Monica’s Stage 2B IDC Breast Cancer & Undifferentiated Pleomorphic Sarcoma Story
Monica shares her stage 2B breast cancer story, as well as getting diagnosed with a second cancer, a soft tissue sarcoma. Overall, she describes getting through multiple surgeries like oncoplasty, chemotherapy, and radiation therapy.
In her story, Monica talks about how she navigated life after 2 cancer diagnoses, including managing hair loss, setting up the right support around her, and how she got through that second cancer.

- Name: Monica H.
- Diagnosis:
- Breast cancer
- Invasive ductal carcinoma (IDC) of left breast at age 37
- Second primary cancer diagnosis: Sarcoma
- Undifferentiated pleomorphic sarcoma (UPS) of the same pectoral muscle at 39
- Breast cancer
- Staging: 2B
- 1st Symptoms:
- Tightness in breast
- Lump
- Treatment:
- Surgeries
- Oncoplastic surgery (lumpectomy with reconstruction)
- Hysterectomy
- Single radical mastectomy w/ DIEP flap
- 4 additional surgeries to try to salvage breast
- Chemotherapy
- AC-T: Adriamycin, Cytoxan, Taxol
- 4 rounds of AC followed by 4 rounds of T
- AC-T: Adriamycin, Cytoxan, Taxol
- Radiation
- Targeted to left chest
- Surgeries
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.

Don’t give up. It’s not the end. With today’s medical advances, you’re in good hands. Don’t get depressed. Laughter is great medicine.
Don’t go to message boards, because those people are usually talking about horror stories.
Find a Facebook group or something like The Patient Story. Ask your nurses for help and resources.
Monica H.
Diagnosis
What were the first symptoms?
I was working with a physical therapist on strengthening and getting back my range of motion in my left shoulder after some unrelated injuries. I got on my foam roller one night that I had this tightness.
I felt around it, and I thought, “I’m 36. It’s probably just a knot.” I had talked to my twin sister and a friend, and they said during their cycles, they got knots sometimes. I just brushed it off.
I showed my sister on a family trip because I still had it. She felt and it, and her response was, “What the F, Monica?”
We got back into town, and I waited for my cycle to end in case that’s what it was. It ended, and the knot was still there, so I called my doctor’s office.
What scans did you undergo?
I said, “Hey I have a spot in my breast. My sister is kind of paranoid about it.” They had me come in the next day.
We went in on a Friday to the office. They felt it, and within 10 minutes, they called up to the hospital and made me an appointment to walk in for an ultrasound and mammogram.
I walked across the street and got the scans done. About 4 hours later, they pulled my mom in and told us it wasn’t good news.
They said they couldn’t officially say, but they wanted to do a biopsy. We had a trip to Hawaii planned, and I wouldn’t be able to go if we did the biopsy right away, so they told me to go ahead and go.
Surgical biopsy and diagnosis
I had a surgical biopsy because the tumor was big. On November 2nd, they gave me the news I didn’t want to hear. It was a little bit of a shock. They stepped out for a minute and let us pull ourselves together.
My mom had just had stage 0 breast cancer, invasive ductal carcinoma (IDC). We were asking, “Okay, so can we just do the same thing she did?” They were like, “No. No. No.”
»MORE: Patients share how they processed a cancer diagnosis
Appointments, scans, blood work
Over the next 8 business days, I had meetings with the oncologist and surgeons, and I had scans, blood work, and everything.
The doctor said it was aggressive. They said every time I had my period, I was feeding the cancer. I saw my OB/GYN.
All my doctors wanted to start me on chemo right away, but that’s not how insurance companies work. I was pretty much living at the hospital, getting myself ready for treatment.

Discussing treatment plans with medical team
They said even with a mastectomy, I would need chemo. I had a really awesome doctor. He sat there with a chart and showed us the good and bad.
I was pretty much 95% on the bad side. He explained exactly why we had to treat it the way we did.
He laid it all out for us. We talked about fertility as well on the 2nd.
They told me if I took the time to freeze my eggs that I’d be stage 4 and writing my will by Thanksgiving. By November 16th, I started chemo.
Breast Cancer Treatment
Describe the chemo regimen
I had to do 4 rounds of AC and 4 rounds of Taxol. I had a double dose, basically. They needed to blast it.
Getting a port
I started off without a port, but after the first 2 treatments taking hours to get to my veins, my nurses told my doctor I needed one.
AC-T chemo side effects
Summary: nausea, diarrhea, weight loss, shortness of breath
During the AC (Adriamycin and Cytoxan), I had a lot of nausea and a lot of diarrhea. I only threw up once, though.
I popped Zofran as soon as I started feeling it coming on, and that really helped me. The stomach issues were hard, though.
I had some weight loss. I was at a healthy weight when I started treatment, but then I lost 20 pounds. They told me to try to stop losing weight because it’s better to have some fat when you’re going through chemo.
The biggest side effect I had from Adriamycin was in my wrist and forearm from the IV treatments before my port. I had some bruising and pain.
It took me about 6 months for my veins to recover. It felt like a deep bone bruise. I couldn’t put any pressure on my arms for a long time.
I also had some trouble breathing each time they would infuse Taxol. When they first start it, you can get some shortness of breath. That happened, and they had to stop the infusion and let me meditate and get my mind right and catch my breath for a minute. They had to up my steroids, so I was wired and constipated constantly.
Taxol did a number on me. I went in for Taxol on January 11th. Then 2 days later, I went downstairs after waking up at home, and I told my mom, “I don’t feel so good.”
I went to the bathroom, and I was crying because I couldn’t go. I was trying to drink hot water, squat, and do anything I could.
After an hour or 2, I finally went. Not to be too graphic, but it was the size of a basketball. My mom was like, “Oh my gosh, oh my gosh.”
We had to call the doctor. They said to just lay me down. They reassured us it was the Taxol.
After a while, I couldn’t feel from my waist down, and my fingertips had gone to sleep. We called the doctor. They said, “Put some pressure on your nerves.” After my next round, the neuropathy was getting worse. There wasn’t really anything they could do because I needed that drug.
After the third round, I woke up and came downstairs. My sister was like, “What’s wrong with you? You’re talking funny.” I was drooling. I couldn’t feel my face when they were tapping my face. We called the doctor again. They did a head scan and everything, and it was just a side effect.
I had some facial paralysis for a while. We had to delay my last chemo treatment. I had my last dose on February 24th. I still have some bone pain and neuropathy as a lasting side effect. I wound up getting on some medication from that.
»MORE: Cancer patients share their treatment side effects
You had an oncoplastic surgery
I opted to do an oncoplasty. That’s where they do a lumpectomy with reconstruction at the same time. The prep was pretty easy. I had to meet with a plastic surgeon about sizing and all that.
They did a really good job with my surgery. They removed the tumor and a couple lymph nodes. The scars are close together, and I was happy with the way they did it.
The only thing before surgery that was hard wasn’t even related to my surgery. The surgery before mine ran long, and I had a midday surgery, so I hadn’t eaten in like 14 hours.
When they finally got me back for surgery, I was just ready to have it over with. I was a little nervous, but it wasn’t bad because I was just ready for it to be done.
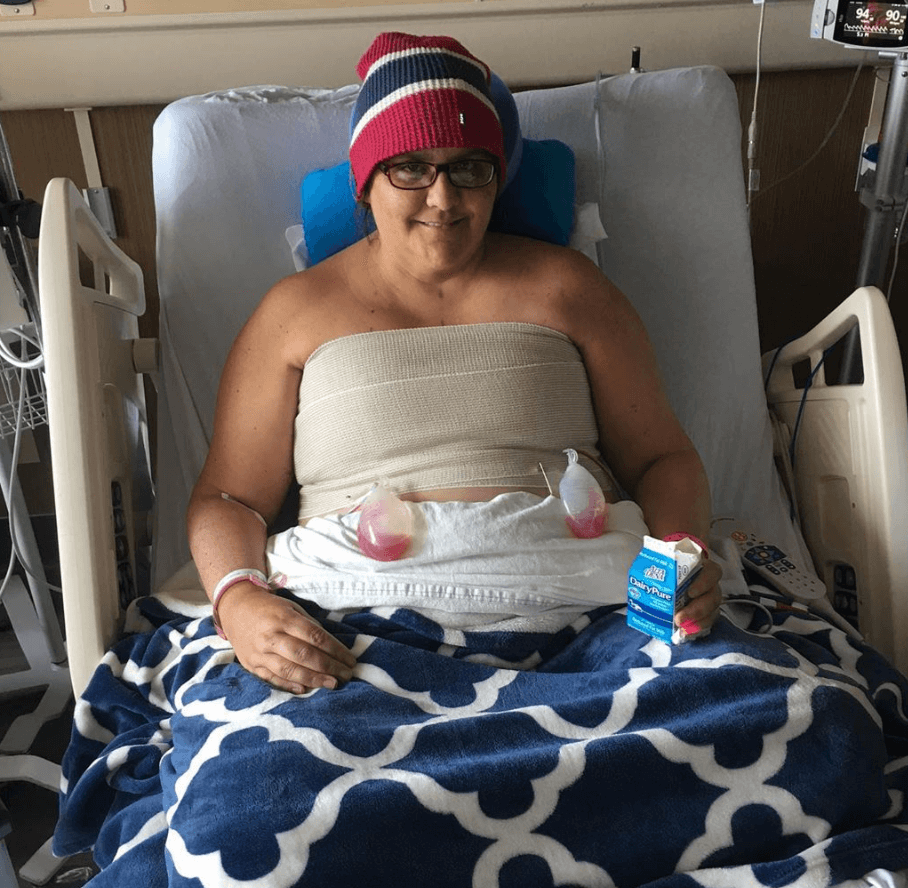
I remember waking up and seeing my mom and my sister mumbling. The nurses and doctors told me they could take me home, but it was already midnight or so by the time I woke up, so they advocated for me and told them I was staying the night at the hospital.
That helped my recovery. I was thankful the hospital didn’t argue. Having the morphine every few hours helped so much.
The only thing that scared me was preparing to see the drains. It was a little uncomfortable and painful, but I got through that. The drains freaked me out, though.
I thought I was going to pass out when he went to take them out, but it took about 30 seconds. It just felt like someone took a wet finger and swiped it across me.
Describe the radiation therapy
I did 35 rounds of radiation. I started on Memorial Day and ended on July 11th, 2016. The day I had my last treatment was the day I was considered in remission as well.
We noticed during radiation therapy that I was snoring a lot during the night. They radiated my breasts, but it also reached up into my throat, so the snoring was a side effect of that.
Radiation wasn’t too terribly bad. I used Aquaphor to try to calm my skin. It was going well until the last week of radiation, when I got some redness.
The worst part of radiation wasn’t actually the process itself. I had a male nurse who ripped one of my stickers off in the radiated area instead of carefully taking it off.
That was more painful than surgery. I remember going back to put my clothes on, and I couldn’t. It was burning so bad.
The nurse had given me a first degree burn when he did that. I ended up needing wound care for a few weeks after that.
Out of everything other than chemo, that was the most painful. He got a slap on the wrist for that one.
»MORE: Read other patient experiences with radiation therapy
Describe the hysterectomy
I started on hormone meds about a month after chemo in April. I did Arimidex for a while. I don’t remember having bad hormonal issues like trouble sleeping, sweating, and hot flashes from the Arimidex specifically.
I was already having issues with that stuff from my chemo and just the weather anyways because it was hot outside.
Describe the hormone therapy (Lupron)
When I started chemo, I had to go on the Lupron shot. I had already experienced being on some type of medication for hormones, so I didn’t really notice a difference when I started on Arimidex.
The longer I was on the hormone medications, the more I was having severe migraines — about once a month. I told my doctor I didn’t want to do it anymore. In April 2018, he said we could go ahead and do a hysterectomy. They took everything — my uterus, my ovaries, all of it.
Second Primary Cancer
Getting a second cancer
Getting cancer once is hard enough, but getting cancer a second time is even more shocking. I was diagnosed with a separate primary cancer. This time it was sarcoma. I was diagnosed in fall of 2018.
I was going in to see my oncologist because I was ready for reconstruction. I was due for a scan in December, and he asked if I wanted to just go ahead and do it instead of waiting until after surgery when it might be more painful.

We did the scan on Friday. Monday was Labor Day, and on Tuesday, I got a call from my breast cancer navigator. She said, “Monica, I need you to come in. Your scan. I’m sorry.”
I said, “It can’t be back. You’re wrong.” I had to go in that day. I was even more in denial than the first time around.
I had to call my parents. I felt like a little kid when I told my mom. I just kept saying, “Mom, mom. My cancer’s back.”
They did a scan again and a biopsy and confirmed it. They went to get my mom, and they told us they needed more testing.
I had to come in for another biopsy, and that one was a little tricky.
What was the needle biopsy for sarcoma like?
It was a really scary procedure actually. I had to be so still because it was right near my ribs, and if I moved, they could accidentally poke my lung. I had to lie on my side, and the nurse had to hold me.
One little error, and she could hit my lung. I knew what to expect from the biopsy, so I was pretty calm. I was extra numb, too, because the radiation oncologist who would up doing the biopsy even admitted she was a little nervous because it was so deep.
They called me later and said they couldn’t get a reading on it. They had to send it somewhere in Boston. The results came back, and it was undifferentiated pleomorphic sarcoma (UPS) in my pectoral muscle.
Describe the radical mastectomy with a DIEP flap
My hospital had a tumor board, and I was one of the discussions on the board. My surgery was going to be 12 to 15 hours. They were trying to plan it out at a time when they could have enough staff available for that major of a surgery. They found out a weekend that worked.
Unfortunately, I had to go on a cleanse for a few days before surgery since I was getting a DIEP flap. That wasn’t fun. I did the other prep as well, like getting a marker in my chest. The prepping before was pretty tough because I couldn’t eat for 4 days.
I had the radical mastectomy on my left side and DIEP flap on October 20, 2018.
How was recovery from the mastectomy surgery?
I was in the hospital for a good week. My first day without the intubation tube in the ICU, I vomited all over my uncle. That’s why they tell you not to eat before surgery.
I was out of it for about 3 days. I remember waking up in a warm blanket. I felt like I was in a cocoon because they had kind of wrapped me up in it since they didn’t want me to move a whole lot.
I had a drain in each side of my chest, one in each hip, and one in each side of my vagina. I didn’t know that was going to happen. That was the most uncomfortable thing.
A week into the hospital stay, I finally was able to eat.
They were bringing me food, and a nurse came to check on me. My numbers were spiking. They found out I had some fluid building up in my lungs, and I had to have emergency surgery. I was in the hospital until November 2nd.
You had complications from surgery
I had to have surgery on my surgical breast in January 2019 because I had an infection. My radiated skin was having trouble healing well. Then in April 2019, I had another surgery because of the open wounds and some fat necrosis.
I went through so much to try to get that breast to take, and I just couldn’t take it anymore. In August 2018, I told my doctor to just take the breast out. I wanted it over with.
In September, he went in, took all the dead tissue, and added fat from my back into my chest. That surgery has taken so far.
We’re celebrating that win right now.
Reflections
How are you doing now?
I’ve found a support group recently. My mom and my sister go with me. I thought it was only for people who’ve lost a spouse or child, but for me, I’m grieving the ability to have children. I’m doing things like that.
I’m going to art classes at the hospital because it’s such great therapy. I’m going to start swimming PT soon because it’s good for neuropathy and bone pain.
Can you talk more about your support system?
My parents and sister are everything. I’ve been ghosted by a lot of my friends, even my best friend.
One of the friends who has been there for me lives in Sacramento. She comes down every 6 months or so.
A lot of my friends I played softball and volleyball with have been a disappointment. I’ve always been the friend you can lean on, but when I need something, they’re MIA.
I’ve vented about that at my support group. If they were true friends, they would come see me, so I just try to let it go.
My sister’s boyfriend is great, too. He comes in and cooks, cleans, and supports her. I appreciate that so much.
»MORE: What kind of support cancer patients say helped the most

Describe the hair loss after cancer treatment
I had a haircutting party. I cut off like 13 inches. Then I started getting a headache when it started falling out, so we buzzed it.
After the second chemo treatment, it was just so itchy, so I had to shave it. I was so happy I didn’t have an egg-shaped head when we shaved it.
»MORE: Dealing with hair loss during cancer treatment
After that, it was kind of liberating. I’m a little bit of a tomboy, so I rocked the beanies. We threw a hat party, and I got so many. I was really comfortable with it.
Do you have any advice for someone who has just been diagnosed?
Don’t give up. It’s not the end. With today’s medical advances, you’re in good hands. Don’t get depressed. Laughter is great medicine.
Don’t go to message boards because those people are usually talking about horror stories. Find a Facebook group or something like The Patient Story. Ask your nurses for help and resources.

Inspired by Monica's story?
Share your story, too!
Invasive Ductal Carcinoma Stories
Amelia L., IDC, Stage 1, ER/PR+, HER2-
Cancer details: IDC is most common kind of breast cancer.
1st Symptoms: Lump found during self breast exam
Treatment: TC chemotherapy; lumpectomy, double mastectomy, reconstruction; Tamoxifen
Rachel Y., IDC, Stage 1B
Cancer details: IDC is most common kind of breast cancer. Stage 1B.
1st Symptoms: None, caught by delayed mammogram
Treatment: Double mastectomy, neoadjuvant chemotherapy, hormone therapy Tamoxifen
Rach D., IDC, Stage 2, Triple Positive
Cancer details: IDC is most common kind of breast cancer.
1st Symptoms: Lump in right breast
Treatment: Neoadjuvant chemotherapy, double mastectomy, targeted therapy, hormone therapy
Caitlin J., IDC, Stage 2B, ER/PR+
Cancer Details: ER/PR positive = estrogen and progesterone receptor positive
1st Symptoms: Lump found on breast
Treatment: Lumpectomy, AC/T chemotherapy, radiation, and hormone therapy (Lupron and Anastrozole)
Joy R., IDC, Stage 2, Triple Negative
Cancer details: Triple negative doesn’t have any receptors commonly found in breast cancer making it harder to treat
1st Symptoms: Lump in breast
Treatment: Chemo, double mastectomy, hysterectomy
Callie M., IDC, Stage 2B, Grade 2, ER+
Cancer Details: ER positive = estrogen receptor positive
1st Symptoms: Dimpling/lump found on breast
Treatment: Mastectomy, AC/T chemotherapy, hysterectomy, reconstruction
Monica H., IDC, Stage 2B & Undifferentiated Pleomorphic Sarcoma
Cancer details: IDC is most common kind of breast cancer.
1st Symptoms: Tightness and lump in left breast
Treatment: Chemotherapy, radiation, surgery
Stefanie H., IDC, Stage 3, Triple Positive
Cancer details: IDC is most common kind of breast cancer. Triple positive = positive for HER2, estrogen receptor (ER), progesterone receptor (PR)
1st Symptoms: Lump in breast
Treatment: chemotherapy, lumpectomy, radiation
Doreen D., IDC, Stage 2A, Triple Positive
Cancer details: IDC is most common kind of breast cancer. Triple positive = positive for HER2, estrogen receptor (ER), progesterone receptor (PR)
1st Symptoms: Lump in left breast
Treatment: Neoadjuvant chemotherapy (TCHP), lumpectomy, radiation
Melissa H., Stage 2B, Triple Negative
Cancer details: Triple negative doesn’t have any receptors commonly found in breast cancer making it harder to treat
1st Symptoms: Lump in left breast
Treatment: Mastectomy, chemotherapy, 2nd mastectomy
Genoa M., IDC, Stage 3, HER2+
Cancer details: HER2-positive tends to be more aggressive than HER2-negative cases
1st Symptoms: Nausea
Treatment: Chemotherapy, radiation
Andrea A., IDC, Stage 2B/3, ER+
Cancer details: Found cancer while pregnant
1st Symptoms: Divot in breast
Treatment: Chemotherapy, radiation, surgery
Stephanie J., Stage 3, Triple Negative, BRCA1+
Cancer details: Triple negative doesn’t have any receptors commonly found in breast cancer
1st Symptoms: Lump in left breast
Treatment: Chemotherapy, surgery
Renee N., IDC, Stage 3-4, HER2+
Cancer details: IDC is most common kind of breast cancer.
1st Symptoms: Lump in breast
Treatment: chemotherapy, bilateral mastectomy, radiation
Shari S., Stage 4, Metastatic, Triple Positive
Cancer details: Triple positive = positive for HER2, estrogen receptor (ER), progesterone receptor (PR)
1st Symptoms: Lump in breast
Treatment: Surgery, chemotherapy, radiation
Erin C., IDC, Stage 2B/4, Metastatic, Triple Negative
Cancer details: Triple negative doesn’t have any receptors commonly found in breast cancer making it harder to treat
1st Symptoms: Pain in breast
Treatment: Surgery, chemotherapy, radiation
Margaret A., IDC & DCIS, Stage 2B
Cancer details: IDC is most common kind of breast cancer. DCIS means cancer has not spread into surrounding breast tissue
1st Symptoms: Pain in left breast, left nipple inverting
Treatment: Double mastectomy, chemo (AC-T), Radiation
Abigail J., Stage 4, Metastatic
Cancer Details: HER2-low, node negative, PIK3CA mutation
1st Symptoms: Back and leg pain, lump in breast
Treatment: Surgery, chemotherapy, radiation, CDK4/6 inhibitors
Bethany W., Stage 2, ER+
Symptoms: Lump in breast and armpit
Treatment: Chemotherapy, double mastectomy, radiation
Bethany W., Stage 4 Metastatic
Symptoms: Lower back pain
Treatment: Chemotherapy, radiation, maintenance treatment
Lainie J., IDC, Stage 2, HER2+
Symptoms: Lump in breast
Treatment: Chemotherapy, double mastectomy, radiation





















