused it.
My cancer was one of the ones that just happens. They couldn’t pinpoint a reason.
Describe the procedure to get a PICC line
Just like the biopsy, the lidocaine hurt the worst. They did it while I laid in my hospital bed.
It was so nice to have it in because my veins are so small, and I was so dehydrated, so no one could ever get an IV in. Putting it in took about a half an hour, and it was no big deal.
Is there anything you wish you had known up to this point?
I wish I had known how to accurately describe my symptoms and how I felt. I also wish I had known I wasn’t losing weight on purpose. I think that would’ve led to a much faster diagnosis.
Describe the CHOEP chemotherapy regimen
I got CHOEP, which is cyclophosphamide, hydroxydaunorubicin, Oncovin, etoposide and prednisone. I did 6 cycles with 3 weeks in between each cycle. It’s a pretty intense chemo.
I got infusions every 28 days for 3 days. The first one took about 6 hours because it was 3 different medications. The second and third day each took 2 hours.
I did the first infusion inpatient so they could monitor me. I tolerated it well, so I got to do them outpatient.
What were the chemo side effects?
Summary: Fatigue, hair loss, nausea, vomiting, low blood cell counts
Fatigue was a big one. It was constant. There were some days where I couldn’t even get up out of bed and take my pills. Some days I just wasn’t able to shower or make a meal.
I lost my hair. All of it. All over my body. That started late after the first infusions and progressed to the fourth infusion. By the time that was done, I had no hair.
Nausea and vomiting were pretty constant. I was having a hard time getting those under control. I tried Zofran and some other meds, but none of them really worked for me.
I went to the hospital because I couldn’t stop vomiting. One of the nurses gave me Ativan. That cleared the nausea. I cycled between constipation and diarrhea.
My blood cell counts dropped every infusion. It happened in the expected timeframe. I would need platelets and red blood cells. I had no immune system.
One of the bigger, less common side effects I had was cardiotoxicity. This was late in March of 2016, so around the time I finished radiation. I was out hiking in Phoenix. I took myself out on a little vacation post-treatment.
I found myself getting really short of breath hiking easy trails in the desert alone. I thought, “Wow, I must be really out of shape. I guess I’ll have to work a little bit harder.”
It just kept getting worse. By the time I got home from the trip, I couldn’t catch my breath even sitting down. I went to the ER after finishing a season finale of Criminal Minds.
That’s when they figured out I had cardiomyopathy. My left ventricle was enlarged. The output is normal when it’s around 55 to 75%, and it was at 25%. I was in heart failure.
The put me on several medications. I had to restrict my sodium and fluid intake. That was how they were going to keep it in check. Eventually, my levels came back up, but I’m still on medications for that and hoping to come off of them soon. I don’t have any restrictions anymore. I consider myself lucky.
»MORE: Cancer patients share their treatment side effects
Advice for someone who’s about to start chemo
Follow the directions your doctor gives you. If they tell you your white blood cell count is going to be low, and they tell you to keep yourself safe from infection, do it. Wash your hands, keep yourself away from crowds and be careful.
If your platelets are going to be low, don’t floss. Don’t do anything dangerous that might lead to you bleeding. Follow those rules because that can prevent so many complications in and of itself. The last thing you want to deal with when you’re going through cancer already is unnecessary complications.
Why did you need to have radiation?
I did a CT scan after the fourth or fifth infusion. It showed a small residual area. They said, “You’re not done with chemo yet. We’re just going to wait and see what happens.”
In November, after I finished chemo, I did a PET scan. It showed the same small area of residual activity. They said they were going to still watch it and see what happened.
They repeated the scan in January or February. It was still there, so they decided to do 20 sessions of low-dose radiation to that area.
How did you feel going into radiation?
I was more nervous that it wouldn’t work and that I’d have to get more chemo or a transplant. Mostly, radiation was just lonely. I drove myself there every week day for 4 weeks.
I didn’t look as bad as chemo made me look, so I didn’t get the same support that I got during chemo. It was like I did it on my own.
My hair was coming back. I was working and all that, so people assumed I was better.
I missed the emotional support.

What’s radiation like?
The first time I met with the radiation oncologist, they mapped out my body and determined which area they were going to radiate. They put small tattoos on each of my hips and one in my pubic area that would line me up with the machine each time I went.
With some people, they’ll just use marker, but since I was going to be getting radiation over 4 weeks, they went ahead and did the tattoos. I still have them.
I would go in, and they would put me on a table. The room was open. The machine was pretty open above me and on each side of the room. The radiation technologist would leave the room and set everything else up.
The machine would line up with my tattoos. It had my settings programed. It took longer to get lined up than it did for the actual radiation. The actual radiation only took a few minutes because mine was low dose.
Radiation side effects
The only side effects I had were diarrhea and a little bit of fatigue. The area they targeted was so small, and the area they targeted was around my GI tract.
Biopsies after radiation
After radiation was done, I had another PET scan that showed the area resolved. However, it showed activity by my sternum in my chest, which indicated possible relapse. They had to do another biopsy, and because of where it was, they had to do a surgery.
They deflated my right lung to get the biopsy and inflated it again after they were done. That was pretty rough. I stayed in the hospital overnight, but recovery was fairly easy. During surgery, I think they had my neck positioned weird because I felt like I had whiplash afterwards. That was the worst thing about it.
Results after radiation
The results came back, and it wasn’t cancer. It was something called thymic rebound.
The thymus makes T-cells. My cancer was a T-cell cancer, so it was working overtime to make new healthy cells. That’s more commonly seen in children, so they didn’t suspect it for me since I was 23 at the time.
My red blood cells were not recovering as quickly as they’d hope. They suspected I had aplastic anemia, which just means your bone marrow is not working. They did another bone marrow biopsy. It ended up just being a B12 deficiency. In the span of a few months, I had a relapse scare, heart failure, 2 biopsies and suspected aplastic anemia.
It was awful. I felt worse than I did when they told me I first had cancer. I had more of a support system when I was first diagnosed.
It was very lonely and very scary. I didn’t want to have to go through all this other stuff after having gone through cancer.

Survivorship
How did you react to being told you were in remission?
When they told me I was in remission, I drove myself to my appointment. It was June 3rd. I didn’t let anyone go with me because I wasn’t entirely sure what the results were going to be or how I was going to react.
They told me, and I tried to celebrate. You see all these videos of people ringing bells, crying happy tears and celebrating, so I tried to do that, too.
I went across the street to get some ice cream and to try and be happy. I ended up sobbing into my ice cream. I had just been through so much with the chemo and everything that happened the month and a half before this.
It was so much to process. I couldn’t just be happy. Even though this was good news, the whole thing was still the worst thing I’ve been through in my entire life. I didn’t feel like I could celebrate any part of it.
I told everybody pretty soon after. I kept so many people updated on how I was doing, and they were all excited to hear I was in remission. I didn’t throw any parties or anything. I didn’t celebrate, but I let everybody know.
Processing the entire cancer experience
It took me a long time to be okay with my whole experience. After you’re done, you’re still getting scans and blood work and seeing your oncologist so often. It feels like it’s not over. My health feels fragile, and it makes it hard to relax.
What is your ongoing follow-up protocol?
At first, I saw the oncologist once every 3 months. I did a PET scan every November for 2 years. At first the blood work was twice a week, then monthly, and it’s down to every other month now.
In January, my white blood cell count came back a little low, so they did 6 months of monthly blood work. So far, everything has come back normal. I don’t need scans now. I go see my oncologist once every 6 months.
I basically pay the co-pay to say hi.
What was the biggest surprise for you during treatment?
It wasn’t like what you see on TV. I thought I would get side effects right away from chemo, but that didn’t happen for a few weeks. You see a bunch of different things on TV. That was my only experience with cancer.
I don’t have any close relatives with cancer. I didn’t really know what to expect from lying in a hospital bed to living like you’re dying. My biggest surprise was really just the whole experience. I didn’t know what to expect from any of it.
How has cancer changed your perspective?
At the time I was going through treatment, it didn’t. I followed all the rules to make sure I didn’t get sicker. I laid in bed all the time because I was so tired.
That’s a more accurate way to think about living like you’re dying, because you feel like you could die.
Now, I would say that I take more trips that I wouldn’t have taken before. I invest more time into my hobbies.
I invest more time in friendships and family time because it means so much more to me now.
I have so many patients who come in and have just retired, and now they have cancer. They say, “I saved up everything for after I retired, and now I can’t do any of it.”
I’m determined that that’s not going to be me. While I’m healthy, I’m going to do everything I want to do and do everything I can to make my life the best that it can be.
I know the chances of me developing a secondary cancer are higher now because of the chemo I had. That may happen, and it may not. But while I’m here, I’m not wasting any time.
It’s made me more appreciative of what I have. It’s made me think I can do whatever I set my mind to now since I’ve beaten that. It’s made me a little more introspective. I spend a lot of time thinking about the world and my place in it.
How did the hair loss affect you?
I thought it wouldn’t affect me that much, but it did. I had so much going on that I thought the hair loss was going to be an afterthought.
Before that, I’d always had pretty long, thick hair. I remember one day, I was home alone and running my fingers through my hair. A big clump came with it.
I just sat there like, “Is this really happening?” I kept running my hands back through my hair and kept pulling it out since I knew it was going to come out anyway. I filled a grocery bag.
I couldn’t bring myself to shave it until it was almost all gone. I shaved it myself and had my dad help me with parts I couldn’t reach. I had a tiny ponytail, and I cut that off. Then I rocked the bald look with hats. I didn’t want to do a wig. It was much better after I shaved it.
After I shaved, I put a hat on and went to Starbucks. I forced myself to leave my house. I thought, “This is what I look like now. I have to be at least somewhat comfortable with it.” I prepared myself.
I knew other people were going to see it. I knew they were going to look at me strangely and in ways I didn’t like. I figured I might as well just start getting used to it.
I’m lucky enough that my head is a nice shape. I got used to that pretty quickly. What I didn’t get used to very easily was not having hair anywhere else. You don’t think too much about the hair on your arms or all over your body.
That all fell out, too, and felt weird. It changes the way your skin feels, especially if it gets wet.

Advice on dealing with hair loss
Let yourself feel however you need to feel about it. People will tell you that it’s just hair. People will tell you that you look good, and you won’t believe them. That’s okay. Your feelings are totally valid.
It’s your hair. You can do whatever you want with it after. You can rock the bald look. You can wear hats or wigs. You can do whatever you want because it’s your head.
»MORE: Dealing with hair loss during cancer treatment
Was there a point when you had to advocate for yourself?
It happened a couple times. I was throwing up so much more than normal. I couldn’t even keep water down. I couldn’t walk across my house without getting nauseous.
I knew it wasn’t normal. I felt like my home health nurse brushed it off at first. I pushed, and that’s when I forced them to admit me back to the hospital because I knew something was wrong.
Turns out, the calcium levels in my blood were way too high. That can cause severe nausea and vomiting. I had to speak up for myself.
I had to make them understand the severity of it because they see chemo patients vomiting all the time. That’s when the nurse finally put me on Ativan, which helped so much.
»MORE: How to be a self-advocate as a patients
What’s your advice for someone who’s nervous about standing up for themselves?
Honestly, suck it up and just do it. You have to be an advocate for yourself. You can tell your nurse if something is going on. We have patients sometimes who hide symptoms they’re having because they don’t want to go through more tests. That’s the worst thing you can do. It delays your care.
If you’re feeling too sick or scared to stand up for yourself, find someone who can do it for you. That can be a nurse you have a bond with, a family member, friend or anyone [who can] advocate for you.
You have to speak up about things that are going wrong, that you’re uncomfortable with or things that are hurting. You really are the champion of your own care. You have to be.
Preserving fertility using Lupron shots
I hadn’t been having a period for a few months before I was diagnosed. They put me on lupron shots to protect my fertility. It puts you in a temporary menopause, so I continued to not have one.
I had hot flashes and all the other general symptoms of menopause. It’s kind of funny now because my old coworkers or aunts will complain about hot flashes or something, and I’ll say, “Yeah, I know how you feel.” They usually give me a weird look, but I really do.
My period did come back. As far as I’m aware, everything is normal now. I’m not 100% sure about fertility. I’m still kind of on the fence about kids.
»MORE: Fertility preservation and cancer treatment
What is your “new normal” after cancer?
Obviously my career. I wouldn’t have it without having gone through cancer. I haven’t changed much day to day in what I do. I’ve always tried to eat healthy and work out.
In a negative way, there’s always the thought that pops up and says, “Hey, you had cancer. It could come back.” I have to deal with those things occasionally.
The thoughts get quieter, and things get easier to deal with as time goes on. Now when that thought pops up, I can reassure myself that it’s okay.
It took until recently to really feel at peace with everything. It took me a while to not feel angry. Now that I feel at peace, it feels better than it did before I got sick.
Support
How important was it to have a support system around?
It was the most important thing in getting me through everything.
I have aunts and uncles on both sides of the family. I have a lot of cousins I’m close with. I don’t have a ton of friends, but I have very close friends. They were the key to getting through it. I didn’t always share my feelings as much as I should have. I kept a lot of them bottled up, especially the fear and anger. I kept a journal with all those thoughts.
It was so nice to have people visit, send food and bring cards. It made me feel like I had a lot of people looking out for me.

Was it hard for you to ask for support?
It was hard for emotional support. It was easy to ask for rides to the doctor, food and stuff like that.
It was hard for me to open up emotionally and tell people, “I’m really scared today.” I couldn’t tell them things like, “I had a nightmare last night that my doctor told me the cancer spread to my brain and that there was nothing they could do.” That’s the kind of stuff I didn’t tell people.
Did you ever feel isolated?
I felt so isolated the whole time. Even though I had all these people around me who wanted to help and empathize, I felt like nobody really knew what I was going through.
My diagnosis isn’t a common one. I did find a mentor from Imerman Angels. It’s a mentor/mentee program. They set me up with a girl who was my age, had my exact same treatment, diagnosis and everything.
I emailed back and forth with her. That was easier because she understood firsthand what it was like. We still email some days.
I also met a guy in the hospital. He had a different leukemia diagnosis. He was the only one besides me that was in his 20s. We formed a little bit of a bond while we were in the hospital. It was nice to have people who really knew.
Then during radiation specifically, I felt isolated because the support system faded. They were still there, but kind of off to the side. I looked better, so they didn’t think about it as much.
I was dog sitting at the time, so I was driving myself to radiation and driving back to a big empty house with a dog instead of being at home with my family. I was spending a lot of time alone.
Paying for cancer treatment
I was out of work (for one year). I was lucky to be young enough to still be on my parents’ insurance. My dad has incredible insurance. It was really a blessing to have that.
I had a large amount of savings from a lawsuit I won after a car accident a few years beforehand. All this bad stuff happened, but everything really was a blessing in disguise.
If you’re having financial difficulty, reach out to your social worker on your oncology team.
Look online. Check out the Leukemia and Lymphoma Society. They could have resources for you. Look into other cancer cancer foundations and co-pay assistance programs.
There are even programs to help you get to and from the doctor. There are prescription help programs. There’s a lot out there, but you just have to look for it.
Do you have any advice for someone who has just been diagnosed?
Don’t Google things. You will read the worst statistics that probably don’t even apply to you. You will dig yourself into a hole of fear and depression that is very hard to get out of.
You can do this. You just have to take it one day at a time. Trust in your team and the people around you to take care of you. Try to take care of yourself, but if you can’t, know there are people who will surround you and help when you can’t do it on your own.
Allow yourself to feel however you need to feel. Don’t bottle up emotions. Don’t try to hide. Don’t try to pretend that you’re happy or fine when you’re not. Your feelings are valid and need to be expressed. You’re allowed to feel scared.
You’re allowed to cry into your ice cream after you’re told you’re in remission. You don’t have to be the happy, strong cancer warrior all the time.
Inspired by Brianna's story?
Share your story, too!
Anaplastic Large Cell Lymphoma (ALCL) Stories
Brianna B., Anaplastic Large Cell Lymphoma (ALCL)
1st Symptoms: Infections, inflammation, high fever, swelling, abdominal pain
Treatment: Chemo, radiation
...

One reply on “Brianna’s Stage 2B ALK+ ALCL Non-Hodgkin’s Lymphoma Story”
I liked to hear your story, my daughter has a 24 year old friend and she was diagnosed with anaplastic large cell lymphoma and she has hard time to find a support group. Where could we find young people like Brianna to contact and talk about the cancer experience. She is so scared.